التهاب ماحول التاج أو التواج هو تورم وإصابة أنسجة اللثة حول ضرس العقل ويكون أكثر شيوعاً حول ضرس العقل السفلي، سنتعرف على أعراضه وعلاجه في تركيا من خلال المقال.
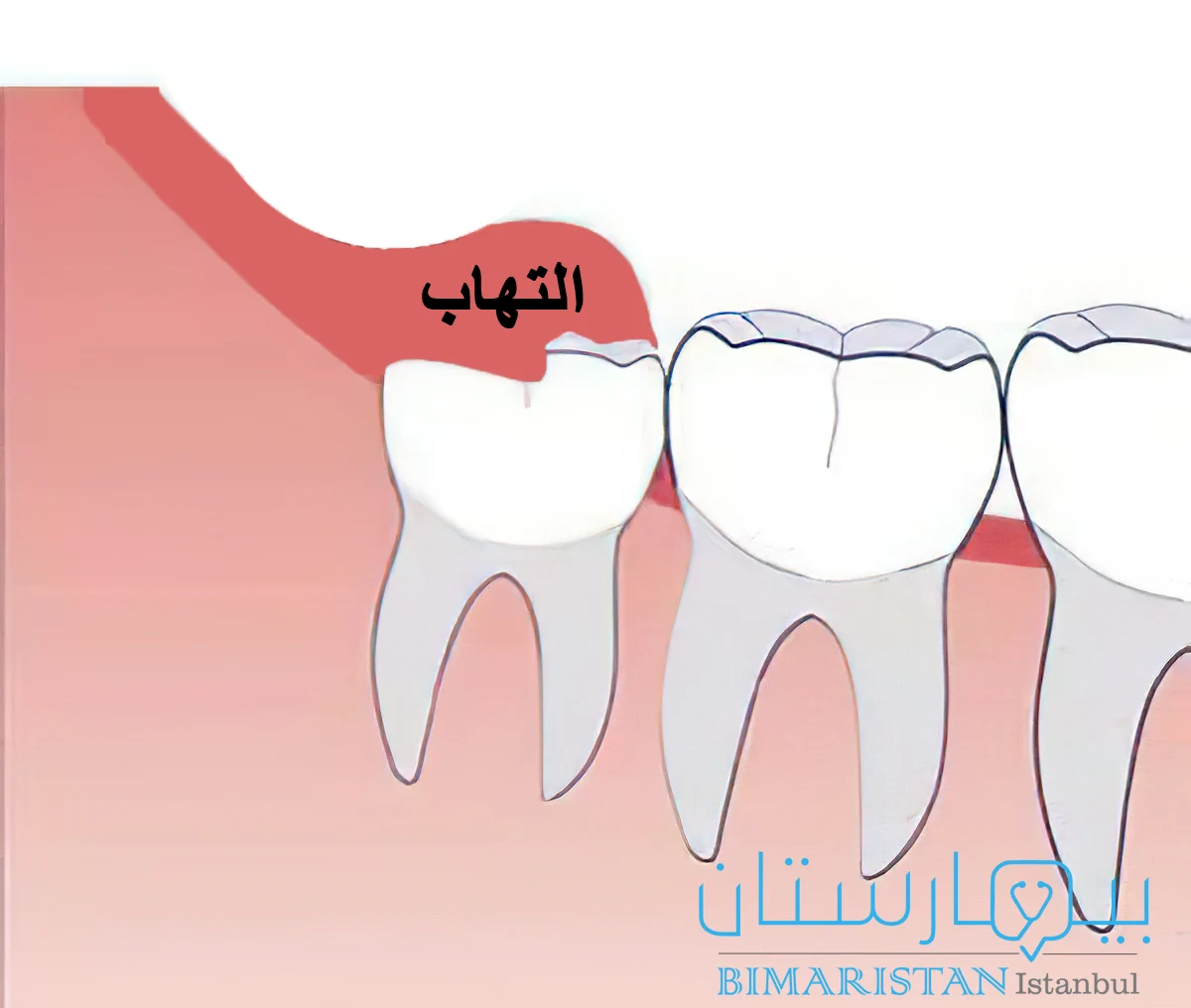
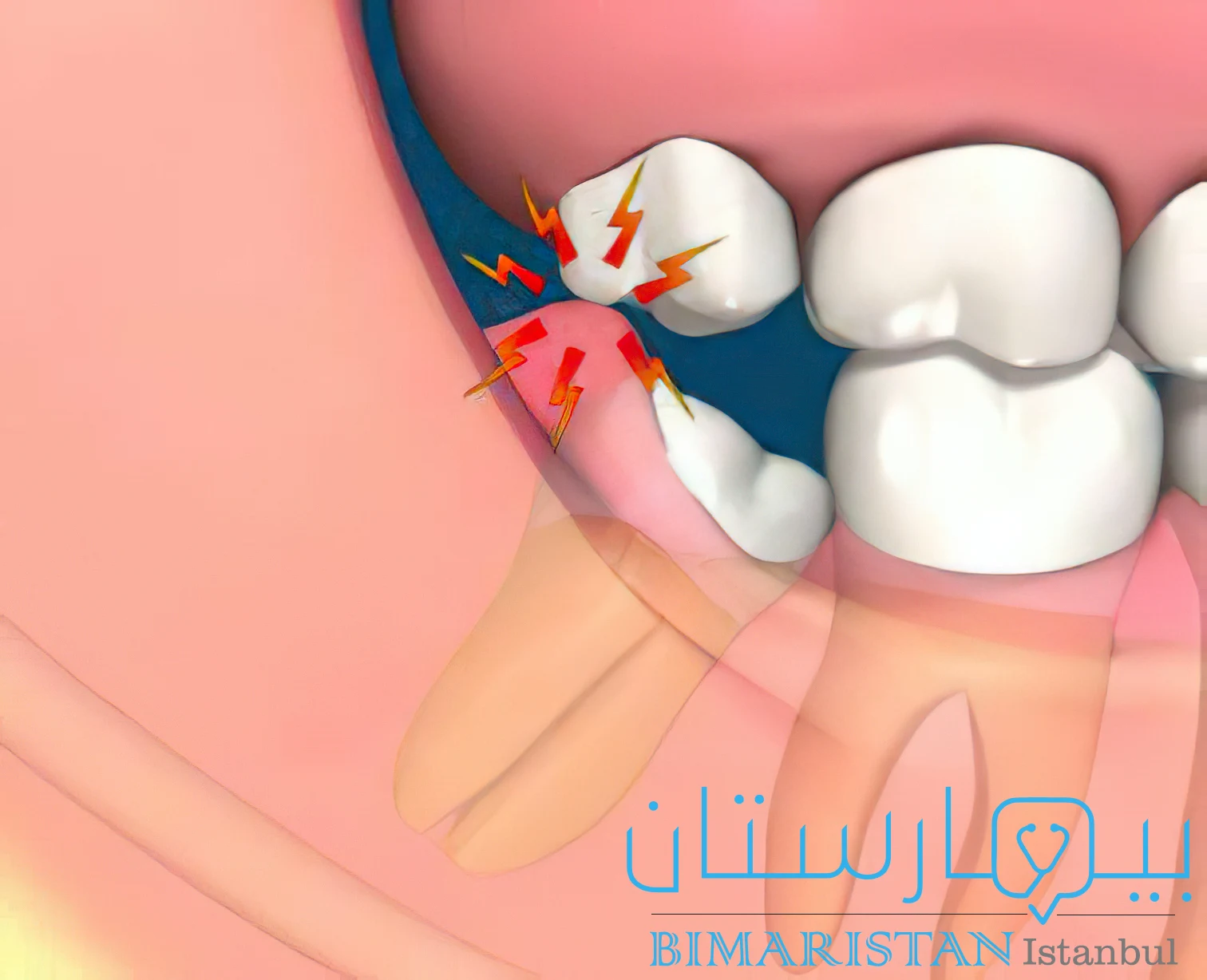
التهاب ما حول تاج السن حالة التهاب شائعة في الأعمار العشرينية يحدث عندما لا يكون للضرس مساحة كافية للبزوغ فيخرج جزئياً فقط من اللثة مما يؤدي إلى التهاب نسيج اللثة المحيط بالضرس، تحدث عادةً حول ضروس العقل وهي المجموعة الثالثة والأخيرة من الأضراس التي تبزغ لدى معظم الناس في أواخر سن المراهقة أو أوائل العشرينات.
أسباب التهاب ماحول التاج
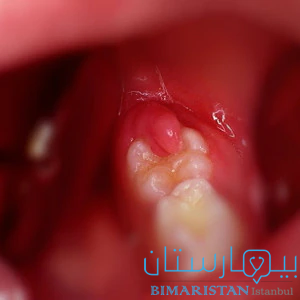
يمكن أن يحدث التهاب ماحول التاج pericoronitis عندما تبرز ضروس العقل جزئياً فقط عبر اللثة، يسمى نمو الأنسجة الرخوة فوق ضرس العقل البازغ جزئياً حينها بالرف اللثوي.
يمكن أن تنحصر بقايا الطعام بعد الأكل تحت الغطاء اللثوي مما يسمح للبكتيريا بالدخول حول الأسنان والتسبب في العدوى والتورم.
إذا بقيت هناك يمكن أن تهيج اللثة وتؤدي إلى التهاب حوائط التاج وفي الحالات الخطيرة قد يمتد التورم والعدوى إلى ما وراء الفك إلى الخدين والرقبة وينتشر مسبباً خناق لودفيغ وهي حالة مهددة للحياة.
عوامل خطر التهاب ماحول التاج
تتضمن العوامل التي قد تزيد من خطر الإصابة بالتهاب ماحول التاج أو التهاب محيط التاج ما يلي:
- أن تكون في العشرينات من العمر
- التهابات الجهاز التنفسي العلوي
- الضغط النفسي
- صحة فموية سيئة
أعراض التهاب ماحول التاج
يمكن أن تكون أعراض التهاب ماحول التاج حادة قصيرة المدى أو مزمنة مستمرة.
تشمل الأعراض الحادة:
- ألم
- التورم حول السن والتهاب اللثة بسبب تراكم السوائل
- نز قيحي
- ضزز أو صعوبة فتح الفم والفك
- ألم عند البلع
- حمى
- فقدان الشهية
- إنتان وعدوى
- تورم العقد اللمفاوية تحت الفك السفلي في الرقبة
تشمل الأعراض المزمنة:
- ألم خفيف في بعض الأحيان أو انزعاج خفيف
- الشعور بطعم سيء في الفم
تشخيص التهاب ماحول التاج
سيقوم طبيب الأسنان بفحص ضروس العقل لمعرفة وضعية بزوغها وتحديد ما إذا كانت قد بزغت جزئياً.
قد يأخذ أشعة سينية بشكل دوري لمعرفة توضع ضرس العقل ويلاحظ طبيب الأسنان أي أعراض مثل التورم أو العدوى ويتحقق من وجود الرف اللثوي حول ضرس العقل.
علاج التهاب ماحول التاج
يعالج التهاب حوائط التاج أو التهاب محيط تاج السن من قبل طبيب الأسنان العام أو أحد هؤلاء الأخصائيين:
- طبيب أسنان الأطفال أو طبيب أسنان الأطفال
- أخصائي عصب الاسنان
- اللثة
- التركيبات السنية
- جراح الفم
وتشمل علاجات التهاب ماحول التاج ما يلي:
نظافة الفم
إذا كانت أعراض التهاب ماحول التاج موضعية في المنطقة المحيطة بالسن ولم ينتشر فقد يجرب طبيب الأسنان الاكتفاء بالقيام بتنظيف المنطقة جيداً وإزالة أي بقايا طعام مع تصريف أي صديد، ستحتاج إلى التأكد من إبقاء اللثة خالية من أي بقايا طعام منحصرة.
مسكنات الألم
يمكنك تناول مسكنات الألم مثل الأسبرين أو الأسيتامينوفين أو الإيبوبروفين، قد يصف لك طبيب أسنانك أيضاً مسكنات للألم.
المضادات الحيوية
إذا حدث انتفاخ وألم في منطقة الأسنان والفك والخد منتفخة استشر طبيب الأسنان على الفور يمكنهم علاج العدوى بالمضادات الحيوية بعد إجراء اختبار الحساسية.
العلاج الجراحي
إذا كان الألم والالتهاب شديدين أو إذا تكرر التهاب ماحول التاج فقد يكون من الضروري إجراء جراحة الفم لإزالة اللثة أو ضرس العقل، يمكن لطبيب الأسنان الخاص بك إجراء الإحالة المناسبة إلى جراح الفم والوجه والفكين.
من المهم الإسراع بمعالجة أعراض التهاب ماحول التاج بسرعة لمنع انتشار العدوى وتقليل مخاطر حدوث المضاعفات.
يمكن استخدام ليزر منخفض المستوى لتقليل الألم والالتهاب المرتبط بالتهاب ماحول التاج.
الخلع
إذا كان ضرس العقل لا يزال غير قادر على البزوغ بشكل طبيعي فقد تحتاج إلى عملية جراحية لإزالته قد يوصي طبيب الأسنان بخلع ضرس العقل العلوي والسفلي لمنع الأسنان العلوية من العض على اللثة والتسبب في عدوى أخرى.
المضاعفات المحتملة
يمكن ظهور عدة مضاعفات مرتبطة إذا لم يتم علاج الأعراض على الفور، أهم مضاعفات التهاب ما حول التاج:
- قد تنتشر العدوى من المنطقة المصابة مما يؤدي إلى حدوث تورم وألم في أجزاء أخرى من الرأس والرقبة.
- الضزز، حيث يجد الشخص صعوبة في فتح الفم أو العض.
- في حالات نادرة يمكن أن تكون مضاعفات التهاب ماحول التاج مهددة للحياة، حيث يمكن أن يؤدي عدم علاج التهاب ماحول التاج إلى حصول ذبحة لودفيغ وهي عدوى تنتشر تحت الفك واللسان.
- يمكن أن تسبب هذه الحالة التهابات عميقة أخرى في الرأس أو الرقبة أو الحلق.
- هناك أيضاً احتمال أن تنتشر العدوى في مجرى الدم، في حالة تُعرف باسم تجرثم الدم والتي يمكن أن تكون مهددة للحياة.
بعد العلاج
عادة لا يسبب التهاب ماحول التاج أثراً على المدى الطويل، إذا بزغ ضرس العقل بالكامل أو تمت إزالته فلن يتكرر التهاب ماحول التاج في تلك المنطقة.
عند نزع السن يمكن أن يتوقع الشخص عادة الشفاء التام بعد حوالي أسبوعين، أثناء الشفاء يمكن أن يحدث ما يلي:
- تصلب الفك
- طعم سيء في الفم
- تورم
- الشعور بالألم
- ووجود وخز أو تنميل في الفم والوجه (أقل شيوعاً)
من الضروري اتباع جميع تعليمات الرعاية اللاحقة، يجب على الشخص الاتصال بطبيب الأسنان أو جراح الفم إذا كان يعاني من ألم شديد أو نابض أو حمى أو نزيف.
إن أهم شيء في علاج التهاب غلاف التاج هو ضمان حصول الشخص على العلاج المناسب بحيث يمكن علاج هذه الحالة المؤلمة في أسرع وقت ممكن.
الوقاية من التهاب ما حول التاج
تشمل الخطوات التي يمكن للأشخاص اتخاذها لمحاولة تقليل فرصة الإصابة بالتهاب ماحول التاج ما يلي:
نظافة الفم الجيدة
من الجيد التنظيف الإضافي حول السن المصابة لإزالة بقايا الطعام والبكتيريا.
الزيارات المنتظمة لطبيب الأسنان
ستساعد الفحوصات المنتظمة طبيب الأسنان على تحديد أي علامات أو مشاكل مرتبطة بالتهاب ماحول التاج مما يزيد من فرصة علاجه مبكراً.
اتخاذ إجراءات وقائية
يوصى بالاتصال بطبيب الأسنان عندما يكون لدى الشخص أي مخاوف بشأن تطور التهاب ماحول التاج، يمكنك التواصل هنا مع مركز بيمارستان للحصول على معلومات أكثر أو لحجز المواعيد.
المصادر