في حالة الضعف الشديد أو غياب وظائف الكلى ، من الضروري إجراء تحويلة غسيل الكلى بانتظام عبر ماكينة غسيل الكلى (غسل الدم) في مركز غسيل كلى , حتى تستطيع المنتجات الأيضية والمواد الضارة التي تنقلها الكلى إلى مجرى دم المريض من مغادرة الدم.
أسباب جلسات غسيل الكلى
هناك عدة أسباب لتلف الكلى تجعل من الممكن توصيل ماكينة غسيل الكلى الاصطناعية مثل الفشل الكلوي المزمن (المرحلة النهائية من الفشل الكلوي). بالإضافة إلى داء السكري طويل الأمد ، وأمراض الكلى المزمنة ، والكلى الكيسية وكذلك الأدوية ، وأمراض جهاز المناعة (التهاب كبيبات الكلى) ، وارتفاع ضغط الدم ، أو في حالات نادرة ، تلف أنسجة الكلى بسبب أسباب أخرى.
الأعراض لمرضى غسيل الكلى
مع الفشل الكلوي المزمن ، هناك زيادة في كمية البول في البداية ثم انخفاضها. يتشكل احتباس الماء (الوذمة) في الجسم ، على سبيل المثال في الساقين والرئتين. على المدى الطويل ، تسبب مشاكل الهرمونات ارتفاع ضغط الدم ونقص خلايا الدم الحمراء (فقر الدم) وهشاشة العظام. نظرًا لأنه لم يعد من الممكن التخلص من السموم بشكل كافٍ ، فقد يحدث المزيد من تلف الأعضاء. غالبًا ما يكون تلون الجلد الأصفر ملحوظًا. في المرحلة المتقدمة (المرحلة الرابعة ، الفشل الكلوي النهائي ، الانسمام اليوريمائي ) هناك غثيان وقيء ورائحة الفم الكريهة واضطرابات في الدماغ والأعصاب والأعضاء الأخرى.
تشخيص الحاجة لـ غسيل الكلى الدموي
أولاً ، يتم استجواب المريض وفحصه جسديًا في مركز غسيل الكلى . سيتم فحص الدم والبول وفحص الكلى بالموجات فوق الصوتية.
التشخيص التفريقي
عادةً ما يتم تشخيص مرض المرحلة النهائية من الفشل الكلوي والذي يتطلب غسيل الكلى بوضوح من خلال التاريخ الطبي والفحوصات.
العلاج
ضمن وحدة غسيل الكلى في الـ مستشفيات ،يتم توصيل ماكينة غسيل الكلى إلى مجرى الدم حيث يتم نقل الدم من المريض إلى أجهزة غسيل الكلى ، حيث يصل إلى غشاء شبه منفذ. يقوم هذا بتصفية السموم وفضلات التمثيل الغذائي والسوائل الزائدة من الدم ، والتي تتدفق مرة أخرى إلى جسم المريض في حالة نقاء.
وشملت جلسات غسيل الكلى أشكال أخرى ، مثل غسيل الكلى البريتوني , باستخدام البريتوان الغشائي (الطبقة المبطنة لتجويف البطن ، الصفاق) كغشاء.
يجب أن يكون هناك وصول إلى وعاء دموي لتوصيل جهاز غسيل الكلى . عند الحاجة إلى غسل الكلى ، يتم ادخال قسطرة إلى وريد كبير ، على سبيل المثال في العنق أو وريد الترقوة.
الجراحة
انشاء تحويلة لغسيل الكلى لأول مرة
الأوردة السطحية التي يتم ثقبها من أجل غسيل الكلى ، يتم انسدادها بجلطات الدم (الخثرات) بعد فترة قصيرة ، ويصبح تدفق الدم غير كافٍ. لذلك ، يتم إنشاء اتصال من هذا الوريد إلى الشريان القريب ، وهذا يشار إليه بعد ذلك باسم التحويلة الشريانية الوريدية أو الناسور الشرياني الوريدي.
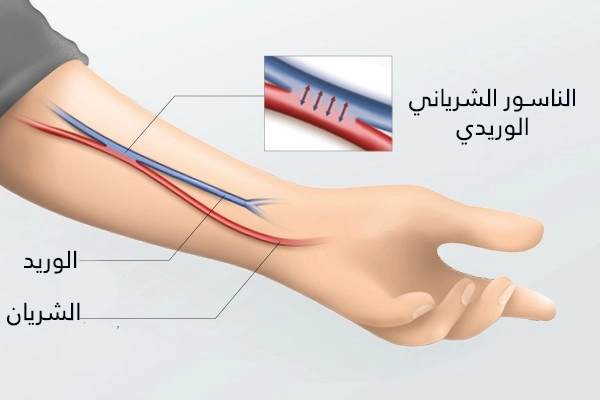
يمكن إجراء العملية تحت تأثير التخدير الموضعي أو الناحي (تخدير منطقة أكبر من الجسم). التخدير العام ممكن أيضًا ، لكن لا يحتاج مرضى الكلى لإجرائه بشكل متكرر لمثل هذه الإجراءات.
عادة ما يتم عمل تحويلة جديدة لغسيل الكلى على الساعد ؛ كما يمكن أيضًا إجراء العملية على أوردة في الجزء العلوي من الذراع أو في الكوع أو على الساق. إذا تم أخذ الساعد ، يتم خياطة نهاية الوريد الذي يمتد من الإبهام إلى الذراع في الشريان المجاور (تحويلة سيمينو). من المفضل استخدام الذراع اليسرى للأشخاص الذين يستخدمون اليد اليمنى والذراع اليمنى للأشخاص الذين يستخدمون اليد اليسرى للوصول إلى تحويلة طبية لغسيل الكلى.
إذا كان هناك شريان في المنطقة المرغوبة ، ولكن لا يوجد وريد مناسب ، فيمكن أيضًا إزالته من جسم المريض نفسه ، وعادةً الساق ، وزرعه ، أو يمكن إدخال طرف اصطناعي وعائي بلاستيكي (طعم). من أجل ضمان وجود مسار أكبر للأوعية الدموية للثقوب المتكررة اللاحقة ، يمكن وضع التحويلة في مسار متعرج.
يمكن فحص حالة الأوعية الدموية الجديدة وتقييمها عن طريق فحص الأشعة السينية مع حقن عامل تباين .
التدخلات الجراحية على تحويلة غسيل الكلى الموجودة مسبقاً
يمكن للجلطة الدموية (الجلطة) التي تكونت داخل التحويلة أن تسدها ويجب إزالتها عن طريق الجراحة. لهذا الغرض ، يتم فتح التحويلة ، ويتم إدخال قسطرة بآلية بالون يمكن ملؤها وتضخيمها خلف الجلطة. يمكن بعد ذلك سحب الخثرة والقسطرة إلى المنطقة المفتوحة وإزالتها بسهولة هناك. هنا ، أيضًا ، يمكن إجراء فحص عامل تباين الأشعة السينية للتقييم. بعد إزالة الجلطة بنجاح ، يتم خياطة التحويلة ، غالبًا بإدخال شريط (طعم ) مصنوع من البلاستيك أو وريد مأخوذ من جزء آخر من الجسم ، عادةً من الساق.
إذا لم يكن هناك ما يكفي من الدم لغسيل الكلى في التحويلة ، فيمكن نقل وصلة التحويلة إلى منطقة أخرى ، على سبيل المثال في الجزء العلوي من الذراع أو في انحناء الكوع. إذا لم يعد وعاء التحويل في حالة جيدة أو تشكل انتفاخ (تمدد الأوعية الدموية) ، فيمكن استبداله بوريد من جسمك أو بنسخة بلاستيكية متماثلة للأوعية الدموية (طعم).
إذا دخل الكثير من الدم في التحويلة ، يجب جعل الاتصال أكثر إحكامًا من جهة لحماية القلب ، والذي يتعين عليه القيام بعمل إضافي ، و من جهة أخرى لضمان وصول الدم إلى الذراع أو الساق.
إزالة تحويلة غسيل الكلى
عندما يتم ضمان وظائف الكلى مرة أخرى عند المصابين ، على سبيل المثال بعد زرع كلية ، أو عند تطبيق تحويلة أخرى تعمل ، يمكن ربط الوصلة الوعائية بخياطة. غالبًا ما يظل الوريد مفتوحًا بسبب التدفقات الأخرى ويمكن تحويله مرة أخرى لاحقًا إذا لزم الأمر.
الإجراءات الإضافية المحتملة للعملية
إذا تبين أثناء العملية أن هناك نتائج غير متوقعة وأكثر شمولاً أو تغييرات مرضية أو مضاعفات أخرى ، فقد يكون من الضروري اتخاذ تدابير أخرى أو مختلفة. ويشمل ذلك أيضًا توسيع تضيقات الأوعية الدموية عن طريق التوسيع بالبالون ، أو إذابة جلطات الدم باستخدام بعض المكونات النشطة (تحلل) أو إدخال دعامة وعائية داخلية (STENT).
مضاعفات عملية تحويلة غسيل الكلى
عادة ما يزول الانزعاج الطفيف والألم في وقت قصير. يمكن أن تحدث إصابات في الهياكل المجاورة. في حالة تلف الأوعية الدموية أو فتح الخيط ، يمكن أن يحدث نزيف ونزيف ثانوي وأورام دموية (كدمات). من ناحية أخرى ، يمكن أن تتراكم الجلطات الدموية في التحويلة ، ويمكن أن تنفصل وتسد الأوعية الدموية الأخرى. أيضاً قد يحدث انتفاخ التحويلة (تمدد الأوعية الدموية). قد يؤدي تلف الأعصاب إلى الشعور بالخدر والشلل. هناك خطر أن تتطور العدوى والالتهابات واضطرابات التئام الجروح والتندب. يمكن أن تؤدي العدوى في منطقة التحويلة إلى تجرثم الدم الذي يهدد الحياة (تنتشر العدوى عبر مجرى الدم). من المضاعفات أيضاً الحساسية.
الانذار بعد تحويلة غسيل الكلى
تصبح التحويلة (ناسور شرياني وريدي )التي تم إنشاؤها حديثًا أكثر سمكًا بمرور الوقت ويصبح جدار الوعاء الدموي أقوى بشكل عام . بعد عدة أسابيع ، يمكن إجراء أول ثقب لغسيل الكلى عبر هذه التحويلة. غالبًا ما تستمر التحويلة لعدة سنوات ، وأحيانًا 10 سنوات أو أكثر. ومع ذلك ، قد تتوقف عن العمل في مرحلة مبكرة.
على الرغم من التطورات الطبية ، فإن متوسط العمر المتوقع للمرضى الذين يخضعون لغسيل الكلى أقل من مرضى الكلى السليمة: معدل البقيا بعد عشر سنوات عند مرضى الغسيل الكلوي هو أكثر من 50 %. يعتمد الانذار على الأمراض المصاحبة وعمر المريض. يمكن اللجوء إلى زرع الكلى.
اذاً يحتاج الأشخاص المصابون بـ أمراض الكلى في مراحله النهائية (الفشل الكلوي) إلى إزالة الفضلات من مجرى الدم عبر وصل ماكينة غسيل الكلى إلى مجرى دم المريض (قسم غسيل الكلى بمستشفى) أو لـ عملية زراعة الكلى كـ علاج لأمراض الكلى للبقاء على قيد الحياة.
قبل عملية تحويلة غسيل الكلى
إذا لزم الأمر ، يجب التوقف عن تناول الأدوية التي تثبط تخثر الدم ، مثل Marcumar® أو Aspirin® ، بالتشاور مع الطبيب. الأدوية التي تحتوي على المادة الفعالة ميتفورمين المستخدمة في داء السكري (مرض السكري) قد يتم حذفها أيضًا قبل فحص عامل التباين.
بعد عملية تحويلة غسيل الكلى
إذا تم إجراء العملية في العيادة الخارجية ، فيجب وجود مرافق لاصطحاب المريض ،حيث لا يسمح للمريض بقيادة السيارة لمدة 24 ساعة .
يجب أن يتم تحويل وضع الذراع أو الساق في البداية عالياً وعدم الضغط عليها. لا تكاد توجد أي قيود في وقت لاحق ، يجب تجنب الإصابات فقط ، لأنها يمكن أن تؤدي إلى نزيف أكثر غزارة.
يجب مراعاة نظافة الجلد الكافية في منطقة تحويلة غسيل الكلى. يجب أيضًا فحص التحويلة المركز مرارًا وتكرارًا من قبل المرضى ، على سبيل المثال ، يمكن الشعور بتدفق الدم. في حالة وجود أي شذوذ يجب الاتصال بالطبيب أو الذهاب الى مستشفى.

