Scoliosis of the spine is a spinal deformity that causes the spine to bend in an S or C shape, with or without vertebral rotation.
Scoliosis is a relatively common spinal condition, especially in childhood, affecting 2-3% of the population, or approximately six to nine million people in the United States. Both symptoms and treatment vary depending on the age at which the condition manifests.
Scoliosis of the spine may not manifest severe symptoms that require urgent treatment, but the deformity of the spine is the main reason for scoliosis surgery. This article discusses the key symptoms of scoliosis, its signs, and the latest surgical techniques used for its treatment in Turkey.
What is Scoliosis of the spine?
Scoliosis of the spine, or spinal curvature, is a skeletal disorder in which the spine deviates to one side, often affecting the thoracic or lumbar vertebrae (or both).
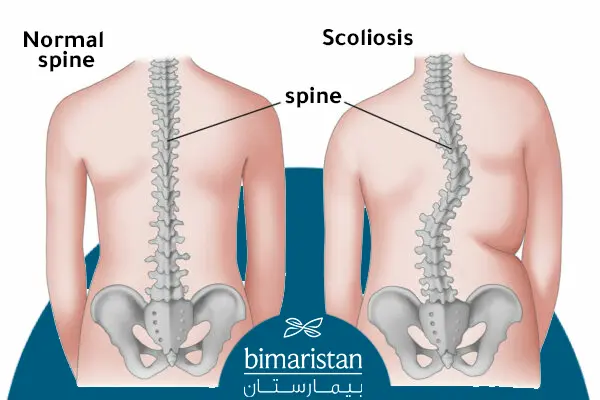
Scoliosis of the spine affects all age groups, including infants, but it usually begins to appear in children aged 10 to 15. Both males and females can develop mild scoliosis without significant gender differences, although the progression and worsening of scoliosis tend to be eight times greater in females.
Each year, people with scoliosis make more than 600,000 visits to private clinics, with around 30,000 children receiving braces and 38,000 patients undergoing spinal fusion surgery to treat scoliosis.
While mild scoliosis of the spine is considered normal, if the curvature exceeds 10-15 degrees on a simple X-ray, it becomes a medical problem that requires treatment.
Scoliosis of the spine causes
About 80% of cases of spinal curvature or twisting are of unknown origin, but there are many expected causes for scoliosis, with the most important being:
- Genetics: Some theories support a link between genetic factors and scoliosis.
- Physical deformities include deformities in the muscles around the spine and uneven growth between different parts of the spine, which may be a potential cause.
- Congenital deformities are developmental deformities of the vertebrae (fused or missing vertebrae), usually appearing around the age of two.
- Tumors or small deformities in the spine: These may be a significant cause of scoliosis in young children.
- Spinal surgery: Surgery to remove a benign tumor may increase the risk of scoliosis in the future.
- Studies have shown that females are more likely to be affected than males because of the presence of a region on the X chromosome linked to scoliosis of the spine (XX chromosome formula for females, while XY for males).
Scoliosis of the spine symptoms
The majority of scoliosis of the spine cases are mild without symptoms, but in some severe cases, the symptoms may include:
- Pain in the area of curvature, especially in the lower back.
- Neurological symptoms such as numbness and tingling in the legs.
- Chest symptoms such as shortness of breath (in thoracic scoliosis).
In one study, about 23% of scoliosis patients with an unknown cause experienced back pain at the time of initial diagnosis. Of these patients, 10% had an underlying condition associated with scoliosis, such as spinal stenosis, tethered cord, herniated disc, or spinal tumor. If a patient with unknown-cause scoliosis has mild back pain, a comprehensive assessment for another cause of pain is recommended.
Due to changes in the shape and size of the chest, idiopathic scoliosis may affect lung function. Recent reports have shown a decrease in lung function in patients with mild to moderate scoliosis of the spine.
Scoliosis of the spine signs
A patient with scoliosis or one of their family members may notice one or more signs indicating spinal deviation. These signs include:
- One shoulder blade is more prominent than the other.
- One shoulder is higher than the other.
- The head is not centrally positioned above the body.
- Clothing does not hang evenly on both sides.
- The chest leans to one side.
- The waist is asymmetrical.
- Asymmetry in the front of the chest.
Diagnosing scoliosis
Initially, the presence of scoliosis in the patient’s family is inquired about, as most cases of scoliosis have a genetic origin. The diagnosis of scoliosis is primarily based on listening to the patient’s complaints and conducting a physical examination. The body is generally observed initially to detect spinal deviation.
Some tests, such as the Adams test, are conducted if this fails to reveal scoliosis. The Adams test asks the patient to stand and bend forward (as in kneeling). Finally, the diagnosis is confirmed through a simple X-ray of the spine, which shows the presence of deviation. The X-ray allows us to measure the Cobb angle, expressing the size of the curvature in the spine, with a curvature of at least 10 degrees indicating scoliosis. In general, scoliosis of the spine is considered significant if the curvature is greater than 25-30 degrees.
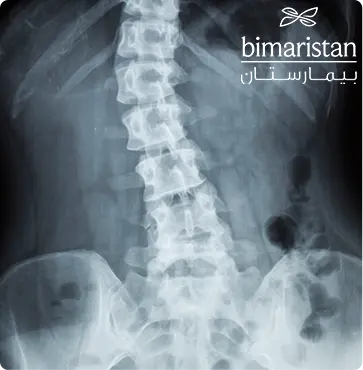
Scoliosis in Children
Idiopathic scoliosis accounts for the majority of cases that emerge during adolescence. Depending on the severity of scoliosis and the child’s age, correction can be achieved through careful monitoring, bracing, or surgery.
In children with congenital scoliosis of the spine, there is a documented increase in its association with other congenital deformities commonly linked to the spinal cord (20%), genitourinary system (20-33%), and the heart (10-15%). Therefore, evaluating the nervous, genitourinary, and cardiovascular systems is essential when diagnosing congenital scoliosis.
Scoliosis in Adults
Scoliosis of the spine that occurs or is diagnosed during the adolescent stage is distinct from scoliosis in adulthood. The underlying causes and treatment goals differ in patients who have already reached skeletal maturity.
In a 20-year study, about 40% of adult scoliosis patients experienced a significant increase in curvature, while 10% showed considerable progression. The remaining 30% experienced moderately severe deterioration (usually less than one degree per year).
Adult degenerative scoliosis of the spine occurs in the lumbar spine (lower back) and is more common in individuals over the age of 65. Typically, this scoliosis is accompanied by spinal stenosis or narrowing of the spinal canal, leading to pressure on the spinal nerves.
Back pain associated with degenerative scoliosis usually begins gradually and is activity-related. The curvature of the spine in this type of scoliosis is relatively mild, so surgery is usually recommended only when conservative methods fail to alleviate the pain associated with degenerative scoliosis.
Curvature of the Spine Risk
The risk of spinal deviations depends on various factors that may affect the patient’s daily life. The most important factors include:
- The degree of scoliosis or curvature in the spine, with a curvature of 45 degrees, is considered poor in thoracic scoliosis and 35 degrees in lumbar scoliosis.
- The location of scoliosis and its impact on adjacent organs.
- The scoliosis patient’s age and the spine’s remaining growth potential predict future warnings. Generally, scoliosis in adults is less risky than in children.
Non-Surgical Treatment for Scoliosis of the Spine
If the degree of scoliosis is less than 25 degrees in children, monitoring through regular X-rays may be sufficient. The doctor may recommend bracing or specific exercises for more severe curvatures, especially in older patients.
Bracing for scoliosis of the spine
In cases where scoliosis measures between 20-25 degrees in adults and 40-45 degrees in children, some doctors may recommend using belts and braces that can be worn for several hours a day to prevent the progression of scoliosis with the child’s growth.
Prominent examples of these braces include the Boston brace, the Providence brace (worn only at night), the Charleston brace, and the flexible spinal brace. There is evidence that scoliosis patients who wear the appropriate brace for at least 13 hours a day are 56% less likely to undergo spinal surgery in the future.

physical therapy for scoliosis of the spine
Some studies suggest that exercises such as yoga may help automatically correct posture by strengthening the muscles around the spine and aligning the spine. However, there is currently no conclusive evidence regarding the effectiveness of these exercises in treating scoliosis.
Scoliosis operation in Turkey
For Scoliosis treatment for adults, we perform spinal fusion surgery in Turkey, also known as scoliosis surgery, when bracing treatment fails and the patient’s condition deteriorates (curvature of the thoracic spine greater than 45-50 degrees or lumbar spine greater than 35-40 degrees).
The most common and widely used surgical treatment for scoliosis is spinal fusion (arthrodesis). This involves fusing the vertebrae in the spine together, similar to many other skeletal conditions such as lumbar spondylolisthesis. During the procedure, the surgeon performs osteotomies (cuts) to expose the vertebrae that make up the curvature.
The surgeon removes the facet joints and bony joints along the vertebrae, allowing the spine to straighten. Finally, bone grafts are placed across the exposed surface of each vertebra, and the osteotomies are bent back into their original position, covering the bone grafts.
Preoperative Considerations for Scoliosis of the spine
Before scoliosis surgery, the patient undergoes a comprehensive physical examination to determine leg length and muscle strength and detect any other deformities. Lung function is also assessed, and examination of the operation area is crucial to identify potential infection risks from burns or wounds.
Patients are trained in deep breathing and effective coughing to avoid lung congestion after surgery. Additionally, they are taught a specific bed-turning technique called the logrolling technique.
Bone grafts used in scoliosis surgery are often harvested from the patient’s own body (such as the thigh) or may be obtained from a bone bank to alleviate postoperative pain, which is higher when grafts are taken from the patient’s body.
Approaches to Spinal Intervention in Scoliosis of the spine Surgery
There are two approaches to accessing the spinal column for scoliosis of the spine surgery: the posterior approach (through opening the patient’s back) and the anterior approach (through opening the chest or thoracoscopic approach). Additionally, a combined approach may be used in some cases, especially in pediatric patients.
The posterior approach is the gold standard for treating lumbar scoliosis (lower spine curvature). This method requires several devices and generally takes less time than the anterior approach. However, postoperative back pain and the amount of bleeding are usually greater.
In the anterior approach, an incision is made in the chest, the lungs are deflated, and ribs may be removed (commonly used for bone grafts). This approach allows the surgeon to maintain a fusion of the lower vertebrae. This method is often performed using modern techniques known as Video-Assisted Thoracoscopic Surgery (VATS).
Minimally Invasive Techniques in Scoliosis Surgery in Turkey
Small incisions, called portals, are made on the side of the chest. Surgeons use endoscopes, cameras, and video monitoring devices to visualize the spine, reducing bleeding and shortening recovery time to around two days after surgery. In contrast, open surgery (opening the chest) requires a larger single incision and a longer recovery period.
These modern devices make spinal surgery less invasive for the patient while providing equal or better results. There is minimal impact on lung function using the VATS technique, as some studies have shown. After surgery, small incisions are hidden under the patient’s arm, making scars much smaller from a cosmetic perspective than standard open procedures.
Spinal fusion can sometimes be performed through smaller incisions using this technique. Advanced fluoroscopy (X-ray imaging during surgery) and camera-assisted procedures have reduced the size of incisions and the placement of devices, reducing tissue trauma. It is important to note that not all cases can be treated this way, and several factors contribute to the surgical approach used.
Different Procedures in Scoliosis Surgery
These procedures aim to immobilize the spine for fusion, achieving spinal balance after fusion. Some of these procedures include:
- Harrington Procedure: This involves using a steel rod that extends from below the curvature to above it. Hooks are attached to screws inserted into the bone lift and lock the rod in place to support the spine securely. However, it is challenging to apply in adult scoliosis cases, and the postoperative bed rest period is typically 3-6 months.
- Cotrel-Dubousset Procedure: This procedure involves connecting two parallel rods for better stability of the fused vertebrae. It has a high success rate (about 95%), with patients typically returning home after about 5 days, making it more commonly used for adult scoliosis treatment. The Cotrel-Dubousset procedure helps correct both curvature and rotation of the spine, with a lower incidence of flat back syndrome compared to the Harrington procedure. However, the duration of the procedure and the amount of bleeding are generally greater than in the Harrington procedure.
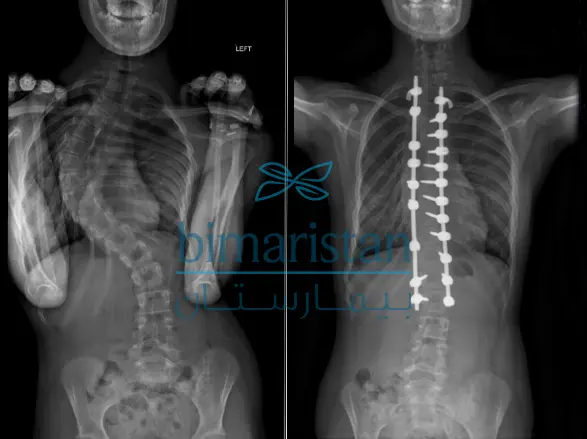
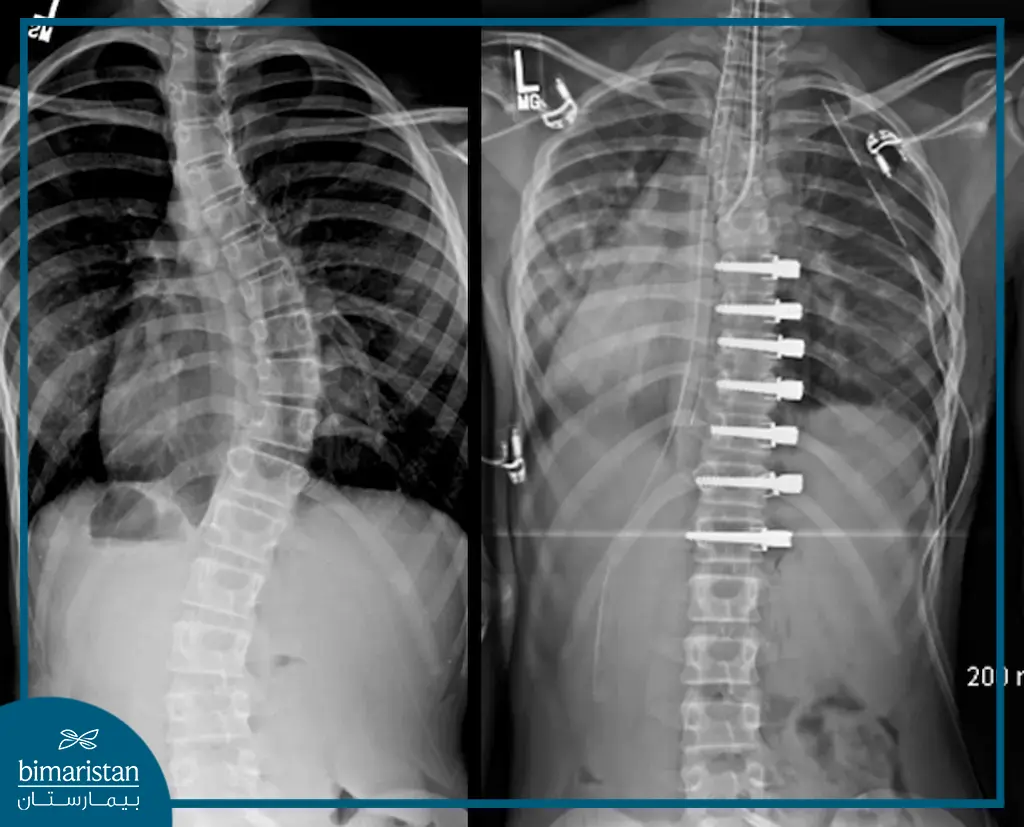
- Wires under the Sublaminar: Frequently used with a single rod for correcting neuromuscular scoliosis or scoliosis resulting from cerebral palsy or spinal cord injury.
These modern devices have made the correction of spinal deformities less invasive, offering improved results for scoliosis of the spine surgery. It is essential to consider that not all cases can be treated using these techniques, and various factors influence the surgical approach chosen.
Tips for Scoliosis Patients After Surgery
There are several tips and practices that you should adhere to after scoliosis of the spine surgery to achieve a lifestyle free from complications and risks. These tips include:
- Avoid lifting heavy objects, as it increases pressure on your spine, leading to a decline in your health.
- Avoid sleeping on your stomach, as this position flattens the thoracic spine, worsening scoliosis.
- Change your body position frequently, as prolonged sitting or standing increases pressure on the spine.
- Regularly engage in physical exercises to strengthen the spinal muscles, enhancing stability.
Scoliosis of the spine Surgery Complications
Like most surgeries, scoliosis surgery is not without complications, although their incidence is relatively low (1-3%). Some of the significant complications include:
- Bleeding, especially in open surgery.
- Postoperative pain is typically managed with morphine immediately after the surgery through an intravenous pump, followed by oral pain relievers like acetaminophen in the days after the operation.
- Infection, as the metallic materials used in stabilizing and correcting scoliosis increases the risk of infection.
- Nerve injury, with a low incidence that increases with age.
- Pseudoarthrosis, where a false joint develops at the site of spinal fusion.
- Disc degeneration and lower back pain.
- Hook displacement or fractures in the fused vertebrae.
Scoliosis of the spine Surgery in Turkey Success Rate
The success rate of scoliosis of the spine surgery depends on various factors that significantly impact the outcome, including the surgeon’s experience, the surgical technique used, and the advancement of the medical center where the surgery takes place.
The success rate of scoliosis surgery, or spinal fusion surgery, is around 70%, especially for those performed on children under 11 years old, where the likelihood of complications is very low.
Scoliosis Surgery Cost in Turkey
Scoliosis surgery costs depend on several factors, including the surgical technique and the patient’s health condition. Additionally, the quality of devices available in specialized medical centers may affect the price. Generally, scoliosis surgery costs in Turkey between $10,000 and $15,000.
Although scoliosis of the spine may negatively impact your health, lifestyle, and appearance, it is not an inevitable fate that you must live with. Many scoliosis patients have been successfully treated in Turkey and are regaining their natural appearance.
With the help of trained specialists and non-invasive or minimally invasive methods, we can assist you in managing your condition. Finding comfort may be much easier than you think. If you are affected by scoliosis or concerned about the possibility, seek treatment today.
Sources:


