اضطرابات المفصل الفكي الصدغي هي نوع من الاضطرابات الشائعة لدى البالغين ويمكن أن تُسبب اضطرابات المفصل الفكي الصدغي ألم في الوجه أو الصرير وقد تؤثر على جانب واحد من الوجه أو الجانبين معاً.
ما هو المفصل الصدغي الفكي؟
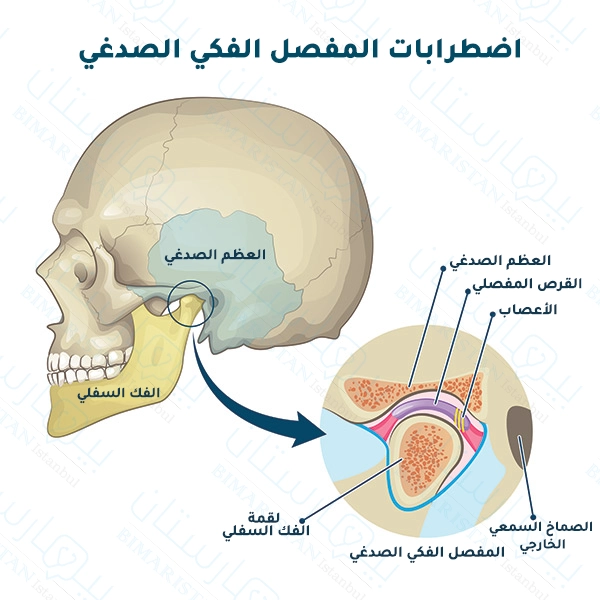
يعد المفصل الصدغي الفكي أحد أكثر المفاصل تعقيداً في الجسم وهو المفصل الذي يربط الفك بالعظام الصدغية بالجمجمة، ويقع أمام كل أذن، يعمل المفصل الفكي على تحريك الفك لأعلى ولأسفل ومن جانب إلى آخر ومن الخلف إلى الأمام مما يمكن المرء من التحدث والمضغ والتثاؤب.
يمكن الشعور به وهو يتحرك بالضغط بإصبع السبابة على الخدين وفتح الفم وإغلاقه، يوجد بالمفصل العظام والعضلات بالإضافة إلى قطعة صغيرة من غضروف (نسيج صلب) تعمل كممتص للصدمات وتحمي العظام من التآكل والتمزق.
تُعرف المشاكل التي تتعلق بالفك والعضلات التي تتحكم فيه باسم اضطرابات المفصل الفكي الصدغي temporomandibular disorders (TMD).
أسباب اضطرابات المفصل الفكي الصدغي
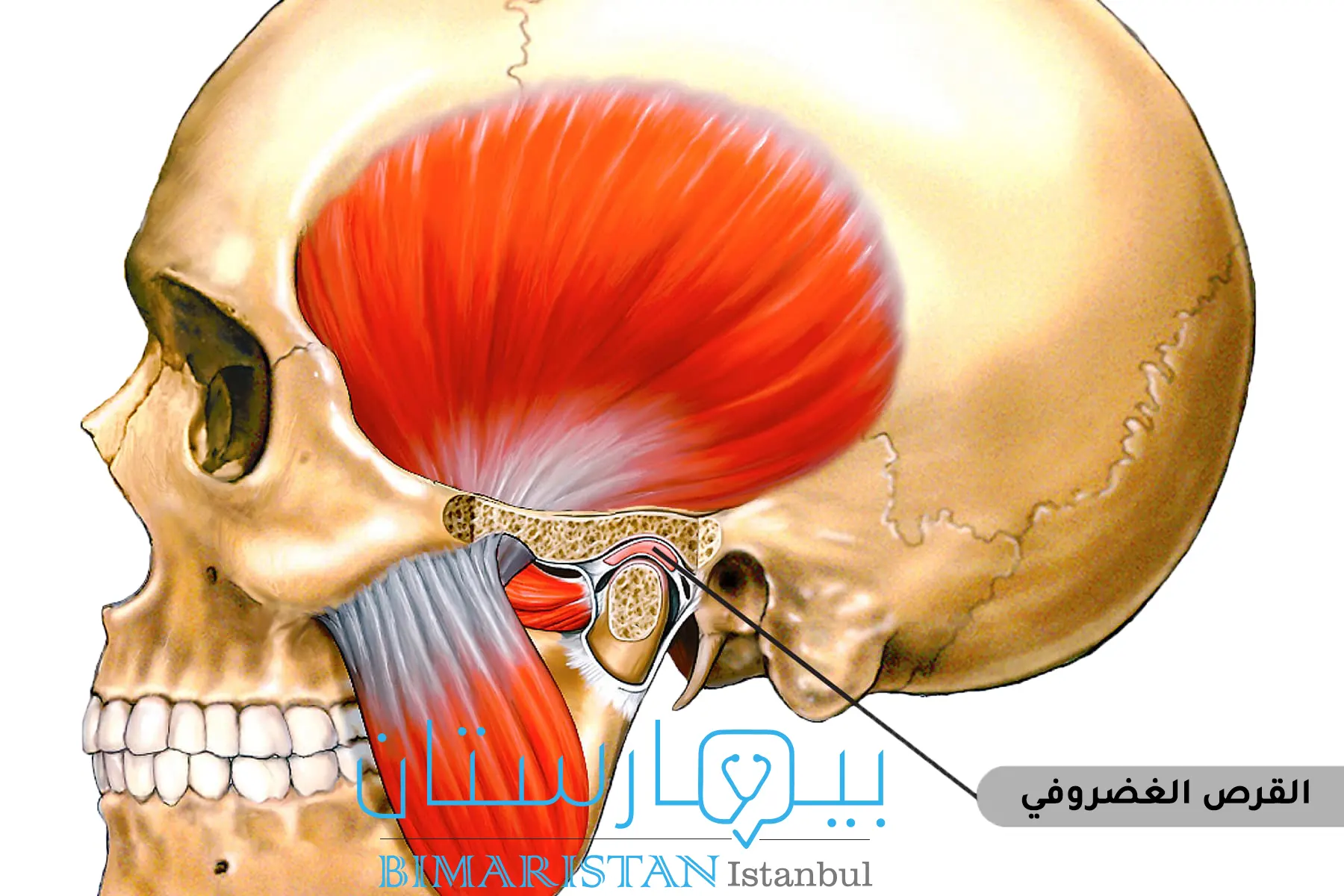
ليس من الواضح دائماً سبب حدوث اضطرابات المفصل الفكّي الصدغي، إن السبب الأكثر شيوعاً هو انزلاق قطعة من الغضروف في المفصل عن مكانها، يعتقد أطباء الأسنان أيضاً أن الأعراض قد تنشأ عن مشاكل في عضلات الفك أو في أجزاء المفصل الأخرى.
- يمكن أن تؤدي إصابة الفك أو خلعه أو إصابة المفصل نفسه أو إصابة بعض عضلات الوجه والعنق إلى اضطراب المفصل الصدغي الفكي.

أعراض اضطرابات المفصل الفكي الصدغي:
غالباً ما تسبب الاضطرابات في المفصل الفكّي الصدغي ألماً شديداً وإحساساً بعدم الراحة، يمكن أن تكون الأعراض مؤقتة أو أن تستمر لسنوات عديدة، وتؤثر على الرجال بشكل أكبر من النساء، وتنتشر عند الأشخاص الذين تتراوح أعمارهم بين 20 و40 سنة، وتشمل الأعراض الشائعة ما يلي:
- الإحساس بالألم في الوجه ومنطقة مفصل الفك والرقبة وقد يمتد للكتفين وداخل الأذن أو حولها وذلك عند المضغ أو التحدث أو عند فتح الفم بشكل واسع كما هو الحال عند التثاؤب.
- يعلق الفك بوضعية الفم المفتوح أو الإغلاق.
- فرقعة أو صرير في المفصل الفكي الصدغي عند فتح أو إغلاق الفم وعند المضغ، قد يكون هذا مؤلماً وقد لا يكون كذلك.
- الشعور بالتعب في الوجه.
- عناء في المضغ أو عضة غير مريحة مفاجئة، كما لو أن الأسنان العلوية والسفلية لا تتلاءم معاً بشكل صحيح.
- تورم في جانب الوجه.
- آلام في الأسنان، وصداع، وآلام في الرقبة، ودوخة، وآلام في الأذن، ومشاكل في السمع، وألم أعلى في الكتف، وطنين في الأذنين.
كيف يتم تشخيص اضطرابات المفصل الفكي الصدغي؟
تتسبب العديد من الحالات الأخرى ظهور أعراض مشابهة لهذا الاضطراب مثل تسوس الأسنان أو مشاكل الجيوب الأنفية أو التهاب المفاصل أو أمراض اللثة، ولمعرفة الحالة بشكل دقيق، يسأل طبيب الأسنان عدة أسئلة متعلقة بالحالة ويجري بعض الفحوص البدنية.
- يفحص الطبيب المفصل الفكي الصدغي بشكل دقيق ويبحث عن مكان الألم، ويستمع للأصوات التي تصدر عن المفصل كصوت النقرة أو الطقطقة أو صوت الصرير المزعج عند التحريك.
- سيتأكد الطبيب أيضاً من أن الفك يعمل كما ينبغي وأنه لا يعلق عند فتح الفم أو عند إغلاقه، بالإضافة إلى أنه قد يختبر العضة ويتحقق من وجود مشاكل في عضلات الوجه.
- قد يأخذ طبيب الأسنان صوراً بالأشعة السينية للوجه الكامل حتى يتمكن من رؤية الفكين ومفصلي الفك والأسنان لاستبعاد المشكلات الأخرى، وقد يعمد الطبيب إلى إجراء اختبارات أخرى، مثل التصوير بالرنين المغناطيسي MRI أو التصوير المقطعي المحوسب CT، حيث يمكن للتصوير بالرنين المغناطيسي أن يُظهر ما إذا كان قرص المفصل الفكي الصدغي في الموضع المناسب أثناء تحرك الفك، بينما يُظهر التصوير المقطعي المحوسب التفاصيل العظمية الكاملة للمفصل.
- قد تتم إحالة المريض إلى جراح الفم والوجه والفكين للحصول على المزيد من الرعاية والعلاج، يكون هذا الطبيب متخصص في الجراحة في وحول منطقة الوجه والفم والفك بالكامل، وقد يحال المريض إلى أخصائي تقويم أسنان للتأكد من توضع الأسنان والتأكد من عدم وجود ضغط زائد من الأسنان والعضلات على المفصل الفكي الصدغي.
العلاجات المنزلية لاضطرابات المفصل الفكي الصدغي
هناك عدة طرق منزلية يمكن للمريض أن يفعلها بنفسه للمساعدة في علاج اضطرابات المفصل الفكي الصدغي:
- تناول الأدوية التي لا تحتاج استشارة أو وصفة طبية، حيث يمكن للمريض أن يأخذ مضادات الالتهاب غير الستيروئيدية NSAIDs مثل الايبوبروفين للتخفيف من آلام العضلات ومن التورم.
- استخدام الكمادات الباردة، إذ يساعد وضع أكياس الثلج على منطقة المفصل الفكي الصدغي على تخفيف التورم.
- القيام ببعض تمارين التمدد stretches للفك، وعند الانتهاء من ذلك يُنصح بوضع منشفة دافئة على المنطقة نفسها لمدة 5 دقائق، يجب تكرار هذا الروتين عدة مرات في اليوم
- تناول الأطعمة اللينة سهلة المضغ مثل اللبن والبطاطا المهروسة والجبن والحساء والفواكه والخضروات المطبوخة والفاصوليا والحبوب، وتقطيع الأطعمة إلى قطع صغيرة حتى لتجنب حركات المضغ الزائدة، ويجب تجنب الأطعمة القاسية والمقرمشة (مثل البسكويت المملح والجزر النيء) والوجبات السميكة أو الكبيرة التي تتطلب فتح الفم على مصراعيه.
- تجنب حركات الفك الشديدة، كمحاولة تخفيض حركات التثاؤب والمضغ (خاصةً العلكة) إلى الحد الأدنى، تجنب الصراخ أو الغناء أو أي شيء يجبر الفم على الانفتاح بشكل واسع.
- تجنب بعض الوضعيات المؤذية مثل استناد الذقن على اليد أو وضع الهاتف بين الأذن والكتف.
- إبقاء الأسنان العلوية والسفلية متباعدة قليلاً عن بعضها قدر المستطاع، سيؤدي ذلك إلى تخفيف الضغط على المفصل، كما يمكن وضع اللسان بين الأسنان للحد من الصرير أثناء النهار.
- إجراء بعض تقنيات الاسترخاء للمساعدة في إرخاء الفك، قد ينصح طبيب الأسنان إجراء العلاج الطبيعي أو التدليك، وكذلك الارتجاع البيولوجي.
العلاجات التقليدية لاضطرابات المفصل الفكي الصدغي:
هناك بعض العلاجات المجربة التي قد يصفها طبيب الأسنان لعلاج اضطرابات مفصل الفك.
- الأدوية: يمكن للطبيب أن يصف جرعات أعلى من مضادات الالتهاب غير الستيروئيدية NSAIDs للتخفيف من الألم والتورم في المفصل، قد يوصي الطبيب بالمرخيات العضلية وذلك لإرخاء الفك خاصةً عند مرضى الصرير، أو دواء مضاد للاكتئاب للتخلص من التوتر والذي قد يسبب يزيد من اضطرابات المفصل الفكي الصدغي.
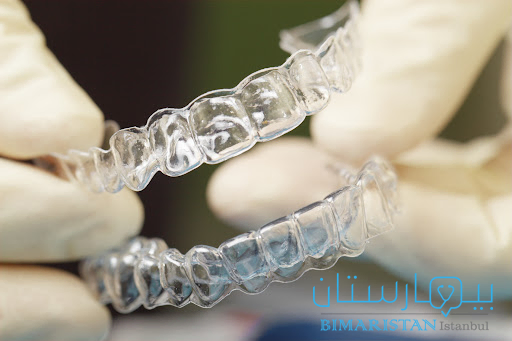
- الجبيرة أو واقي الصرير الليلي: تكون هذه القطع الفموية مناسبة للأسنان حيث توضع على الأسنان العلوية والسفلية كي تمنع تلامسهما فتعمل بذلك على تقليل آثار الصرير أو الضغط على الأسنان وتصحح العضة عن طريق وضع الأسنان في وضع أكثر راحة.
ما هو الفرق بينهما؟ يستعمل واقي الصرير الليلي أثناء النوم في حين أن الجبيرة تستخدم في كل وقت، إن مهمة طبيب الأسنان إخبار المريض بالنوع الذي يحتاجه.
- المعالجات السنية، يمكن لطبيب الأسنان استبدال الأسنان المفقودة واستخدام التيجان أو الجسور أو التقويم لموازنة أسطح العض في الأسنان أو لتصحيح مشكلة العض لدى المريض.
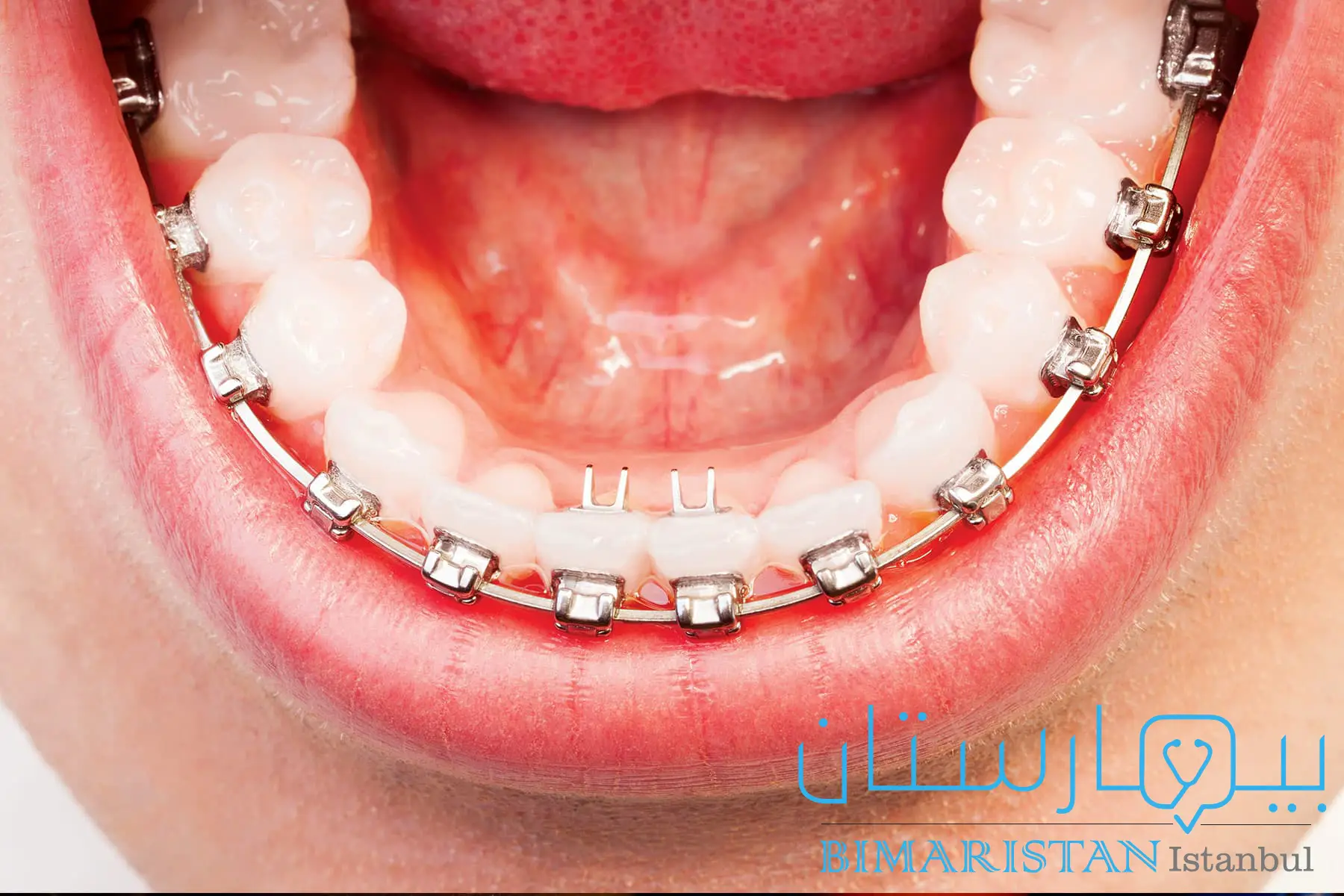
علاجات أخرى لاضطرابات المفصل الفكي الصدغي:
في حال لم تنفع العلاجات التقليدية المذكورة سابقاً، قد يعمد طبيب الأسنان إلى واحد أو أكثر مما يلي:
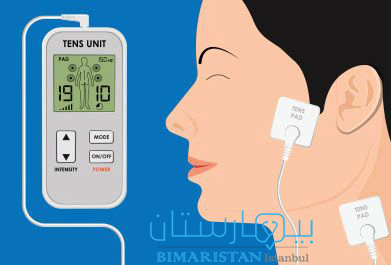
- التحفيز الكهربائي للأعصاب عبر الجلد TENS يستخدم هذا العلاج تيارات كهربائية منخفضة الشدة لتخفيف الآلام عن طريق إرخاء مفصل الفك وعضلات الوجه، يمكن إجراء هذا العلاج في عيادة طبيب الأسنان أو في المنزل.
مخدر موضعي مثل الليدوكائين، الذي يحصر مستقبلات الألم في العضلات.
كورتيكوستيروئيد، الذي يقلل الالتهاب في العضلات والنسيج الضام المحيط بالعصب
توكسين البوتولينوم (البوتوكس)، الذي يتداخل مع مسارات الإشارات العصبية ويمنع تقلصات العضلات.
أثناء الحقن يقوم الطبيب بإدخال إبرة صغيرة في نقطة تحفيز اللفافة العضلية ويحقن الدواء فيها، قد يشعر الأشخاص الذين لديهم توتر في العضلات بشكل خاص بإحساس طاحن عندما يقوم الطبيب بإدخال الإبرة، وعادةً ما ينحسر هذا الشعور مع ارتخاء العضلات.
- العلاج بموجات الراديو، تعمل موجات الراديو على تنشيط المفصل مما يزيد من تدفق الدم ويخفف الألم.
- العلاج بالليزر منخفض المستوى، يقلل هذا العلاج الألم والالتهاب ويساعد المريض على تحريك رقبته بحرية أكبر وفتح فمه على نطاق أوسع.
جراحة اضطراب المفصل الفكي الصدغي:
في حال فشل جميع العلاجات السابقة تأتي الجراحة كخيار أخير.
يجب على المرض أخد رأي طبيبين أسنان أو أكثر قبل اللجوء إلى الجراحة.
هناك ثلاثة أنواع من جراحات اضطرابات المفصل الفكي الصدغي، يعتمد النوع الذي يحتاجه المريض على نوع المشكلة لديه.
- بزل المفصل الفكي الصدغي وغسله:
تشمل التقنيات الجراحية الباضعة بالحد الأدنى ثقب المفصل (بزله) حيث تُسحب السوائل من المفصل باستخدام إبرة خاصة، وفي حال وجود التهاب غالباً ما تتجمّع السوائل الالتهابية في الحفرة العليا من المفصل، ويدعى ذلك “انصباب المفصل الفكي الصدغي”.
يُصرَّف هذا التجمع من السوائل المفصلية الحاوية على الكثير من المركبات البروتينية الالتهابية المؤذية أولاً، ثم تتمدد الحجرة المفصلية وتتحرر المحفظة المفصلية، ويصبح بإمكان القرص التحرك مباشرة بصورة أفضل في المفصل، ثم يُثقب الحيز المفصلي بإبرة أخرى ويُغسل بما يقارب 200 مل من محلول ملحي معقم، ولا ينحصر تأثير سائل الغسيل في التخلص من البروتينات الالتهابية المؤذية في الحيز المفصلي بل أيضاً في طبقات أعمق من المحفظة المفصلية والغضروف الليفي المفصلي.
الخطوة التالية هي حقن حمض الهيالورونيك أو دواء غيره داخل الحيز المفصلي، وبهذا أخيراً يصبح القرص المفصلي قادر على الحركة بسهولة وينحسر أي خلل في وظيفة المفصل.
تُجرى هذه التقنية تحت تأثير التخدير العام، وهي مناسبة لمعالجة جميع أشكال الالتهابات في المِفصل الصدغي، وفي حالات الانزياح غير الردود للقرص المفصلي، فيمكن لهذه الطريقة أن تستخدم لتصحيح توضع القرص المفصلي بسرعة، ويجب دوماً أن يكون ذلك مصحوباً مع المعالجة بالجبائر والمعالجة الفيزيائية.
- جراحة تنظير المفصل:
تتم باستخدام منظار المفصل، وهو أداة خاصة لها عدسة وضوء، يمكن المنظار الطبيب من رؤية ما بداخل المفصل، يوضع المريض تحت تأثير التخدير العام، ثم يقوم الطبيب بعمل شق صغير أمام الأذن ويدخل المنظار الموصول مسبقاً بشاشة عرض، حتى يتمكن من فحص المفصل والمنطقة المحيطة به، قد يقوم أيضاً بإزالة الأنسجة الملتهبة في المفصل.
يسمى هذا النوع من الجراحة باسم الجراحة طفيفة التوغل، ومن صفاتها أنها تترك ندبة أصغر، ولها مضاعفات أقل، وتتطلب وقت شفاء أقصر من الجراحة الكبرى.
- جراحة المفصل المفتوح:
اعتماداً على سبب اضطرابات المفصل الفكي الصدغي، قد لا يكون تنظير المفصل ممكناً، حيث يحتاج المريض إلى هذا النوع من الجراحة إذا:
كان هناك تآكل في البنى العظمية للمفصل
كان هناك أورام في المفصل أو حوله.
وُجد تشقق في المفصل.
يحصل المريض في هذه الجراحة على التخدير العام، ثم يقوم الطبيب بفتح المنطقة المحيطة بالمفصل بالكامل حتى يتمكن من الحصول على رؤية كاملة ووصول أفضل.
يحتاج المريض إلى وقت أطول للشفاء بعد جراحة المفصل المفتوح، وهناك فرصة أكبر للتندب وإصابة الأعصاب المحيطة.
بعض التمارين المفيدة لعلاج اضطرابات المفصل الفكي الصدغي:
تهدف هذه التمارين إلى استعادة نطاق واسع لحركة الفك تدريجياً وتقليل أي إزعاج يسببه المفصل الفكي الصدغي، تستهدف هذه التمارين بشكل أساسي عظم الفك السفلي الموجود في قاعدة الجمجمة، وتستهدف أيضاً عضلات الحلق والرقبة على نطاق أوسع.
- تمرين السمكة الذهبية Goldfish Exercise: يساعد هذا التمرين على الحصول على محاذاة صحيحة لعظم الفك السفلي أثناء المضغ.
الخطوة 1: اضغط بلسانك على سقف فمك.
الخطوة 2: الآن ضع إصبع السبابة على المفصل الفكي الصدغي الأيسر وإصبع السبابة الآخر على ذقنك.
الخطوة 3: أسقط ذقنك نحو الأسفل، واستخدم ضغطاً خفيفاً بكل إصبع وحافظ على اللسان في سقف الفم، كرر هذا التمرين لمفصل الفك الصدغي الأيمن.
كرر هذا التمرين ست مرات في كل مجموعة، قم بإجراء ست مجموعات يومياً.

- تمرين تثبيت الفك السفلي Mandibular Stabilization Exercise: يساعد هذا التمرين بالمثل على محاذاة عظم الفك السفلي وتحسين نطاق حركته بمرور الوقت.
الخطوة 1: ضع الفك في وضع محايد ومريح.
الخطوة 2: ضع إبهامك على قاعدة الفك، أسفل الذقن مباشرة، واضغط برفق أثناء فتح فمك.
الخطوة 3: كرر الحركة، وحرك إبهامك إلى الجانبين الأيسر والأيمن من الفك على التوالي.
كرر هذا التمرين خمس مرات في كل مجموعة، قم بإجراء خمس مجموعات يومياً.