تعرف على أفضل طرق علاج تضيق الشريان الأبهري بواسطة جراحة مجازة الشريان الأبهر والتي تتم على يد أمهر أطباء الجراحة القلبية والوعائية في تركيا.
تعريف جراحة مجازة الشريان الأبهر
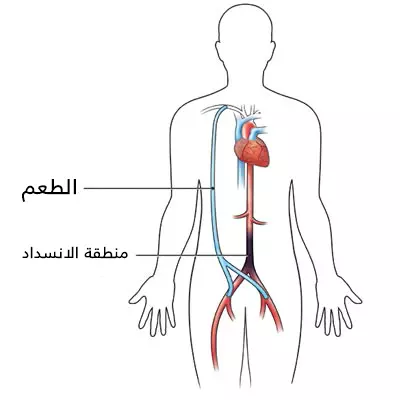
توضع أنابيب صناعية (طعوم) بالقرب من جزء من الأوعية الدموية المسدودة أو الضيقة. تخلق مسارًا بحيث يمكن للدم أن يتحرك حول الانسداد. في هذه الحالة، يتم وضع الطعوم على مسار الشريان الأبهري والشريان الحرقفي أو الفخذ.
الشريان الأبهري هو الشريان الرئيسي الذي يغادر القلب. يجلب الدم الغني بالأكسجين إلى الجسم. عند مستوى السرة تقريبًا، ينقسم الشريان الأبهري إلى شريانيين حرقفين. على مستوى الفخذ، تصبح الشرايين الحرقفية هي الشرايين الفخذية.
يُطلق على جراحة مجازة الشريان الأبهر مع الفخذيين أيضًا اسم البطال الأبهري. هذا لأنها تكون على شكل “y” مقلوب.
تتضمن معظم جراحات المجازة شقًا مفتوحًا تقليديًا. يتم إجراء الأبحاث حول كيفية إجراء هذه عمليات من خلال تقنيات التنظير البطني أو بضع البطن المصغر. حيث يتم استخدام شقوق أصغر بكثير.
أسباب إجراء جراحة مجازة الشريان الأبهر
للحصول على تدفق دم جيد إلى الجزء السفلي من الجسم، يجب أن يكون هناك تدفق دم جيد عبر الأبهر والشرايين الحرقفية وشرايين الفخذ. تصلب الشرايين مرض تتراكم فيه البقع اللاصقة (لويحات) على طول جدران الأوعية الدموية. تمنع هذه اللويحات التدفق الطبيعي للدم داخل الأوعية الدموية المصابة. عندما ينخفض تدفق الدم، لا تتلقى الأنسجة الموجودة على الجانب الآخر من الانسداد ما يكفي من الأكسجين. يمكن أن يؤدي هذا إلى ما يلي:
- الألم الذي يزداد كلما طالت مدة المشي أو ممارسة الرياضة (يسمى العرج المتقطع)
- برودة القدمين أو الساقين
- تقشر، جفاف، احمرار، حكة، جلد بني على الساقين أو القدمين
- تقرحات غير ملتئمة و / أو مصابة بالإنتان على ساقيك أو قدميك
- الغرغرينا
- ضرورة بتر الساق
- تلف الأعصاب
يمكن ل جراحة مجازة الشريان الأبهر أن تعيد تدفق الدم إلى الساقين
المضاعفات المحتملة لجراحة مجازة الشريان الأبهر
المشاكل من هذا الإجراء نادرة، لكن جميع الإجراءات تنطوي على بعض المخاطر. سيراجع طبيبك المشاكل المحتملة، مثل:
- عدوى
- انسداد المجازة الجديدة عن طريق الجلطات الدموية
- نزيف
- مضاعفات التخدير
- تندب
- تلف الأعصاب
قبل الإجراء، تحدث إلى طبيبك حول طرق إدارة العوامل التي قد تزيد من خطر حدوث مضاعفات مثل:
- التدخين
- الكحول
- الأمراض المزمنة مثل السكر أو السمنة
أنواع جراحة مجازة الشريان الأبهر
تعد جراحة المجازة الشريانية الفخذية الخيار الأفضل للانسداد الذي يقيد تدفق الدم إلى الشريان الفخذي. ومع ذلك، هناك إجراء آخر يسمى المجازة الفخذية الإبطية والذي يمكن استخدامه في بعض حالات جراحة مجازة القلب.
تضع المجازة الفخذية الإبطية ضغطًا أقل على القلب أثناء جراحة القلب والصدر. كما أنه لا يتطلب فتح بطنك أثناء إجراء جراحة مجازة الشريان الأبهر. هذا لأنه يستخدم طعمًا أنبوبيًا بلاستيكيًا باسم طعم مجازة الشريان الأبهر ويربط الشرايين الفخذية في ساقيك بالشريان الإبطي في كتفك. ومع ذلك، تعد الجراحة المستخدمة في هذا الإجراء أكثر عرضة لخطر الانسداد والعدوى والمضاعفات الأخرى لأنه تنتقل لمسافة أكبر ولأن الشريان الإبطي ليس بحجم الشريان الأبهري. يرجع السبب في زيادة خطر حدوث مضاعفات إلى عدم دفن الطعم بعمق في الأنسجة ولأن المجازة أضيق في هذا الإجراء.
ماذا تتوقع عند ترتيب الخضوع لجراحة مجازة الشريان الأبهر
قبل الإجراء قد يقوم طبيبك بما يلي:
- فحص سريري
- تحاليل الدم
- مؤشر الكاحل والعضد -يقارن هذا الاختبار قياسات ضغط الدم في ذراعيك وساقيك. يجب أن تكون هذه الأرقام متشابهة جدًا. إذا كانت القيم في ساقيك أقل بكثير من تلك الموجودة في ذراعيك، فهذا يشير إلى وجود انسداد في الشرايين التي تنقل الدم عبر ساقيك.
- الموجات فوق الصوتية دوبلر -يستخدم هذا الاختبار الموجات الصوتية لفحص تدفق الدم في الشرايين. يمكنه تحديد الشرايين المسدودة.
- تصوير الأوعية الدموية -يتم حقن صبغة في الشرايين والتقاط صور بالأشعة السينية لساقيك. نظرًا لأن الصبغة لن تكون قادرة على التدفق عبر المناطق الضيقة أو المسدودة بواسطة اللويحات، فسيتم تحديد الموقع المحدد للانسدادات. تشمل الأنواع الأخرى من تصوير الأوعية طفيف التوغل المستخدمة حاليًا أيضًا تصوير الأوعية بالتصوير المقطعي المحوسب وتصوير الأوعية بالرنين المغناطيسي.
قبل إجراء جراحة مجازة الشريان الأبهر:
- لا تأكل أو تشرب أي شيء بعد منتصف الليل في الليلة التي تسبق جراحة فتح مجرى جانبي للشريان.
- رتب للحصول على المساعدة في المنزل بعد عودتك من المستشفى.
- رتب أن يكون هناك شخص ما يقودك إلى المنزل عندما تغادر المستشفى.
تحدث إلى طبيبك عن أدويتك. قد يُطلب منك التوقف عن تناول بعض الأدوية لمدة تصل إلى أسبوع قبل الإجراء.
وصف إجراء جراحة مجازة الشريان الأبهر
سيتم عمل شق كبير في بطنك. سيتم قطع العضلات حول بطنك. للوصول إلى الشريان الأورطي البطني، يجب نقل بعض الأعضاء بعناية بعيدًا عن الطريق.
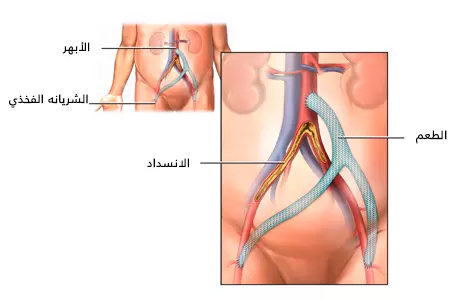
سيتم إيقاف تدفق الدم عبر الأوعية لفترة وجيزة. سيتم وضع المشابك على جانبي المنطقة المسدودة لوقف تدفق الدم. سيتم خياطة المجازة في مكانها. سيتم تحويل مسار الشريان التاجي عن طريق ربط أحد طرفيها بالشريان الأبهري الموجود فوق الانسداد مباشرةً. وربط الطرف الآخر مباشرة بعد الانسداد على الشرايين الفخذية أو الحرقفية.
ستتم إزالة المشابك. سيراقب الطبيب للتأكد من وجود تدفق دم جيد عبر المجازة. ستعود أعضائك الداخلية إلى مكانها. سيتم شد عضلات البطن معًا. سيتم خياطة العضلات لإغلاقها. سيتم إغلاق شق الجلد إما بالخيوط الجراحية أو الدبابيس.
بعد عملية جراحة مجازة الشريان الأبهر
بعد الجراحة، سيتم نقلك إلى غرفة الإنعاش. يمكن إزالة الأنبوب الموجود في حلقك، أو قد يحتاج إلى البقاء فيه لبضعة أيام. قد يستمر التخدير فوق الجافية أيضًا لبضعة أيام. ستتم مراقبتك بحثًا عن أي ردود فعل سلبية للجراحة أو التخدير.
كم سيؤلم؟
التخدير سيمنع الألم أثناء الجراحة. يمكن السيطرة على الألم وعدم الراحة بعد العملية بالأدوية.
متوسط الإقامة في المستشفى
المدة المعتادة للإقامة هي 5-7 أيام. سيعتمد الطول على صحتك العامة وسرعة شفائك. قد يختار طبيبك إبقائك لفترة أطول إذا ظهرت مضاعفات.
رعاية ما بعد عملية جراحة مجازة الشريان الأبهر
في المستشفى
ستحتاج إلى قضاء يوم أو يومين في السرير بعد العملية.
- ستتم مراقبتك بعناية في وحدة العناية المركزة (ICU).قد تكون هناك لمدة يوم أو يومين حسب الحاجة.
- مقياس التنفس التحفيزي، سيتم استخدامه كل ساعتين خلال اليوم. سيبقي ذلك رئتيك مفتوحتين قدر الإمكان ويساعد على تجنب الالتهاب الرئوي.
- يمكن وضع أنبوب أنفي معدي (NG)أثناء العملية. يتم وضع الأنبوب في أنفك وصولاً إلى معدتك. غالبًا ما تتوقف أمعائك عن العمل بشكل طبيعي بعد الجراحة. لن تتمكن من تناول أي شيء عن طريق الفم حتى يبدأ في العمل مرة أخرى. سيتم بعد ذلك إزالة أنبوبNG. سوف تتقدم ببطء من نظام غذائي سائل، إلى نظام غذائي للأطعمة اللينة، وأخيراً إلى نظام غذائي منتظم.
- قد يتم إعطاؤك أيضًا أدوية يومية للمساعدة في تجنب تجلط الدم.
أثناء إقامتك، سيتخذ طاقم مستشفى قسم جراحة القلب خطوات لتقليل فرصة الإصابة بالعدوى، مثل:
- غسل أيديهم
- لبس القفازات أو الأقنعة
- الحفاظ على جروح العمل الجراحي مغطاة بضماد
هناك أيضًا خطوات يمكنك اتخاذها تهدف لتقليل فرص الإصابة مثل:
- غسل يديك بشكل متكرر وتذكير الزوار ومقدمي الرعاية الصحية بفعل الشيء نفسه
- تذكير مقدمي الرعاية الصحية بارتداء القفازات أو الأقنعة
- عدم السماح للآخرين بلمس الجرح
في البيت
قد يستغرق التعافي ما يصل إلى 6 أسابيع. توقع أن ترى تحسنًا كبيرًا في قدرتك العامة على المشي أو ممارسة الرياضة. عندما تعود إلى المنزل، ستحتاج إلى الحفاظ على الجرح نظيفًا لمنع العدوى. يمكن السيطرة على الألم بالأدوية. قد تتم إحالتك إلى معالج فيزيائي للحفاظ على قوتك أو إعادة بنائها.
ماذا تتوقع بعد جراحة مجازة الشريان الأبهر
ثمانون في المائة من جراحات المجازة الأبهرية الفخذية تفتح بنجاح الشريان وتخفف الأعراض لمدة 10 سنوات بعد العملية. يجب أن يخف ألمك عندما تكون مستريحًا. يجب أيضًا أن يختفي الألم أو يقل بشكل كبير عند المشي. سيكون انذارك أفضل إذا كنت لا تدخن أو تقلع عن التدخين قبل جراحة تطعيم مجازة الشريان الأبهر.
اتصل بطبيبك بعد جراحة مجازة الشريان الأبهرعند
من المهم مراقبة تعافيك. نبه طبيبك إلى أي مشاكل. في حالة حدوث أي مما يلي، اتصل بطبيبك:
- علامات العدوى بما في ذلك الحمى والقشعريرة
- احمرار، تورم، ألم متزايد، نزيف مفرط، أو أي إفرازات من موقع الجرح
- الغثيان أو القيء المستمر
- ألم لا يمكنك السيطرة عليه بالأدوية التي أعطيت لك
- ألم أو حرقة أو إلحاح أو كثرة التبول أو نزيف مستمر في البول
- سعال أو ضيق في التنفس أو ألم في الصدر
- تصبح ساقك باردة، أو شاحبة، أو زرقاء، أو وخز، أو خدر
- ألم أو تورم في ساقيك أو ربلتيك أو قدميك
إذا كنت تعتقد أن لديك حالة طارئة، فاتصل بالخدمات الطبية الطارئة على الفور.