Tracheal diseases may cause airway obstruction, leading to respiratory symptoms such as chest tightness and difficulty breathing. learn about ways to diagnose and treat them in Turkey.
What are the types of tracheal diseases?
There are two main types of tracheal disorders:
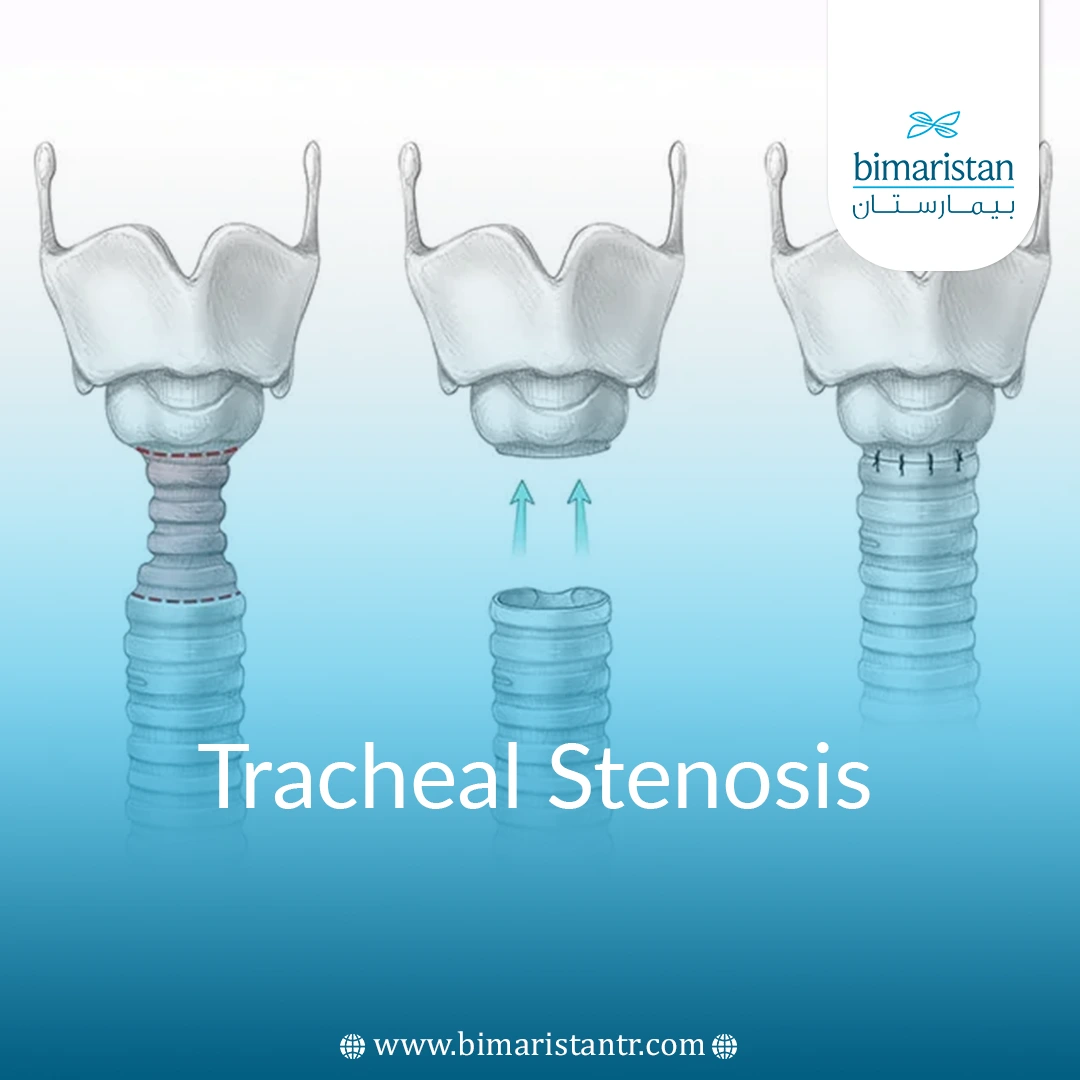
- Tracheal stenosis is a narrowing of the trachea that prevents air from reaching the lungs adequately. The effects of tracheal stenosis can range in severity from mild to more severe. In severe cases, the patient may have to rely on a breathing tube.
- Tracheomalacia is a condition characterized by the absence of cartilage from the walls of the trachea, causing weakness in the trachea, which must be rigid to perform its function of normal breathing. Children can be born with tracheomalacia, but adults can also develop it later in life.
While tracheal tumors are rare, they can cause a narrowing of the trachea that prevents air from fully reaching the lungs and can also cause a bloody cough.
Types of tumors include
Benign tumors
Pleomorphic adenoma, squamous cell carcinoma, chondroma, granulosa cell tumor, glomus tumor, neurofibroma
Malignant tumors
Adenoid cystic carcinoma, squamous cell carcinoma, epithelial carcinoma, mucosal carcinoma, and lung carcinoma.
Another tracheal disorder is tracheal fistula, which is an abnormal connection (fistula) between the esophagus and the trachea.
What are the causes of tracheal disorders?
The most common cause of tracheal diseases, such as stenosis, is intubation, when a breathing tube is inserted into the windpipe for surgery or other medical procedures.
Other causes of tracheal diseases may include the following:
- External damage to the throat or chest
- Thermal or caustic injuries
- Chronic inflammatory disease
- Infections, including tuberculosis
- Tumors that compress the windpipe
- Radiation therapy
- Conditions in young women of unknown cause
- Pressure from other tissues in the chest, such as blood vessels
- Autoimmune disorders
Tracheomalacia:
Tracheomalacia, a tracheal disease, can have many causes, the most common of which are:
- Damage caused by surgery or procedures in the windpipe or esophagus
- Damage caused by a long-term breathing tube or tracheostomy
- Chronic infections, such as bronchitis
- Cartilage inflammation (tracheal cartilage inflammation)
- Emphysema
- Gastroesophageal reflux disease
- Inhalation of irritants
What are the symptoms of tracheal disorders?
Tracheal stenosis:
Many patients do not experience any of the symptoms of tracheal diseases, such as stenosis. However, a patient may have one or more of the following:
- Hyacinth
- Squeak (high-pitched musical breathing sound)
- Shortness of breath
- Difficulty breathing
- Coughing
- Hoarseness
- Recurrent upper respiratory infections, such as pneumonia
- Treatment-resistant asthma
- A bluish color on the skin
- A bluish color in the mucous membrane of the mouth or nose
- Bloody cough
Tracheomalacia:
- Shortness of breath.
- The cough is chronic.
- Hoarseness.
- Recurrent respiratory infections.
- Abnormal breathing sounds that improve when you change position or fall asleep.
- High-pitched, noisy breathing, sometimes with a rattling sound.
- Difficulty swallowing food.
How are tracheal diseases diagnosed?
Tracheal stenosis
In addition to a thorough physical examination, the following procedures can be done to determine if your symptoms are caused by tracheal stenosis:
- Pulmonary function tests, or PFTs, assess the function and strength of the lungs. In the most common of these tests, the patient blows air forcefully into a tube, and a device called a spirometer measures how much air the patient can hold in the lungs and how quickly they can exhale. Compared to normal values, a blocked airway can be identified.
- A CT scan that uses a combination of X-rays and computer technology to produce horizontal or axial images of any part of the body, including bones, muscles, fat, and organs. A 3D CT scan of the chest provides a closer look at the area of stenosis during both inhalation and exhalation, outlining the contours that will be used for the surgery.
- Chest X-rays produce images of internal tissues, bones, and organs.
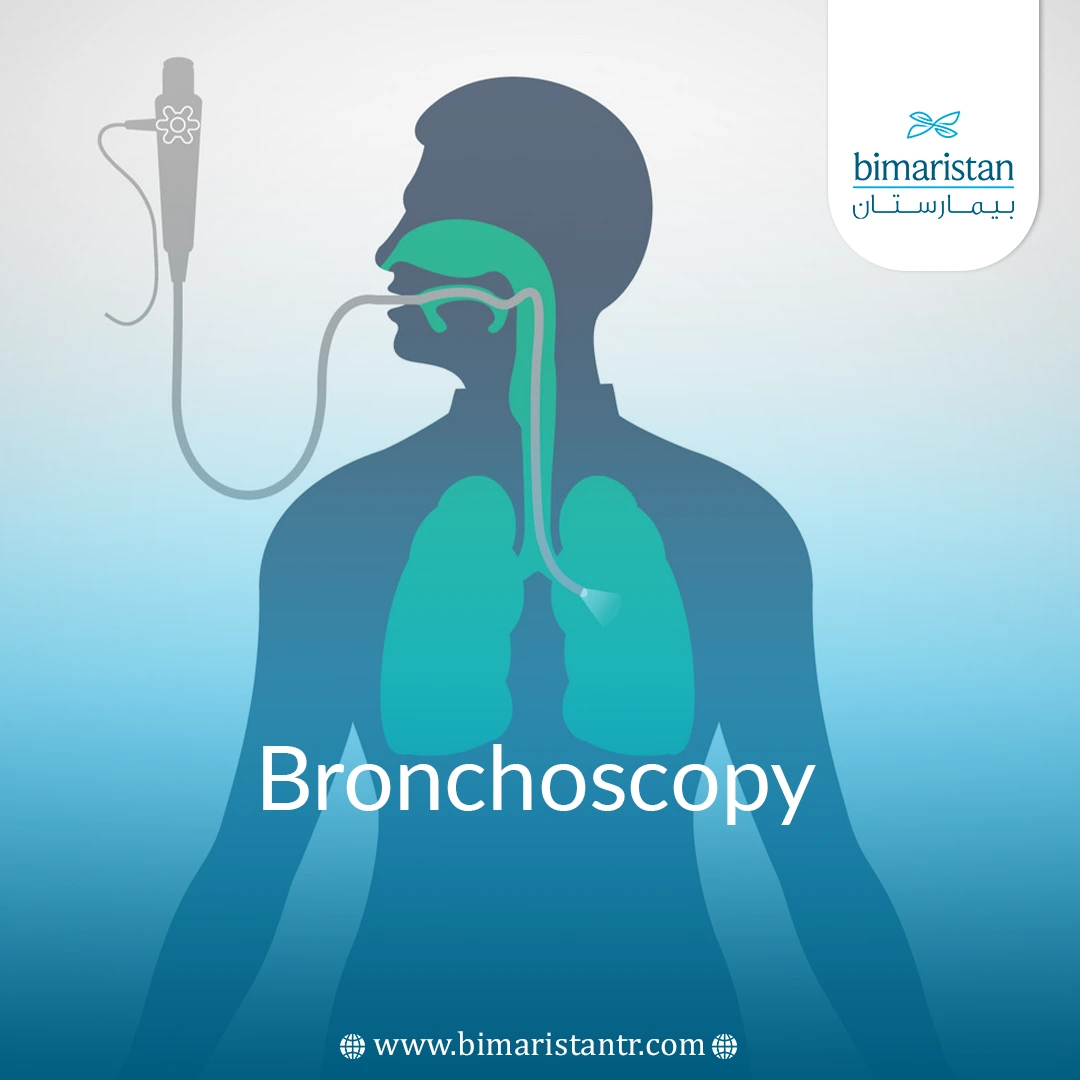
- Bronchoscopy – A procedure in which a lighted tube is inserted into the windpipe and allows the doctor to examine the trachea and bronchi (the airways leading to the lungs). The procedure allows the doctor to make an accurate diagnosis and measure the length of the non-medical airway segment
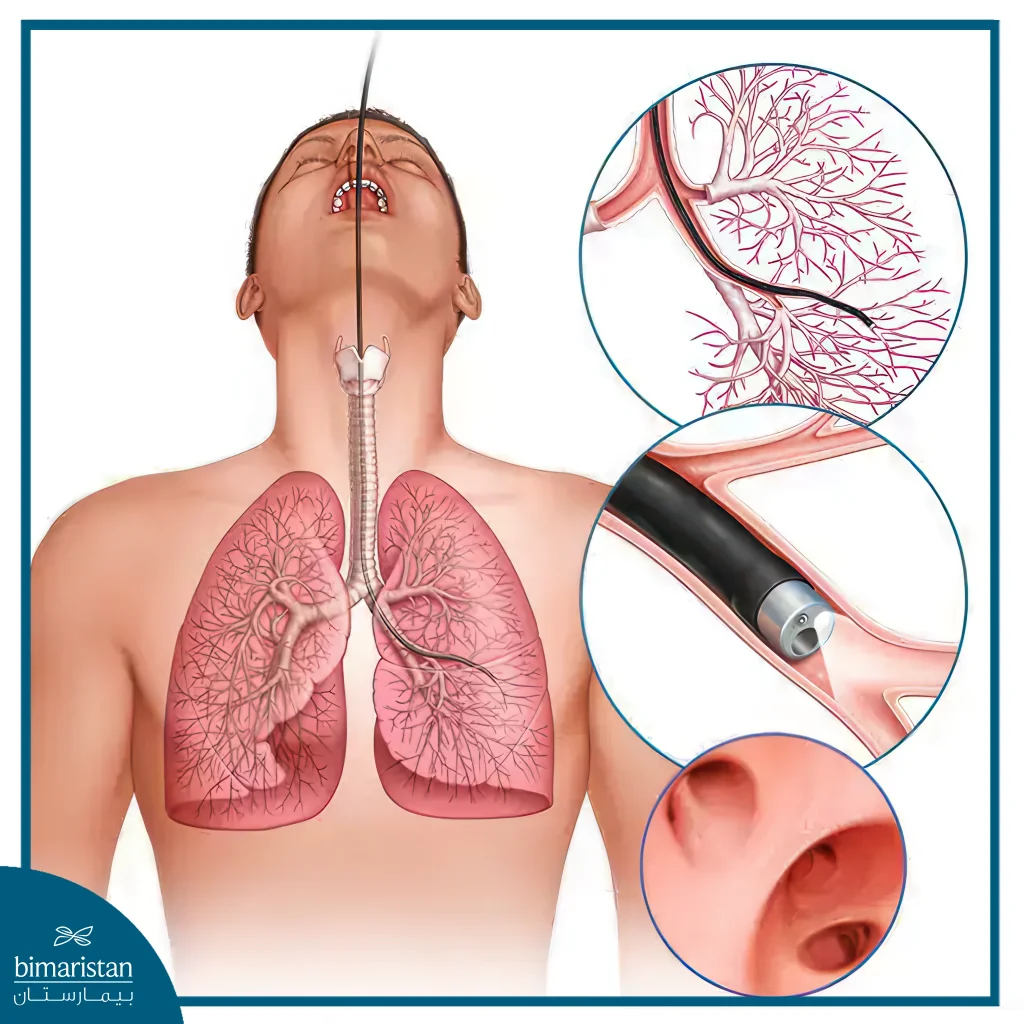
Tracheomalacia
After taking your medical history and performing a thorough physical examination, the following procedures may be performed to confirm the diagnosis of tracheal diseases such as tracheal stenosis or tracheomalacia:
- Functional exercise capacity is measured by a walking test that measures the distance an individual can walk over 6 minutes on a hard, flat surface.
- Measure cardiopulmonary function during exercise on a treadmill or stationary cycling.
- Perform a bronchoscopy to examine the inside of the trachea and bronchi. This allows for an accurate diagnosis and measurement of the affected area to determine the best possible treatment options.
- Use of CT scans.
- Chest X-ray.
- Laryngoscopy enables the doctor to examine the back of the throat, larynx, and vocal cords using a scope.
- Magnetic resonance imaging (MRI) is a non-invasive way to evaluate the trachea.
- A pulmonary function test measures how well your lungs are working.
- Checking pulmonary ventilation/perfusion using two nuclear scanning tests: injecting radioactive albumin into your veins and inhaling the radioactive gas through a mask to allow the scanner to measure blood circulation (perfusion) and breathing (ventilation).
What are the treatment options for tracheal disorders?
Tracheal stenosis
There are several surgical options for treating tracheal diseases, such as tracheal stenosis. Your thoracic surgeon will recommend the best option for you based on the cause, location, and severity of the stenosis. Possible treatments and procedures are:
- Argon plasma coagulation (APC) is a form of non-contact electrocoagulation using a flexible bronchoscopic device that allows for rapid coagulation with minimal mechanical trauma to the tissue. This procedure is used for patients who are unable to undergo tracheal reconstruction for medical or personal reasons.
- Bronchial artery embolization (BAE), a procedure that involves examining the bronchial arteries by X-ray using a special dye to determine the cause of the hemoptysis so that the bleeding can be stopped.
- Bronchoscopic tracheal dilation using a balloon, a tracheal dilator, or an electric tracheal dilation cuff. This procedure provides immediate relief to the patient and helps the thoracic surgeon determine the extent of the stenosis.
- Laser bronchoscopy to remove scar tissue and give excellent short-term relief.
- Tracheobronchial airway stenting. This is a nonsurgical procedure that uses a bronchoscope to place a stent to keep the airway open.
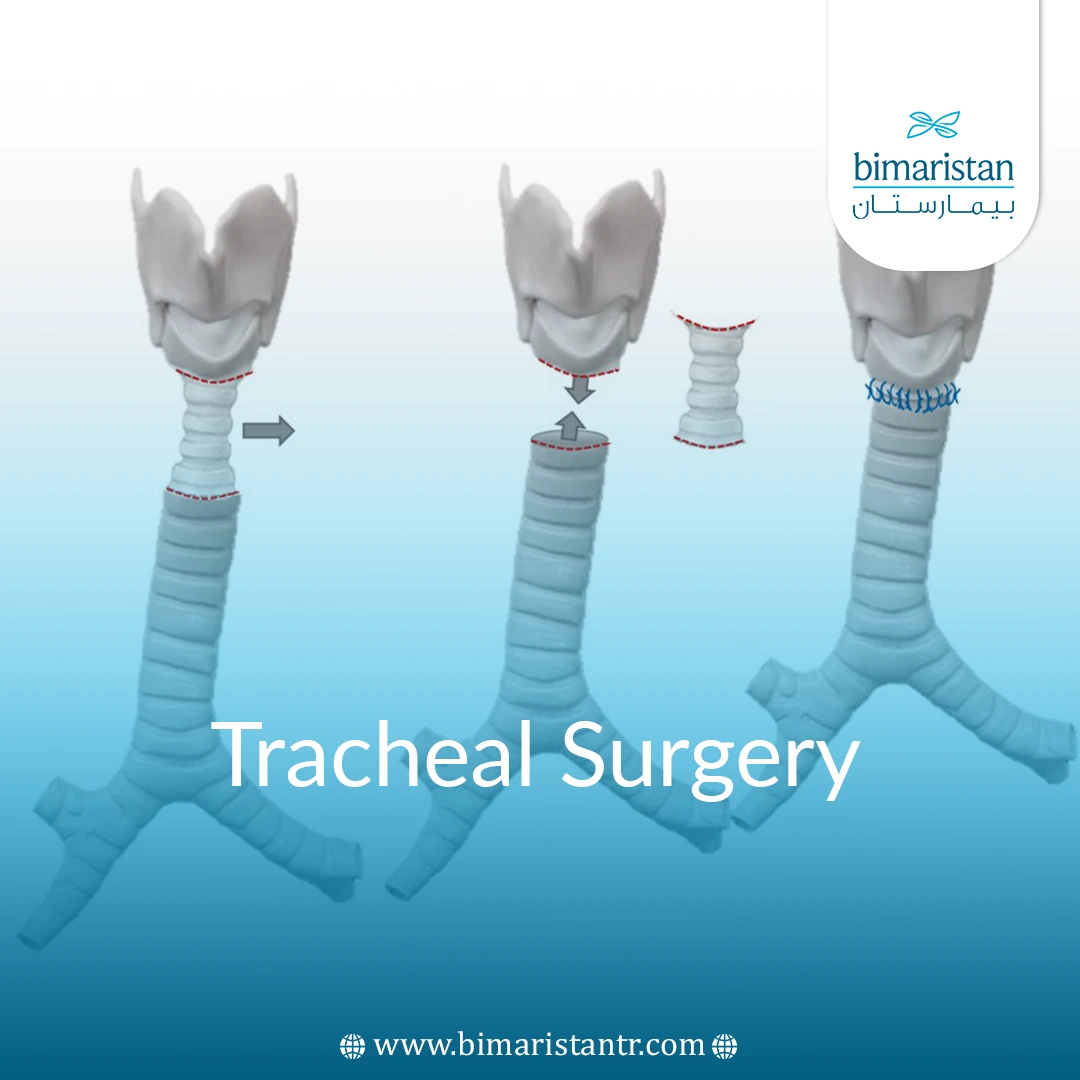
- Tracheal resection and reconstruction, where the scarred and narrowed part of the trachea is removed and the segments are reattached to each other. This treatment has excellent long-term results and is the first procedure indicated for some tumors and stenosis.
- Tracheoplasty, a procedure performed in a small number of hospitals, involves sewing an opening to the outside of the patient’s trachea through a series of knots, which opens up collapsed tissue in the tracheal wall to create an opening for air to pass through. The goal is to create scar tissue in the area that permanently strengthens the tissue.
Tracheomalacia
Often, tracheal diseases such as tracheomalacia can get better without treatment. However, you should be closely monitored if you have frequent respiratory infections. Treatments may include:
- Use a continuous positive airway pressure (CPAP) device to keep your airway open.
- Chest therapy, including deep breathing exercises and chest tapping, to break up mucus.
- Speech and language therapy to modify breathing patterns and swallowing issues.
- Use of a tracheobronchial airway stent.
Sources: