Colonoscopy is one of the most important tests performed to detect diseases and abnormal changes in the colon and is used for diagnostic or therapeutic reasons, depending on the case.
Overview of the colon
The colon is the largest part of the large intestine, measuring about 150 centimeters in length. The colon absorbs water and salts from waste before it is excreted, as the colon forms a passage for feces to pass into the rectum, and then out of the body through the anus.
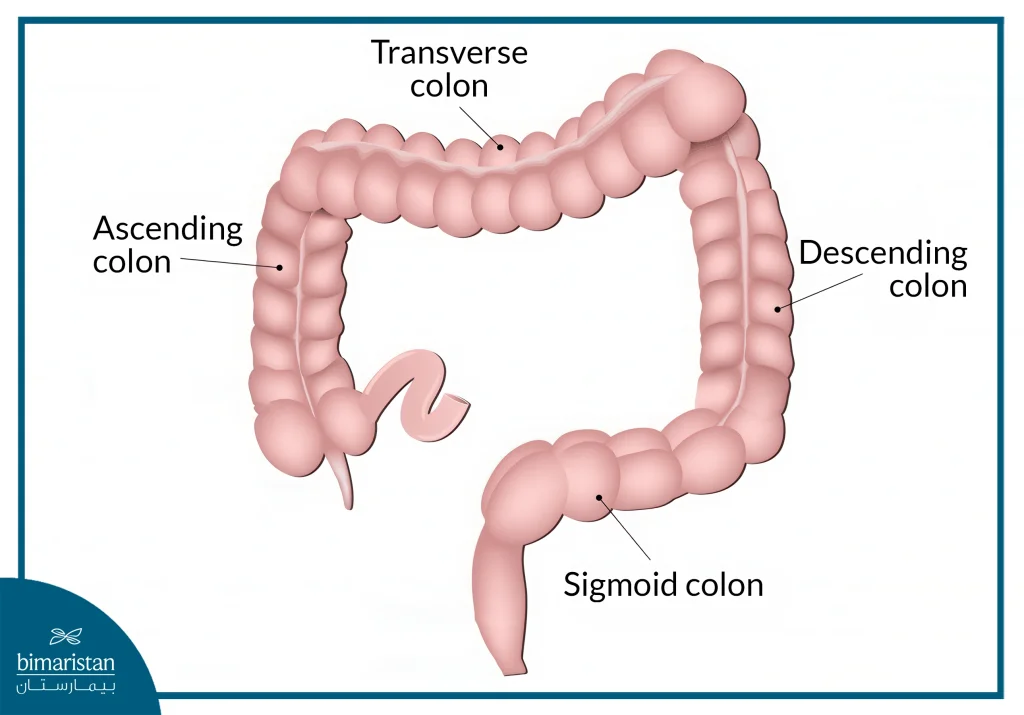
The colon is anatomically divided according to its location into four sections:
- Ascending colon
- Transverse colon
- descending colon
- Sigmoid colon
What is a colonoscopy?
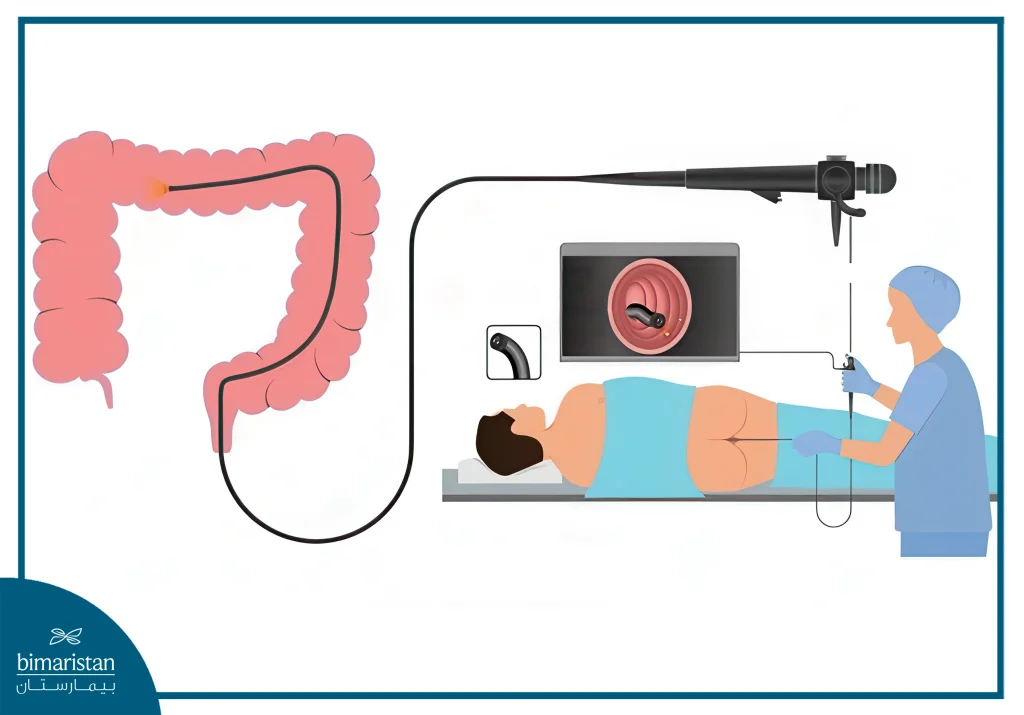
In a colonoscopy, the doctor inserts a long, flexible tube with a camera underneath through the anus into the rectum and into the distal parts of the colon.
The endoscope is connected to a screen where what the camera captures is displayed on the screen, enabling the examiner to see and examine the colon and identify pathological changes, if any.
During the colonoscopy, the patient is anesthetized so that no pain is felt. Endoscopy can be used for therapeutic reasons, meaning that if a mass is suspected in the colon, a biopsy can be taken to examine it, and healthy masses and polyps can also be removed through endoscopy.
Why is a colonoscopy used?
The doctor advises the patient to have a colonoscopy for one of the following reasons:
- Digestive symptoms such as bleeding, abdominal pain, and chronic constipation or diarrhea.
- Detect colorectal cancer and the presence of polyps in the colon.
- Suspected inflammatory bowel diseases such as ulcerative colitis and Crohn’s disease.
- Colonoscopy is routinely performed in patients who have an increased risk of colorectal cancer, such as a family history or advanced age.
Preparing before a colonoscopy
There are some guidelines that the patient must follow before the colonoscopy in order to clear the colon of feces that impede the entry of the scope so that the examiner can get a clear view of the colon.
Diet before endoscopy
Certain foods such as corn, nuts, and red meat should be avoided about three days before the endoscopy, and a low-fiber diet is recommended several days before the endoscopy.
You should refrain from eating solid foods and alcohol the day before the procedure and not eat at all four hours before the endoscopy.
The most important thing is to follow your doctor’s dietary instructions.
Drinking laxatives
The doctor often advises the patient to take laxatives before the endoscopy, either in the form of pills or in the form of a drink that the patient drinks. Laxatives are recommended to be taken the night before or the morning of the endoscopy.
Modification of certain medications
The doctor may ask the patient to modify some medications before the endoscopy procedure or reduce the dose taken. For example, if the patient is taking blood-thinning medications such as warfarin, it can be temporarily stopped before the endoscopy procedure to reduce the risk of bleeding.
Patients are advised to take a driver or family member with them to the hospital or clinic where the endoscopy is performed. The reason behind this is that the patient may be anesthetized during the endoscopy, so someone else will need to drive for them on the way back.
During a colonoscopy
A colonoscopy is performed either in a hospital or outpatient setting by a doctor who is experienced in the procedure.
During the procedure, the patient wears a special gown, lies on his left side, and raises his knees towards his chest (fetal position). The patient is anesthetized with either regional anesthesia, which means the patient remains awake without feeling any pain, or in some cases, general anesthesia is administered.
The examiner inserts a colonoscope through the rectum, and the scope is equipped with a camera and is long enough to reach all parts of the colon. The scope contains a small lamp and a channel that enables the doctor to release air through it; the air works to expand the colon and give the doctor a clearer view.
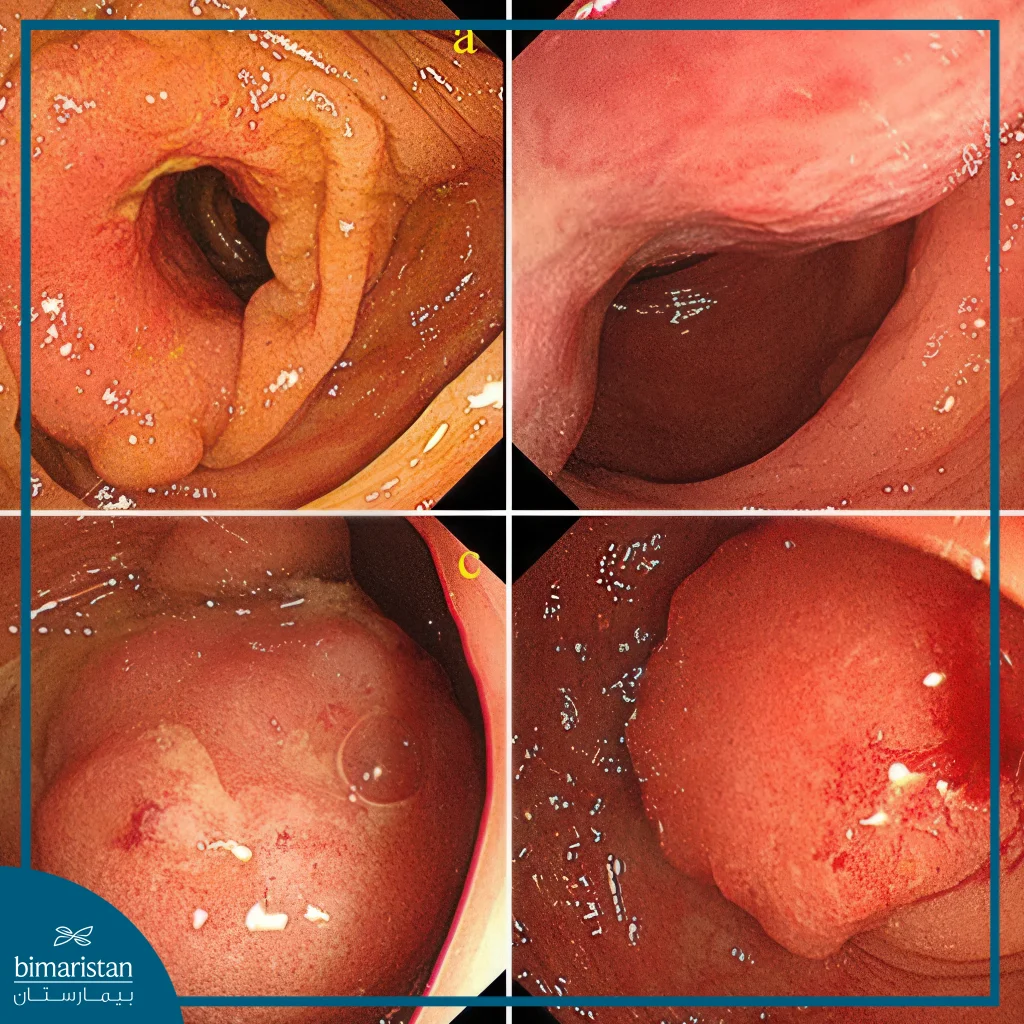
The doctor looks for any abnormal changes in the colon and may take a biopsy if a cancerous mass is suspected. If a polyp is found, the doctor will remove it.
After completing the examination, the doctor gently pulls out the scope. The patient may feel cramps during the withdrawal, which can be relieved by resting and taking a deep breath.
A colonoscopy takes about half an hour or less in normal cases, but it may take longer if a polyp or mass is found.
After a colonoscopy
After the endoscopy, the patient remains in the hospital to recover and make sure there are no complications related to the endoscopy. The recovery period depends on the type of anesthetic the patient received during the endoscopy.
Avoid driving or strenuous activities for at least 24 hours after the procedure, and avoid alcohol and smoking for at least a day after the procedure.
The patient may experience temporary abdominal cramps or abdominal colic that go away quickly. Due to the complete emptying of the colon, the patient may not have a bowel movement for several days after the colonoscopy. If the doctor removes a polyp during the colonoscopy, the patient may notice mild rectal bleeding for a day or two after the colonoscopy.
After the endoscopy, the examiner will determine the need to discontinue or adjust medications.
Colonoscopy results
After the endoscopy, the doctor explains to the patient what happened during the endoscopy in case a polyp was removed or an abnormal tissue was suspected and a biopsy was taken.
The results of the endoscopy are either:
Negative endoscopy results
In other words, no abnormal changes were detected at the level of the colon and rectum, meaning that the examination was normal and there is no cause for concern or fear, and the doctor advises the patient to repeat the colonoscopy during:
- 10 years if there is no risk factor for colon cancer.
- 5 years if there are previous polyps that have been removed.
- Yearly, if you have a high risk factor for cancer, such as familial polyposis, which significantly increases the risk of colon cancer.
Positive endoscopy results
The results are considered positive if polyps are detected during the colonoscopy or if abnormal tissue is detected in the colon.
In most cases, polyps are non-malignant, but there is a risk of the polyp becoming a cancerous lesion, so the doctor removes the polyp as soon as it is detected.
The doctor may ask the patient to repeat the endoscopy sooner if:
- The presence of two or more polyphenols
- Large polyp greater than 1 centimeter
- Polyp with a shape close to a cancerous lesion
If the doctor is unable to remove the polyps laparoscopically, the patient may be referred for surgery to remove them.
No results
This means that the doctor was unable to examine the colon clearly due to the presence of a fecal mass that obstructs the entry of the endoscope due to improper preparation by the patient before the endoscopy procedure.
In this case, the doctor will ask the patient to repeat the colonoscopy in a short period of time with good preparation.
Colonoscopy risks
Colonoscopy is generally considered a safe procedure, and the likelihood of complications is fairly low. Some of the colonoscopy-related complications that can occur are:
- Bleeding following a biopsy or laparoscopic polypectomy
- A tear in the wall of the colon or rectum
- Problems related to anesthesia
- Infection if the scope used is contaminated
- Some complications occur prior to endoscopy, such as excessive laxative use causing perianal skin irritation due to constant defecation.
Colonoscopy guidelines
It is recommended to start having regular colonoscopies at the age of 45 every ten years. A colonoscopy is the best way to minimize the risk of colorectal cancer and detect it early if it occurs.
In some cases, periodic colonoscopies should be started at an earlier age, i.e. before the age of 45, in one of the following cases
- Having a first-degree relative with colorectal cancer
- Having an inflammatory bowel disease such as ulcerative colitis or Crohn’s disease
- Having genetic diseases that increase the risk of cancer, such as familial polyposis and Lynch syndrome
Alternative tests to colonoscopy for cancer detection
There are alternative tests to colonoscopy for cancer prevention, such as:
Sigmoid colonoscopy
In fact, this test is somewhat similar to a colonoscopy, but with a sigmoid colonoscopy, the scope is shorter and is used to view only the rectum and sigmoid colon. In other words, a sigmoid colonoscopy cannot examine the entire colon.
Virtual colonoscopy
Also called CT colonography, it is a less invasive procedure than colonoscopy. The technique relies on shining several X-ray beams controlled by a computer that fuses the images together and gives a three-dimensional image of the rectum and colon.
Swallowing a capsule containing a camera
This method is actually used more for the small intestine than the large intestine, as a small pill containing a camera is swallowed and this capsule travels through the digestive tract from the mouth to the colon.
This method is often used to visualize the small intestine because it is difficult to see the colon due to its tortuosity and large size, as well as the difficulty of cleaning it to get a clear view.
Fecal transplant
A stool sample is taken and examined in the lab for occult blood, DNA testing, and immunohistochemical testing.
Relationship between colorectal cancer and colonoscopy
Colorectal cancer is one of the most common cancers affecting older adults and is the most common cancer of the gastrointestinal tract.
Colonoscopy is an essential screening test for colorectal cancer, as studies have shown:
- Cancer mortality decreased due to regular colonoscopies
- Endoscopic polypectomy led to a lower risk of polyps turning into cancer
Sources: