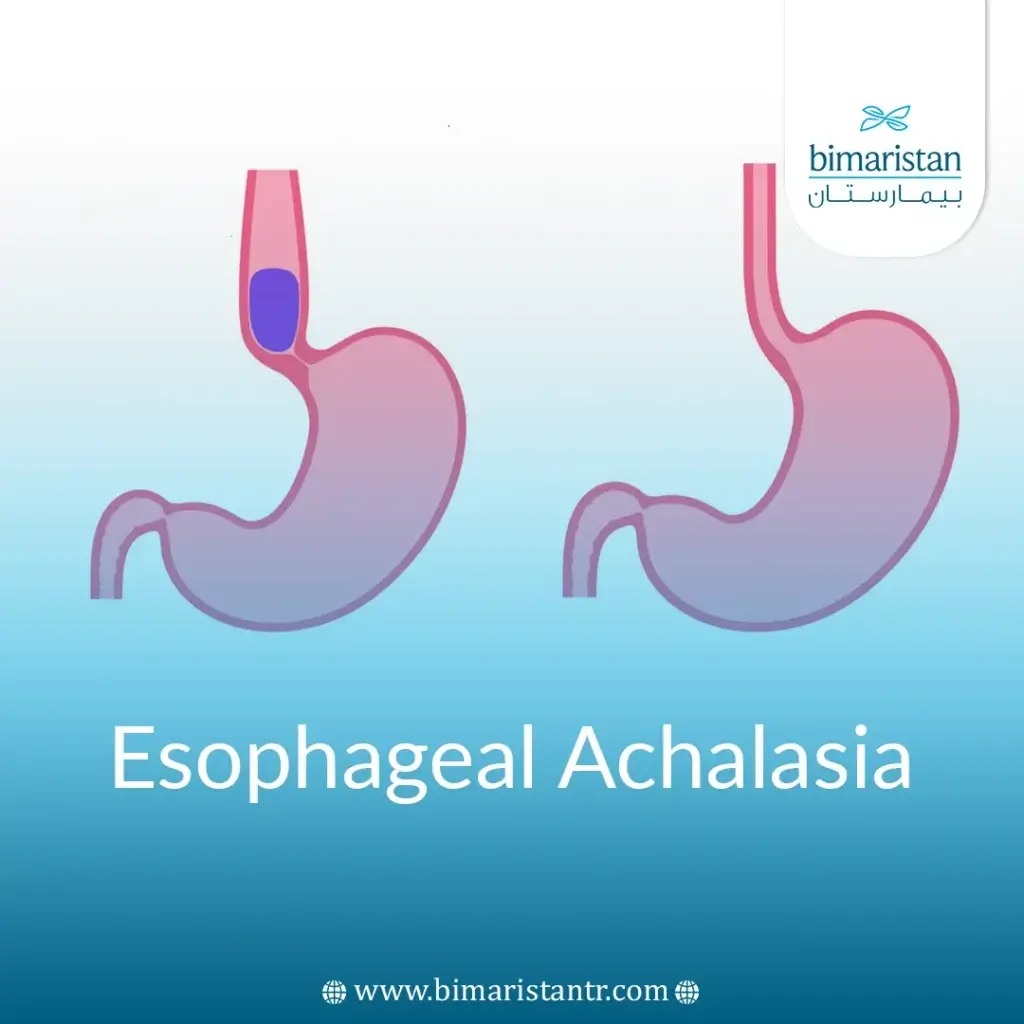
Achalasia is a rare digestive disease affecting the esophagus and preventing food from reaching the stomach. It causes many symptoms and is treated in several ways.
The symptoms of it may get worse over time if treatment is neglected. The esophageal muscles may become paralyzed due to chronic expansion of the esophagus due to the inability to push food into the stomach. You can contact us to request a free consultation on how to treat Achalasia in Turkey. Follow this article for more details.
A quick overview of the esophagus
It is a muscular tube about 25 cm long that allows food and liquids to pass from the pharynx to the stomach.
When food is eaten, the esophagus pushes it toward the stomach through peristaltic muscle contractions, which move the food and accelerate its descent into the stomach.
In the lower part of the esophagus, there is a lower sphincter. The function of the lower sphincter is to prevent the backflow of food into the stomach. The sphincter naturally relaxes when eating food and contracts when the esophagus is free of food or liquids.
In normal conditions, the lower esophageal sphincter maintains a specific pressure. This pressure keeps the sphincter contracted and prevents its relaxation and regurgitation due to stomach components.
Several digestive diseases are linked to the condition of the lower esophageal sphincter. For example, gastroesophageal reflux is one of the common diseases associated with a disorder in the functioning of the lower esophageal sphincter.
What is the achalasia definition?
Achalasia, gastric cardia spasm, or esophageal achalasia are all terms for the same disease. It affects the motility of the esophagus and impedes food’s movement to the stomach.
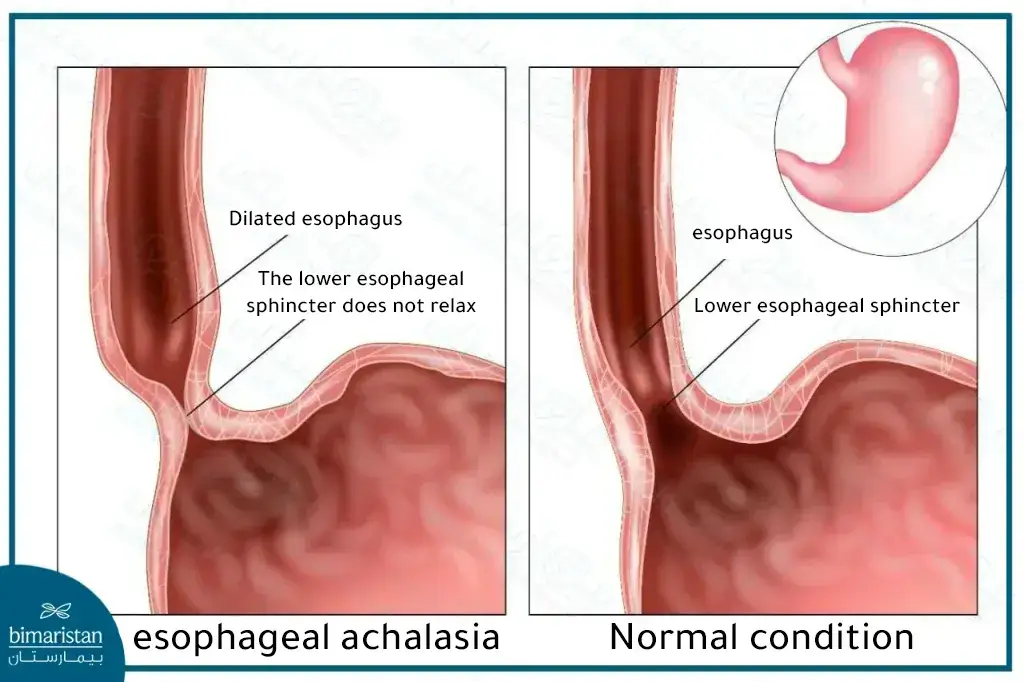
Esophageal achalasia occurs when the lower esophageal sphincter fails to relax properly during eating, obstructing food’s passage to the stomach.
Over time, the inability to relax the esophagus results in a clear expansion of the esophagus and the accumulation of food in it, which may cause the contents of the esophagus to return toward the mouth and a bad taste.
Achalasia is often accompanied by many digestive symptoms that affect the patient’s life. Some patients live with these symptoms, which are not diagnosed until later.
In the advanced stages of the disease, esophageal motility is paralyzed. When this occurs, the esophagus’s normal function cannot be restored.
The main cause of this disease is not clearly understood, but some hypotheses explain the reason for damage to the nerve plexuses responsible for esophageal motility.
Achalasia symptoms
Some patients may not suffer from anything, but the majority of people with achalasia complain of some symptoms, including:
- Difficulty swallowing combined solids and liquids (most common symptom)
- Regurgitation or reflux of undigested food
- Recurring chest pain that increases with eating
- Frequent burping
- Feeling heartburn
- Night cough
- Malnutrition and underweight (due to pain that increases while eating)
- Aspiration pneumonia (caused by inhaling contents of the digestive tract)
How is esophageal achalasia diagnosed?
It can be difficult to diagnose this disease because it is mixed with many other digestive diseases that cause similar symptoms.
A patient suffering from achalasia symptoms is diagnosed through several methods:
Barium swallow
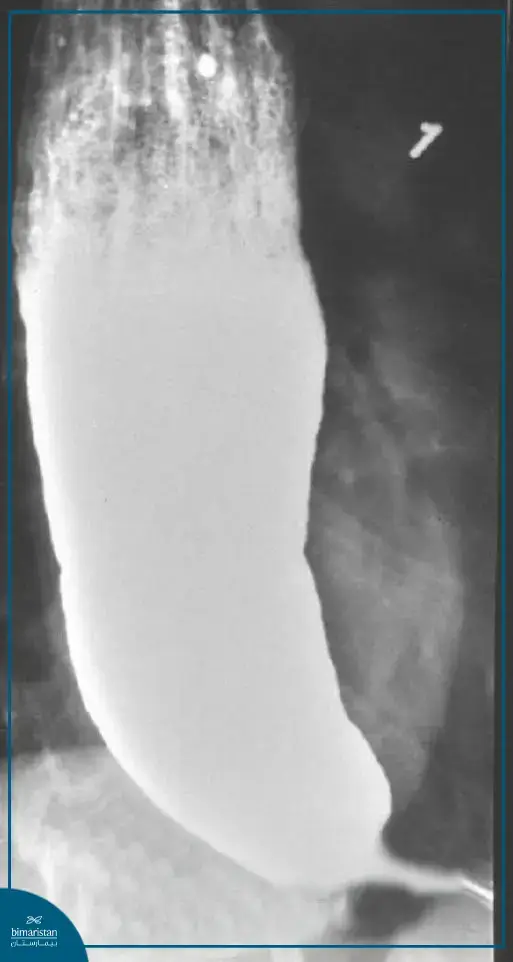
This method is important in studying diseases of the esophagus. The patient is given a contrast barium preparation, which is often in liquid form, and then an X-ray imaging of the esophagus is performed.
In achalasia, the esophagus is dilated with a narrowing at its bottom, such that it takes the shape of a bird’s beak.
Upper endoscopy
The doctor inserts a flexible tube equipped with a camera through the patient’s mouth or nose into the esophagus, through which he can also reach the stomach. Using endoscopy, the doctor can see the esophagus and evaluate the occurrence of infections or cancerous growths within it. This technique helps in evaluating the occurrence of complications of esophageal achalasia.
Esophageal manometry
It is considered the gold standard in diagnosing esophageal achalasia. This examination measures the time and strength of esophageal contractions, as well as the pressure of the lower esophageal sphincter and its ability to relax properly. If the lower esophageal sphincter fails to relax after eating, this indicates achalasia.
The test is performed by inserting a flexible tube containing special pressure sensors through the patient’s nose and into the stomach.
Achalasia treatment in Turkey
Many treatment options are available, mainly to relieve pressure on the lower esophageal sphincter so that it can relax properly and enable food to pass into the stomach.
You can contact our medical team to request a free consultation on how to treat Achalasia, with the possibility of booking an appointment for you with the best surgeons in Turkey at low prices while ensuring all travel and accommodation procedures within the Turkish country so that we can learn more about the available treatment methods.
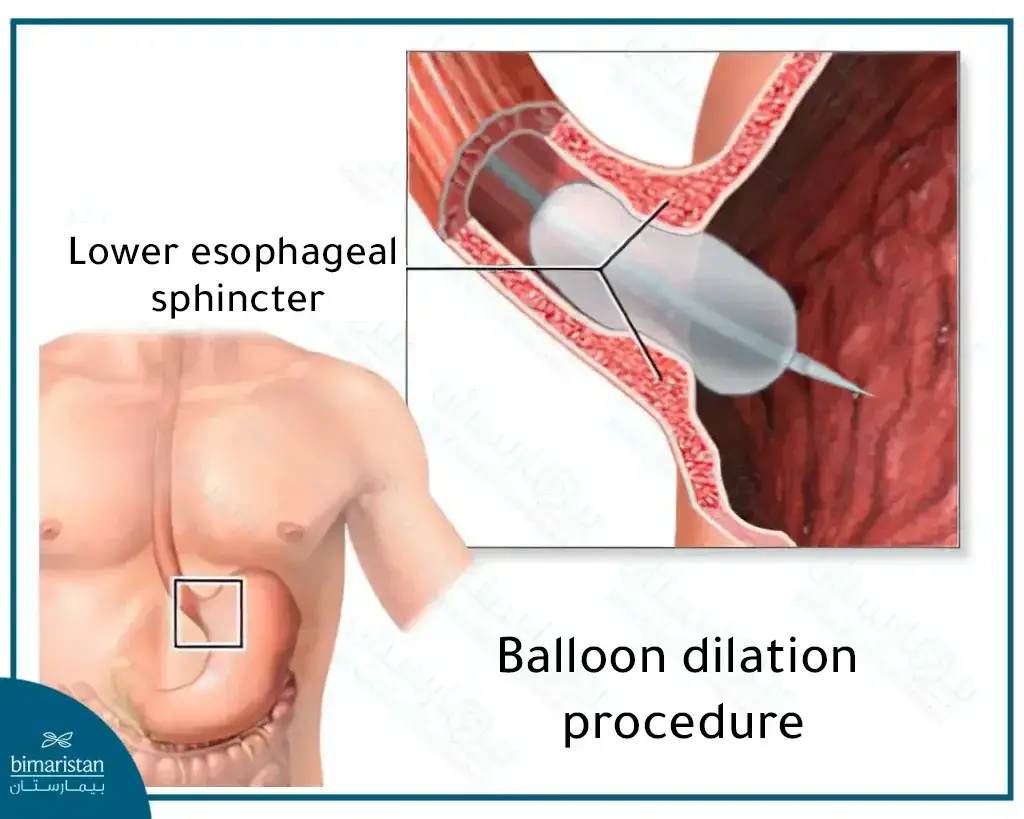
Achalasia balloon treatment
One easy-to-implement treatment method that can be performed in the outpatient clinic is to insert a balloon using an endoscope into the center of the lower esophageal sphincter and inflate it with air. This increases the width of the esophageal sphincter’s opening and facilitates food passage through it.
This procedure reduces the symptoms of the disease in about 50 to 90% of patients. However, if the symptoms of esophageal achalasia return, we may need to repeat the balloon dilatation procedure. Studies have shown that one-third of patients treated with the balloon dilation method must repeat the dilatation procedure once every five years.
Botulinum injection (Botox in the esophagus)
Botox is a muscle relaxant that helps relax the lower esophageal sphincter. It is injected directly into the sphincter via an endoscopically guided needle.
The patient may need to re-inject Botox a large number of times (once every six months). Repeated injections of Botox make surgery difficult to perform, so it is recommended to perform Botox injections in patients who are not candidates for surgery or balloon dilation.
Achalasia medication
The doctor prescribes some muscle relaxants, such as nitroglycerin, or calcium channel blockers, such as nifedipine. The effect of these drugs is weak, and their side effects are many, so drug therapy is often the last treatment option for patients who are not candidates for other achalasia treatments.
Achalasia surgery
The surgical procedures performed to manage esophageal achalasia are:
Heller’s procedure
The surgeon biopsies part of the lower esophageal sphincter muscle through the endoscope, which relieves sphincter pressure and allows food to pass more easily into the stomach.
One of the complications related to the Heller procedure is gastroesophageal reflux disease, which occurs due to excessive relaxation of the lower esophageal sphincter, which allows food to return backward.
To avoid gastric reflux, the surgeon performs a laparoscopic fold of the stomach around the lower esophageal sphincter (Nissen procedure) simultaneously with the Heller procedure.
Transoral endoscopic myotomy
In this method, the surgeon inserts the endoscope through the mouth and then makes an initial incision in the layers of the esophageal wall to reach the muscle layer. A biopsy of the muscle layer in the esophageal wall is performed, after which the lower esophageal sphincter muscle is biopsied, as is done in the Heller procedure.
The esophageal wall layers are then sutured where the surgical incision was made.
You can contact us with any questions about esophageal achalasia and how to treat it. We at the Bimaristan Center work to guide you in obtaining the best medical service in Turkey.
Sources: