Many people suffer from back pain caused by disc problems, significantly impacting their quality of life and daily activities. Epidural steroid injection is an effective treatment option that has gained popularity in Turkey, a leading country in medical advancements. This minimally invasive technique offers pain relief and improves patient well-being without requiring complex surgeries or lengthy recovery times. Epidural steroid injections have become a preferred solution for individuals seeking fast and effective treatment for disc-related back pain.
In this article, we will discuss in detail the process of epidural steroid injection in Turkey, focusing on the advantages and procedures followed and the reasons that make Turkey a preferred destination for many patients from all over the world seeking high-quality medical care.
Epidural steroid injection ESI
It is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain resulting from inflammation of the spinal nerves due to spinal stenosis or disc herniation.
The medications are delivered to the epidural area, which is a fat-filled area between the bone and the protective sac of the spinal nerves.
Pain relief may last for several days or even years.
The goal is to reduce the swelling around the nerve and thus reduce pain so that you can resume normal activities and your physical therapy program.
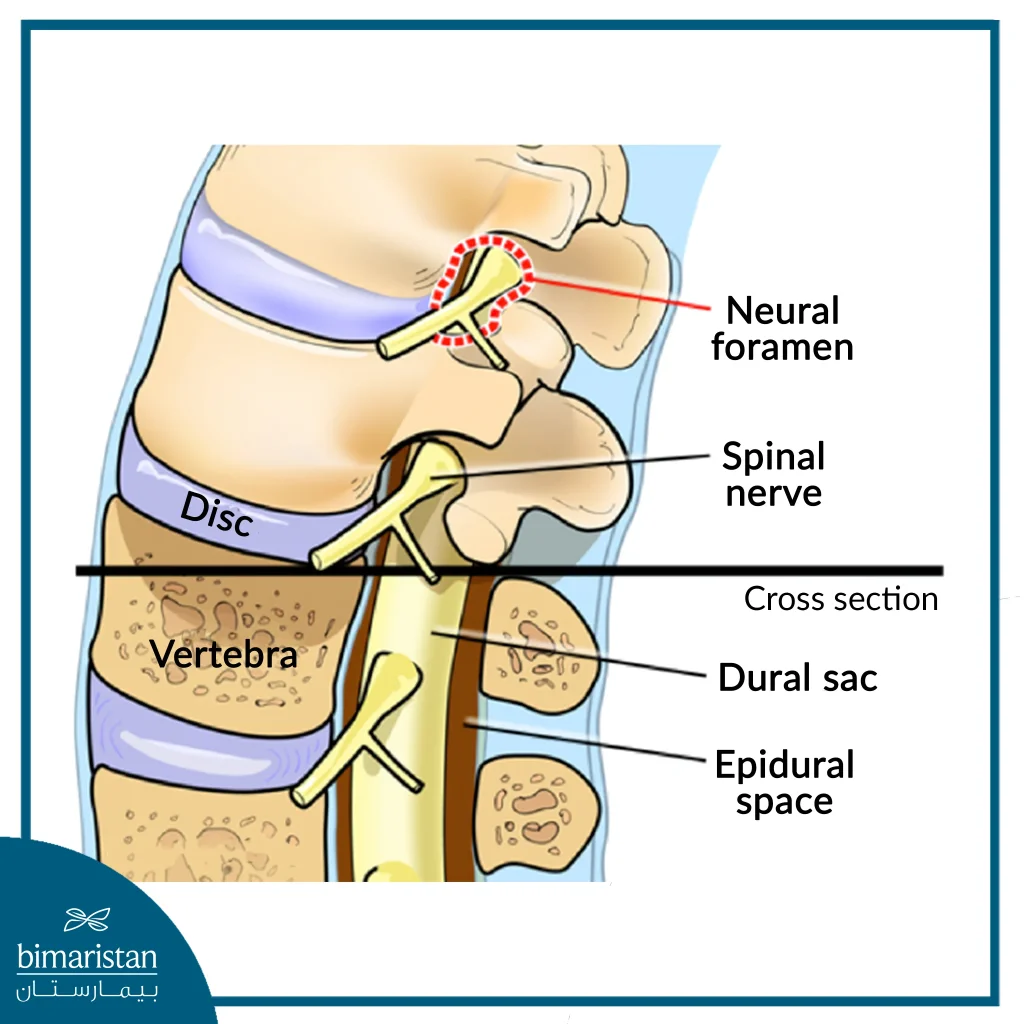
Who is a candidate for Epidural Steroid Injection ESI?
Patients with neck, arm, lower back, or leg pain (sciatica) may benefit from ESI if they have the following conditions:
- Spinal stenosis (spinal canal narrowing): Narrowing the spinal canal and nerve root canal can cause back and leg pain, especially when walking.
- Spondylolisthesis (slipped disc): Weakness or fracture between a vertebra’s upper and lower facets.
- If the vertebra slips forward, it can compress nerve roots, causing pain.
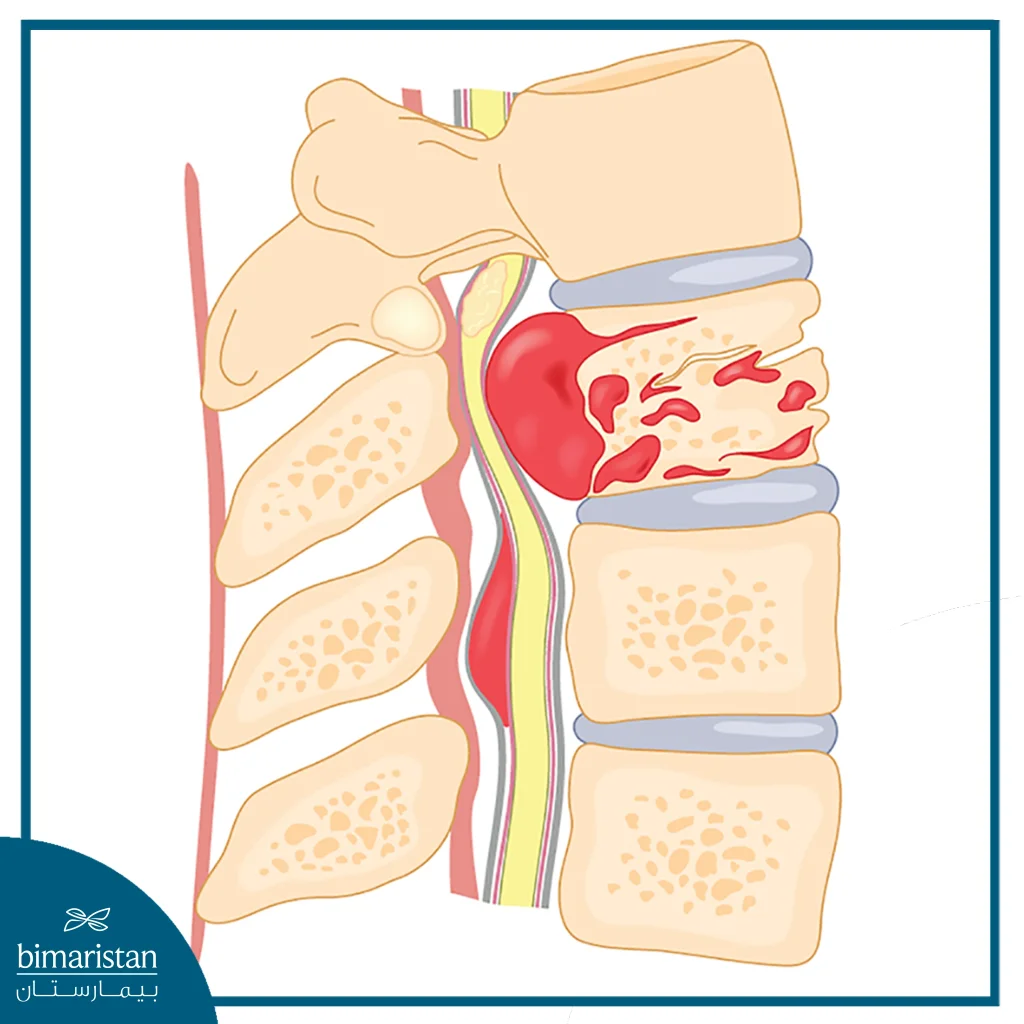
- Herniated disc: The gelatinous material inside the disc can bulge or rupture, causing irritation, pain, and swelling when this material is compressed and comes into contact with a spinal nerve.
- Degenerative disc: A breakdown or aging of the spinal disc that results in the collapse of the disc space, a tear in the annulus, and the growth of bone spurs.
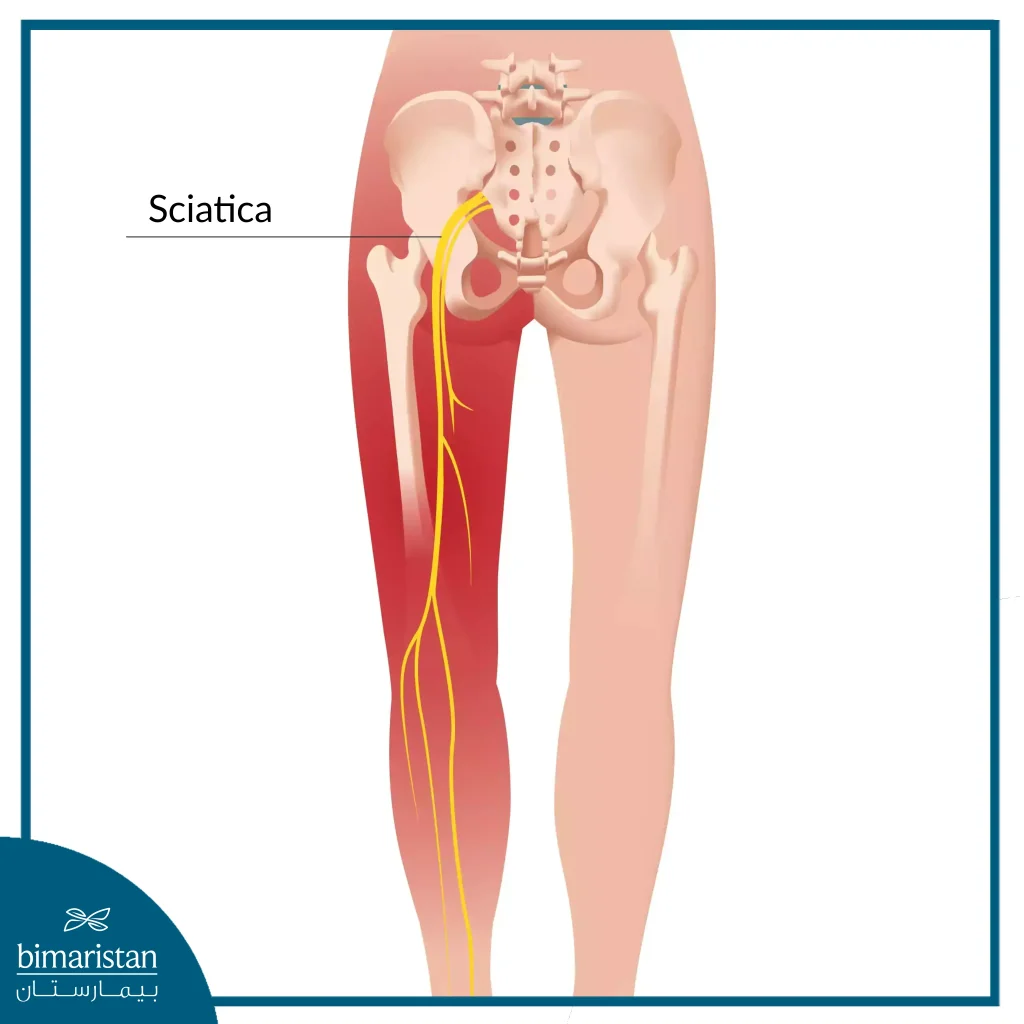
- Sciatica: Pain that radiates along the sciatic nerve into the buttocks and down the legs. Usually caused by compression of the fifth lumbar or first sacral nerve.
ESI has also been shown to be helpful for some patients in treating painful inflammatory conditions.
ESI can also help determine whether disc surgery is helpful for pain associated with a herniated disc.
When symptoms worsen with rehabilitation exercises (physical therapy), an epidural may relieve the pain enough for patients to continue with physical therapy.
ESI should not be performed on people who have an infection or bleeding problems.
The injection may cause a slight increase in blood sugar levels in people with diabetes. It may also temporarily increase blood pressure and eye pressure in people with glaucoma. You should discuss this with your doctor.
If you think you may be pregnant, tell your doctor. X-rays can be harmful to the baby.
What happens before an epidural steroid injection?
The doctor performing the procedure will review your medical history and previous imaging studies to plan the best method of injection.
Patients taking blood-thinning medications (Coumadin, Plavix, etc.) may need to stop taking them several days before an ESI. Discuss all medications with your doctors.
The procedure is usually performed in an outpatient center using X-ray fluoroscopy. Arrange for someone to drive you to and from the center on the day of the injection.
What happens during an epidural steroid injection?
At the time of the procedure, you will be asked to sign consent forms, list the medications you currently take, and indicate if you have any allergies to them. The procedure can take 15-45 minutes and is followed by a recovery period.
The goal is to inject the medication as close to the painful nerve as possible. The type of injection depends on your condition and whether you have metal rods or screws from previous surgery. Your doctor will decide which type will most likely produce the best results.
Step 1: Preparing the Patient
The patient lies on the X-ray table. A local anesthetic is used to numb the treatment area so that pain is minimal throughout the procedure. The patient remains awake and alert during the injection to provide feedback to the doctor.
Low-dose oral painkillers, such as Valium or Versed, may be given depending on the center.
Step 2: Inserting the Needle
With the help of an X-ray scope, the doctor guides a hollow needle through the skin and between the vertebrae into the epidural space.
Fluoroscopy allows the doctor to monitor the needle on an X-ray screen in real-time, ensuring that the needle is moving to the desired location.
Some pain occurs during the procedure, but generally, patients usually feel more pressure than pain.
There are several types of ESIs:
- ESI for cervical disc herniation by injection: The needle entry site is located on the side of the neck to reach the nerve site, just above the nerve root opening and outside the epidural space. A dye that shows up on the fluoroscopy is injected to confirm where the medication is flowing.
- Lumbar ESI (lower back): The needle entry site is slightly off the midline of the back to access the nerve canal. A contrast medium is also injected to confirm where the medication is flowing.
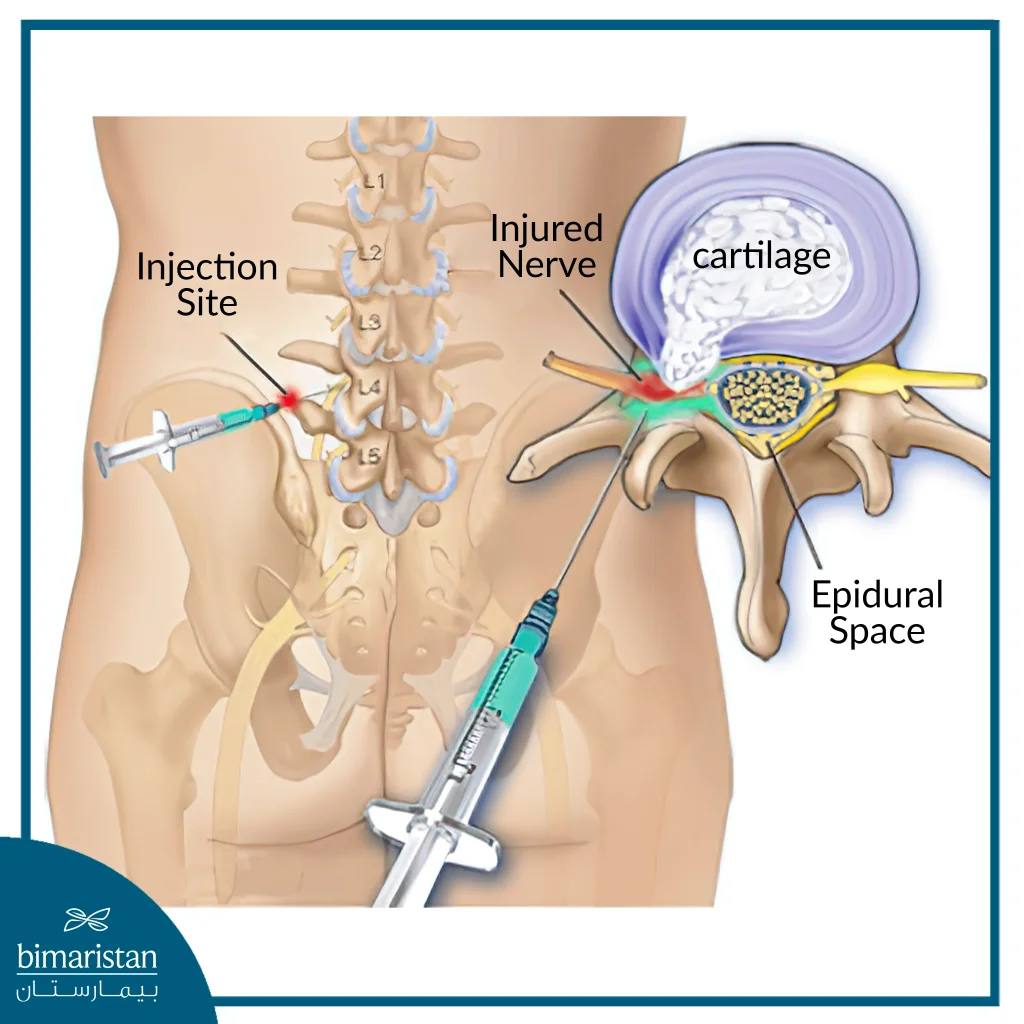
- Caudal ESI (Sacral): The needle is placed in the sacral space above the sacrum to reach the lowest spinal nerves. Contrast dye is injected to confirm where the medication is going.
Step 3: Injecting the Medication
When the needle is correctly positioned, the anesthetic and corticosteroid medications are injected into the epidural space around the nerve roots.
The needle is then removed. Depending on the location of the pain, the procedure can be repeated on both the left and right sides.
One or more levels of the spine can be injected.
Sedation and/or anesthesia can be used.
If necessary, a relaxing medication can be given through an intravenous (IV) line in the patient’s arm, but the patient is usually awake during this procedure.
The treatment area in the lower back is numbed with a very thin local anesthetic injection before the epidural is administered, so the epidural injection procedure is usually painless.
The epidural steroid injection procedure can take about 15-45 minutes to complete.
As the medication enters the epidural space, a slight tingling or burning sensation or a feeling of pressure may be felt. When the injection is complete, irritation and discomfort usually go away within a few minutes.
Patients usually go home after a few hours.
Specific precautions are followed after the injection for the next few days.
Possible benefits of Epidural Steroid Injections
Most doctors agree that epidural injections can be helpful during an acute episode of back and/or leg pain.
The main drawbacks of the injections are that they are not always effective, and when they are effective, the pain relief tends to be temporary, ranging from a week to a year.
If the initial injection is effective, up to 3 injections can be given in a year.
When an epidural steroid injection is given in the lumbar region, the steroid injection may have the following benefits:
- Reducing nerve pain and inflammation. Steroids reduce the production of inflammatory chemicals and decrease the sensitivity of nerve fibers to pain, resulting in fewer pain signals.
- Reducing the need for oral medication. The pain relief from these injections may help reduce or eliminate the need for oral medications, some of which can have side effects when taken long-term.
- Continuation or re-engagement with physical therapy. This injection may provide sufficient pain relief to allow the patient to progress through a rehabilitation program.
- Delaying surgery. The pain relief provided by lumbar epidural steroid injections may help delay surgery and, if physical therapy is effective, may eliminate the need for surgery.
A variety of techniques can be used to treat herniated discs with epidural steroid injection depending on the underlying condition, the patient’s needs, and the physician’s preference and experience.
Efficacy of the injections
Available research indicates generally positive results, with 70% to 90% of patients experiencing pain relief from these injections, lasting for a week to a year.
If a good initial response is seen, a second injection may be considered when the improvement from the first injection begins to taper off. Typically, up to 3 injections may be given over 12 months.
While several studies have documented the short-term benefits of epidural steroid injections, the data on long-term effectiveness are less convincing.
Controversy continues regarding their effectiveness in reducing pain and improving function. Studies supporting and opposing it are provided below.
In addition, there are several limitations to the research that has been conducted, such as:
- Many studies do not include fluoroscopy or X-rays to verify proper medication placement despite the fact that fluoroscopy guidelines are routinely used today.
- Other studies do not classify patients according to diagnosis and tend to “cluster” different types of pain sources together.
These methodological shortcomings tend to limit the usefulness of the research. Further studies are needed to determine the role of epidural steroid injections in low back pain and sciatica.
Who injects herniated discs between the fourth and fifth vertebrae?
Neurosurgeons, anesthesiologists, and pain specialists are among the doctors who perform this type of injection, which is usually performed in a surgery center, hospital, or doctor’s office.
Possible risks and contraindications of epidural injections for herniated discs between the fourth and fifth vertebrae.
Epidural steroid injections are relatively safe and minimally invasive. Temporary side effects may occur in some cases and include (but are not limited to):
- Post-injection pain
- Nausea
- Headache
- Dizziness
- Fainting (vasovagal syncope)
- Flushing of the face
These side effects usually resolve within a few minutes to hours. Serious complications, although rare, may include spinal cord damage, dural puncture, and/or stroke.
Possible complications after Epidural Steroid Injections
While serious complications after epidural steroid injections are rare, they are detailed.
- Infection
Infection may occur generally within the body (systemic infection), affect the brain and/or spinal cord, or occur locally at the injection site. Examples include:
Epidural abscess: accumulation of pus in the epidural space.
Meningitis: inflammation of the membranes of the brain and spinal cord.
Osteomyelitis or discitis: inflammation of the vertebral bones or disc between the vertebrae.
Soft tissue abscess: accumulation of pus within the soft tissues at the injection site.
Microbes from the patient’s skin are thought to be a common cause of infection.
- Bleeding after injection disc treatment
Arterial injury can cause local bleeding and blood to collect within the soft tissues, epidural space, or spinal cord membranes. A hematoma or blood clot may form within the artery, blocking the blood supply to vital tissues, such as the brain and/or spinal cord.
- Dural puncture
Inadvertently inserting a needle into the outer membrane of the spinal cord (dura mater) can result in a puncture of the dura. This condition is also called cerebrospinal fluid leak and causes cerebrospinal fluid to leak, reducing the pressure of cerebrospinal fluid in the brain, causing headaches and head pain that go away with pain medication.
- Nerve damage
Damage to nearby nerves can cause abnormal sensation, loss of sensation, or seizures. If the nerves in the cauda equina at the base of the spinal cord are damaged, it can lead to a medical emergency called cauda equina syndrome.
This syndrome causes loss of bowel and bladder control and must be treated immediately to prevent paralysis of the lower body.
- Cardiovascular (heart) complications
Sometimes, low blood pressure and a slow heart rate can occur after an epidural steroid injection.
- Risks associated with local anesthesia
In injections containing local anesthesia, if the solution enters a blood vessel, it can cause toxicity to the central nervous system and/or the cardiovascular system.
- Risks Associated with Particulate Steroids in Injectable Disc Treatment
The larger particles in the particulate steroids may clump together and block blood vessels, resulting in decreased blood flow to the spinal cord.
The risks and complications are usually higher with epidural steroid injections given above the L3 level, and the most common risk is the injection of steroids into blood vessels, which is more likely to occur in people over the age of 50.
In rare cases, an allergic reaction to the steroids, local anesthesia, or contrast agent may occur.
Fewer risks at spinal levels L4 and below.
In general, epidural injections given at spinal levels L4 and below carry a lower risk of complications than at higher levels. The injections are usually performed under fluoroscopy (x-ray guidance) using contrast dye. Fluoroscopy helps guide the needle to the exact location and helps prevent nerve and/or artery damage.
What happens after lumbar disc herniation treatment with injections?
Most patients can walk around immediately after the procedure.
You can usually leave the office after being monitored for a short period.
Rarely, temporary leg weakness or numbness occurs, so someone should drive you home.
Patients usually resume full activity the next day. Pain around the injection site can be relieved with ice and a mild painkiller (Tylenol).
You may want to record your pain levels in a notebook over the next two weeks. You may notice a slight increase in pain, numbness, or weakness as the numbing medication wears off before the corticosteroid takes effect.
Patients should schedule a follow-up appointment with their referring physician or treating physician after the procedure to document the effectiveness of the procedure and address any concerns the patient may have about future treatments and expectations.
When to call the doctor?
The following serious symptoms of epidural steroid injection that require immediate medical attention include:
- A severe headache when sitting or standing that feels better after lying down, which may indicate a dural puncture.
- A fever of 101 degrees or higher may indicate an infection.
- Decreased or complete loss of bowel or bladder control while the patient is still sedated or after local anesthesia and temporary numbness wears off, which may indicate a medical emergency, such as cauda equina syndrome.
- Numbness and/or weakness in the leg(s), which may indicate a nerve injury.
It is important to contact your doctor immediately if these symptoms occur. In addition, any discomfort or abnormal sensation should be discussed with your doctor.
Studies on Epidural Steroid Injection
One study suggests that this technique has converted about 40% of patients from surgical indications such as endoscopic discectomy to non-surgical treatment.
The price of an Epidural Steroid Injection in Turkey
The cost of disc injection treatment in Turkey is approximately $1,500. Contact Bimaristan Medical Center for medical advice and to book an appointment as soon as possible.
Sources:
- Johns Hopkins Medicine
- Spine-health
- Bupa UK