عملية استئصال الغدة اللعابية هي جراحة تهدف لإزالة كامل الغدة اللعابية أو جزء منها، وهي عملية شائعة في تركيا يمكن إجراؤها بأحدث التقنيات ودون ترك ندبة.
قد يحتاج الشخص إلى عملية استئصال الغدة اللعابية إذا تشكل ورم سرطاني في الغدة فيتم إزالتها لمنع انتقال الورم وتأذي الأنسجة أو البنى القريبة المهمة مثل العصب الوجهي.
عادة تكون جراحة استئصال الغدة اللعابية هي العلاج الأساسي الموصى به عند المصابين بحالات أورام الغدد اللعابية الخبيثة وقد يوصي الجراح إضافة لذلك بالعلاج الإشعاعي أو الكيميائي أو مزيج من الاثنين وفقاً لخصائص الورم ومرحلة الورم.
قد تكون الجراحة الترميمية والعناية بالأسنان وإعادة التأهيل أيضاً جزءاً من خطة التعافي الخاصة بك.
ستتعرف في هذا المقال على جراحة استئصال الغدة اللعابية المتاحة في اسطنبول وأنواعها ومتى تحتاجها.
ما هي عملية استئصال الغدة اللعابية؟
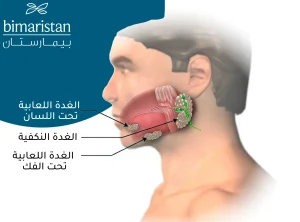
تهدف جراحة استئصال الغدد اللعابيّة إلى إزالة إحدى الغدد اللعابية وهي الغدد المسؤولة عن إفراز اللعاب في الفم، يوجد لدى الشخص غدد صغيرة ثانوية إضافة لثلاثة أزواج رئيسية من الغدد هي:
- الغدتان تحت الفك السفلي
- الغدتان تحت اللسان
- الغدتان النكفيتان
يتوقف نوع التخدير المطلوب لهذه الجراحة على الغدة المراد استئصالها، فإذا كانت من الغدد اللعابية الصغيرة الثانوية فسيتم الاكتفاء بالتخدير الموضعي بينما جراحة الغدد اللعابية الرئيسية الكبيرة مثل الغدة النكفية تتطلب تخديراً عاماً.
متى تحتاج جراحة استئصال الغدة اللعابية؟
يتم إجراء عملية استئصال الغدة اللعابية عادة لإزالة الأورام التي تنمو في هذه الغدد أو بسبب انسداد قنواتها، تشير الدراسات الإحصائية إلى أن أكثر من نسبة 70٪ تقريبا من أورام الغدد اللعابية حميدة (غير سرطانية) ورغم هذا يجب فحص أي كتلة يتم الكشف عنها وعادة ما يتطلب كلا نوعي الورم إلى الإزالة.
الأورام الحميدة
قد يحتاج الشخص إجراء عملية استئصال الغدة اللعابية من أجل إزالة الأورام الحميدة لأنها تنمو أحياناً بشكل كبير وتضغط على النسج المجاورة وتؤذيها، كما يمكن أن تتحول أنواع معينة من الأورام الحميدة إلى سرطان الغدد اللعابية.
الأورام الخبيثة
تسبب الأورام الخبيثة (السرطانية) تلف النسج المحيطة وتتميز بقدرتها على الانتشار لمناطق أخرى في الجسم، حيث تنفصل الخلايا السرطانية عن الورم الأصلي وتنتشر إلى أماكن أبعد في الجسم من خلال مجرى الدم أو الجهاز اللمفاوي.
قد ينتشر سرطان الغدد اللعابية إلى الغدد الليمفاوية القريبة الموجودة في العنق لينتقل بعدها إلى أجزاء أخرى من الجسم.
العلاجات الإضافية للسرطان قد تشمل العلاج الإشعاعي وجراحات إضافية بما في ذلك إزالة العقدة الليمفاوية والإجراءات الترميمية.
الالتهاب والعدوى
يمكن أن يصيب الغدد اللعابية أمراضاً عديدة نذكر أهمها:
حصوات الغدد اللعابية
انسداد والتهاب بالغدد اللعابية بسبب وجود حصى متكلسة، تتشكل حصوات الغدد اللعابية نتيجة تراكم رواسب الكالسيوم في الغدد مما يمنع تدفق اللعاب في الفم، يمكن أن يسبب هذا تورماً متكرراً في الغدد وعدوى.
هناك عدة طرق لإزالة الحصوات اللعابية مثل تنظير الغدد اللعابية، ولكن في بعض الحالات تتوضع التكلسات داخل الغدّة مما يلزم استئصالها.
إلتهاب الغدد اللعابية
قد تحتاج أيضاً إلى استئصال الغدة عند الإصابة بعدوى الغدد اللعابية والتي يمكن أن تحدث نتيجة لوجود حصى ضمنها أو ناجمة عن فيروس أو بكتيريا.
قبل التوصية بالجراحة قد يطلب جراح الرأس والرقبة فحصوات تصوير مثل الفحص بالأشعة المقطعية لرؤية الغدة تحت الفك السفلي ومعرفة المزيد حول ما يعيق تدفق اللعاب.
فرط إفراز اللعاب
قد يفكر طبيبك بإزالة الغدة اللعابية للسيطرة على حالة فرط سيلان اللعاب (زيادة إفراز اللعاب).
يمكن أن تحدث هذه الحالة عند الأشخاص الذين يعانون من مشاكل عصبية تعيق التحكم في عضلات الفم والوجه مثل مرض باركنسون أو السكتة الدماغية.
تساعد بعض الأدوية في السيطرة على الحالة ولكن إذا لم يكن الدواء فعالاً قد يناقش الطبيب إزالة الغدّة اللعابية جراحياً للتحكم في إفراز اللعاب المفرط خاصة في حال هناك صعوبة بالبلع وخطر استنشاق اللعاب والاختناق موجود.
بالنسبة لبعض المرضى قد لا نضطر لإزالة الغدة ونقوم فقط بربط إحدى القنوات اللعابية جراحياً للتحكم في اللعاب الزائد.
التحضير لعملية استئصال الغدة اللعابية
قبل التداخل الجراحي على الحالة سيقوم الأخصائي أولاً بإجراء فحص جسدي والتأكيد على الأدوية التي يجب وصفها قبل العملية وشرح الأدوية التي لا يمكن تناولها.
الفحص الطبي
سيقوم الجراح بإجراء فحص بدني شامل قبل الجراحة ومراجعة حالتك الطبية السابقة والحالية، سيتم فحص الوجه والعنق والفكين وداخل الحفرة الفموية ليتحرى تشكل حصى أو كتل أو آفات.
يشمل ذلك أيضاً فحص تناسق الوجه ووظيفة الأعصاب التي تحرك زوايا الفم والسؤال عن الأدوية التي تتناولها بما ذلك الأدوية العشبية والمكملات الغذائية.
التصوير الشعاعي
قد يتطلب الفحص إجراء اختبارات باستخدام التصوير المقطعي المحوسب CT للرأس والرقبة أو التصوير بالرنين المغناطيسي MRI للتخطيط للعملية الجراحية وتحديد مكان الورم، إذا كان الورم قريباً من عصب الوجه تساعد الصور التشخيصية هذه الجراح في التخطيط لأفضل طريقة يمكن إزالته بها دون إحداث أذية بالعصب الوجهي.
الخزعة
إذا اشتبه الأخصائي بوجود ورم قد يطلب إجراء خزعة تشخيصية باستعمال إبرة دقيقة رفيعة FNA لإزالة عينة صغيرة من الخلايا والمساعدة في تشخيص نوع الورم.
سيتطلب وجود الورم الخبيث السرطاني بالغدة اللعابية خطة علاج مختلفة.
تنظير الغدد اللعابية
إجراء يستخدم لفحص قنوات الغدد اللعابية من خلال إدخال تلسكوب مصغر يسمى بالمنظار في فتحة قناة الغدد اللعابية لاستكشافها، ويمكن إدخال أدوات صغيرة من خلال المنظار الدقيق لإزالة أي حصى موجودة.
تحديد موعد عملية استئصال الغدة اللعابية
بمجرد تشخيص الحالة وأخذ موافقة الشخص سيتم تحديد موعد الجراحة.
ستتلقى تعليمات حول التحضير لاستئصال الغدّة اللعابية بما في ذلك الأدوية التي يجب أن تتناولها أو تتوقف عن تناولها ومتى يجب عليك التوقف عن الأكل أو الشرب قبل الجراحة وما إلى ذلك.
قد تتلقى أيضاً إرشادات حول التوقف عن التدخين، يزيد التدخين من خطر إصابتك بمشكلات في التنفس أثناء الجراحة ويمكن أن يبطئ من سير عملية التعافي بعد ذلك.
عملية استئصال الغدة اللعابية: ماذا يحدث في الجراحة؟
تستغرق الجراحة نفسها حوالي ساعة ونصف لكن العملية برمتها بما في ذلك الاستعدادات السابقة للعملية والتعافي بعد العملية تستغرق حوالي ست ساعات، سيتم إعطاؤك تخديراً موضعياً أو عاماً للتأكد من أنك مرتاح طوال الجراحة.
يقوم الجراح بعمل شق (قطع) في تجعد الجلد بالرقبة أسفل الفك، حيث الندبة أقل وضوحاً، قد يصل طول الشق إلى 2 سم إلى 3 سم.
بعد ذلك يحدد الجراح والفريق موقع الغدة اللعابية وتحريرها بعناية من النسج والبنى المحيطة بها ثم تُستأصل الغدة بالكامل ويُغلق الجرح.
بمجرد استيقاظك من التخدير وفحصك من قبل الجراح قد تقضي الليلة في المستشفى قبل خروجك، سيتم إعطاؤك مسكناً للألم أثناء تعافيك في المنزل.
عملية استئصال الغدة اللعابية النكافية
استئصال الغدة النكفية هو اسم الجراحة المستخدمة لإزالة الورم الحميد أو السرطاني في الغدد النكفية، تتطلب هذه العملية رعاية وخبرة من جانب فريقك الجراحي للتأكد من عمد إحداث أذية بالعصب الوجهي والبنى الأخرى القريبة من هذه الغدة.
ستخضع للعملية في مستشفى أو مركز جراحة، تحتاج إلى البقاء عادة ليلة إلى ليلتين عند استئصال الغدة النكافيّة.
أثناء الإجراء:
- سيتم تخديرك عبر الوريد حتى تبقى نائماً أثناء الجراحة.
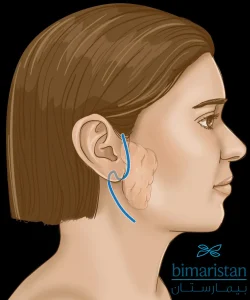
- سيقوم الجراح بعمل شق يبدأ أمام أذنك ويمتد للخلف وللأسفل حتى التجعد الطبيعي في الجزء العلوي من رقبتك، سيساعد نمط القطع في إخفاء الجرح بمجرد أن يشفى.
- يتم كشف الغدة النكفية والتعرف على العصب الوجهي لتوخي الحذر وتجنب إتلافه أثناء الجراحة، قد يتم استخدام جهاز مراقبة العصب الوجهي لضمان عمل العصب الوجهي بشكله الصحيح خلال الجراحة.
- تتم إزالة الغدة بالكامل أو جزء منها، إضافة لإزالة العقد الليمفاوية القريبة في رقبتك في حال انتشرت الخلايا السرطانية هناك.
- وأخيراً خياطة الشق.
قد يدخل الجراح أنبوب صغير يسمى أنبوب التصريف لالتقاط أي دم أو سوائل قد تتجمع في موقع الجراحة.
عملية استئصال الغدة اللعابية تحت الفك السفلي
لعلاج ورم حميد أو سرطاني في الغدد تحت الفك السفلي يزيل الجراح الغدة المصابة.
تقع الغدد تحت الفك السفلي مباشرة أسفل الفك، سيقوم الجراح بعمل شق تحت خط الفك لإزالة الغدة وبعض النسج المحيطة، يعتمد مدى الجراحة على حجم ونوع الورم الذي يتم علاجه.
تتطلب عملية استئصال الغدة اللعابية تحت الفك السفلي دقة ومهارة لوجود أعصاب مهمة قريبة منها:
- العصب الفك السفلي الذي يساعدك على الابتسام
- العصب اللساني الذي يسمح بالإحساس في اللسان
- العصب تحت اللسان والذي يسمح بحركة جزء اللسان الذي يساعد في البلع والكلام
سيحاول جراحك أثناء الجراحة الحفاظ على هذه البنى وغيرها كلما أمكن ذلك اعتماداً على مدى امتداد الورم وموقعه.
عملية استئصال الغدة اللعابية تحت اللسان
يتضمن استئصال الغدة تحت اللسان إزالة الغدة بأكملها، تقع هذه الغدد تحت لسانك على جانبي أرضية فمك.
سيقوم الجراح بعمل قطع داخل فمك لإزالة الغدة مع بعض الأنسجة المحيطة، غالباً ما يتم إصلاح المنطقة الجراحية إما عن طريق إغلاق الفجوة بالغرز أو باستخدام تقنية تطعيم الجلد.
تتطلب عملية استئصال الغدة اللعابية تحت اللسان الدقة من الدكتور الجراح لتجنب أذية العصب اللساني الواقع في هذه المنطقة.
العصب اللساني مسؤول عن الإحساس والتذوق على جانب اللّسان، قد يحدث إحساس بالخدر في الجانب المصاب من اللّسان عادة ما يكون تخديراً مؤقتاً يزول بعد بضعة أسابيع إلى شهرين.
جراحة سرطان الغدد اللعابية الصغرى
يمكن أن يحدث سرطان في أحد الغدد اللعابية الثانوية الصغيرة المنتشرة في الشفاه واللسان وسقف الحنك وباطن الخد والحلق والحنجرة والأنف والجيوب الأنفية.
تعتمد الجراحة على حجم وموقع الورم، عادةً ما يزيل الجراح بعض النسج المحيطة.
استئصال العقدة الليمفاوية
كثيراً ما تنتشر سرطانات الغدد اللعابية إلى الغدد الليمفاوية في الرّقبة أولاً قبل أن تنتشر في أي مكان آخر.
لهذا غالباً ما يتم إزالة العقد الليمفاوية الرقبية التي يظهر أنها تحتوي أو من المحتمل أن تحتوي على السرطان مع بعض النسج الأخرى المجاورة للغدة أثناء إزالة السرطان.
مضاعفات عملية اﺳﺘﺌﺼﺎل الغدة اللعابية ومخاطرها
لا تعد عملية اﺳﺘﺌﺼﺎل الغدة اللعابية جراحة ذات خطورة عالية ومع ذلك هناك احتياطات يجب مراعاتها أثناء الاستئصال نظرًا إلى تصاحبها وقربها من أماكن تشريحية مهمة، أهم هذه الاحتياطات:
حماية الأعصاب
توجد العديد من الأعصاب المهمة بالقرب من الغدد اللعابية التي يحرص الجراح على تجنب رضها أو إتلافها أثناء هذه العملية.
تشمل الأعصاب التي يجب حمايتها أثناء عملية استئصال الغدة اللعابية ما يلي:
- العصب الوجهي
- العصب اللساني الذي يتحكم بالإحساس باللسان
- العصب تحت اللّسان والذي يسمح بحركة اللّسان
يمكن أن تؤدي أذية هذه الأعصاب أثناء عملية استئصال اﻟﻐﺪة اللعابية إلى تغييرات مؤقتة في حركة عضلات الوجه أو ضعف الإحساس في المناطق التي يسيطرون عليها خاصة إذا كانت هناك حاجة إلى تشريح جراحي واسع النطاق حول العصب الوجهي.
يعد الضرر الدائم لهذه الأعصاب من المضاعفات نادرة الحدوث وعادة ما ينتج فقط عن حالات استئصال الغدة النكفية شديدة التعقيد بينما خدر الأذن يكون شائعاً إلى حد ما.
متلازمة فراي Frey’s syndrome
قد تبدأ الحالة لدى بعض الأشخاص بعد عدة أشهر من الجراحة، يحدث لدى الأشخاص المصابين بهذه المتلازمة تعرق شديد على جانب الوجه عند الأكل.
تُعد مضادات التعرق وحقن البوتكس Botox علاجات مقترحة لمتلازمة فراي.
متلازمة العضة الأولى
تتضمن متلازمة العضة الأولى ألماً شديداً عند تناول أول قضمة من الطعام بعد الجراحة، يقل الألم مع كل مضغة تالية.
يمكن أن تؤدي حقن البوتوكس إلى إرخاء العصب المسبب للألم.
مضاعفات إضافية
من الممكن حدوث مضاعفات بالإضافة إلى الموصوف أعلاه بعد عملية استئصال الغدة اللعابية تشمل:
- النزيف
- العدوى
- الندوب
- تراكم السوائل تحت الجلد الذي يمكن أن يشكل كيساً أو كتلة
تشمل المخاطر الأخرى التي تنطبق على معظم العمليات الجراحية بما في ذلك عملية استئصال الغدة اللعابية ما يلي:
- رد فعل تحسسي لأدوية الألم
- تأذي عضو قريب أثناء الجراحة
- تجمع السوائل في موقع الجراحة (التورم المصلي أو الغشاء اللعابي)
- تجمع الدم في موقع الجراحة (ورم دموي)
- عدوى أو نزيف أو تندب
عادة ما يكون بقاء الندوب بعد استئصال الغدد اللعابيّة وخاصة النكفية ضئيلاً بسبب إجراء جروح تتناسب مع تجاعيد الرقبة بحيث يصعب رؤيتها عند التئام الجرح.
التعافي بعد إزالة واستئصال الغدة اللعابية
بعد عملية استئصال الغدة اللعابية سيراقب الأخصائي حركات وجه المريض ويطلب منه الابتسام أو القيام بإيماءات على الوجه.
بمجرد الوصول إلى المنزل من المهم اتباع تعليمات الجرّاح حول العناية بالجروح والروتين الصحي.
قد يعود المريض إلى العيادة لإزالة الغرز بعد أيام قليلة من الجراحة، وقد تلاحظ بعض الكدمات الطفيفة عندها، بمجرد الإزالة يجب غسل المنطقة بالماء والصابون المعتدل.
سيُطلب منه اتباع تعليمات العناية بالجروح والتي تشمل الحفاظ على مكان الجرح نظيفاً وجافاً وعدم إجهاد أو رفع أي أشياء ثقيلة.
قد تضطر إلى التعود على الشعور بإحساس أقل في وجهك عادة ما يكون هذا التغيير مؤقتاً.
ناقش طبيبك حول كيفية تأثير الجراحة على الأنشطة اليومية أثناء فترة التعافي والتغييرات التي يجب أن تتوقعها وكيف يمكنك التخطيط لها قبل الخضوع لعملية استئصال الغدة اللعابية.
متى يجب أن أراجع الطبيب؟
لا تتأخر عن التواصل مع طبيبك في حال لاحظت أياً ما يلي:
- ألم لا يمكن السيطرة عليه بالأدوية
- يشعر وجهك بالخدر أو الضعف بشكل متزايد
- لاحظت تسرب صديد أو سائل أو دم من الجرح
- تشعر بأن جرحك منتفخ ومؤلم
- رائحة كريهة مكان الجرح
عملية استئصال الغدة اللعابية هي جراحة شائعة لإزالة الغدة اللعابية بكاملها أو جزء منها بسبب إصابتها بأحد أمراض الغدد المختلفة، يجب على معظم الناس إجراء تعديلات على روتينهم اليومي بعد الجراحة مثل اختيار الأطعمة التي يسهل مضغها وابتلاعها والابتعاد عن الإجهاد.
المصادر