Liver transplant in Turkey is the definitive surgical treatment for patients with end-stage liver disease and patients with acute liver failure that improves liver function and survival after transplantation.
Liver transplantation is a final solution to many liver problems, as this operation saves the lives of patients with acute liver failure, and the harms of liver transplantation can be avoided with the advancement of medicine in Turkey.
What is the success rate of liver transplants? How many hours does the liver donation process take? What are the contraindications and conditions for liver transplantation? Is liver donation dangerous? Find out with us the answers to these questions in the following article.
Introduction of the Liver Transplant Process
The first liver transplantion was performed in 1963 in the United States by surgeon Thomas Starzl. Today, this operation is the most effective treatment for end-stage liver failure and acute liver failure. Liver transplantation has been performed on more than 80,000 patients suffering from Chronic liver failure in the world.
Over the past three decades, liver transplants have become a life-saving option for patients suffering from end-stage liver disease, malignant liver tumors, metabolic diseases associated with liver damage, and acute liver failure. Transplantation operations aim to prolong the recipient’s life and improve their quality of life.
Survival rates after liver transplant have increased significantly recently, with the survival rate reaching 96% for one year and 71% for ten years after transplantation. In addition to the many developments in surgical techniques, recipient selection and donor management, and preservation of organs prepared for transplantation, Intraoperative anesthetic procedures, advances in postoperative care and immunosuppressive therapies increase the success of long-term survival after liver transplantation.
Conditions for liver transplant surgery
There are three basic principles for determining which patients should be referred and likely to undergo liver transplantation:
- The recipient must have acute or chronic liver disease that cannot be cured and is expected to be fatal without liver transplantation.
- The patient must be in a condition that allows him to survive during and around the surgical procedure.
- The patient should be expected to have a significant survival and quality of life benefit after liver transplantation.
What are the reasons for a liver transplant?
- Acute liver failure: The most common cause of its occurrence is an overdose of acetaminophen medications (39%).
- Hepatic artery thrombosis within 14 days of liver transplantation.
- Cirrhosis: associated with decompensation (variceal bleeding, hepatic encephalopathy, or ascites) or associated with hepatopulmonary syndrome or pulmonary hypertension.
- Primary liver tumors: hilar cholangiocarcinoma and hepatocellular carcinoma.
- Congenital metabolic diseases: cystic fibrosis with lung and liver disease, primary hyperoxaluria type 1 with significant renal insufficiency, familial amyloid polyneuropathy.
Contraindications for liver transplantation
Definite contraindications for a liver transplant include:
- Active malignant cancers outside the liver
- Intrahepatic cholangiocarcinoma
- Hepatocellular carcinoma outside the Milan criteria or metastatic
- Severe cardiopulmonary disease
- Uncontrolled infections
- Alcohol or drug abuse
- acquired immunodeficiency syndrome (AIDS)
- Lack of social support or lack of permanent medical compliance
- Technical and/or anatomical contraindications to liver transplantation
Possible contraindications for a liver transplant include:
- Advanced age
- Portal vein thrombosis
- HIV infection
- Morbid obesity (BMI ≥ 40)
- Poor medical adherence or social support
- Active psychiatric comorbidities (3)
Evaluating the recipient’s condition before a liver transplant
Liver transplants involve physical and hemodynamic demands similar to major surgery, a potentially long recovery period, risks of prolonged immunosuppression, and increased psychosocial stress, so the pre-liver transplant recipient evaluation process is designed to screen the recipient to ensure that:
- Has sufficient physical health to survive the liver transplant and its surrounding period.
- He can adhere to medical recommendations to ensure optimal post-liver transplant care.
- Has a safe psychosocial support system after liver transplantation. (3)
Laboratory tests for liver transplantation in Turkey
The main purpose of these tests before liver transplantation is to confirm blood type (which must match a donor organ), evaluate the state of liver and kidney function, and rule out associated infections that may require treatment or that could affect post-liver transplant care or its results. This includes:
- Blood type: ABO and Rh
- Basic chemical tests
- Complete blood count
- Liver enzymes and clotting factors
- Calcium and vitamin D
- Urinalysis
- Detection of medications in urine
- Serological tests for hepatitis A, hepatitis B, hepatitis C, HIV, varicella zoster virus (VZV), cytomegalovirus (CMV), Epstein-Barr virus (EBV), and screening for tuberculosis (3)
Liver radiological examinations
Adequate CT imaging should be performed for surgical planning before liver transplantation. Three-phase CT or gadolinium-enhanced MRI is the most common and may help identify potential technical barriers to liver transplantation, including portal vein thrombosis, perihepatic varices, anatomical abnormalities in the Liver, and sequelae of previous abdominal surgeries. (3)
If CT or MRI cannot be obtained before liver transplantation, ultrasound with evaluation of Doppler flows may be sufficient. Liver radiography is particularly important for the accurate diagnosis of patients with intrahepatic malignancy in order to confirm their candidacy for liver transplantation. .(3)
Evaluate the recipient’s heart condition
Heart tests before a liver transplant are intended to screen for coronary artery disease, valvular disease, and/or cardiomyopathy, if present. Specific therapeutic interventions may be performed before or during a liver transplant as needed. If there is advanced heart disease, Cancellation of liver transplantation. (3)
Screening for malignant tumors
Age-appropriate cancer screening must be performed in all patients, given that the presence of a malignant tumor outside the liver is a definite contraindication for liver transplantation. The tests performed depend on the patient’s risk, and must be performed in accordance with the approved recommendations and guidelines in this regard. (3)
Bone density test
This test is performed before liver transplantation as the advanced liver disease leads to osteoporosis through relative inactivity, hypogonadism, low vitamin D levels, poor intestinal calcium absorption, and in some patients the direct effects of alcohol, steroids, or excess iron. (3)
Screening for infectious diseases
Hepatocellular dysfunction places liver transplant candidates at increased risk of developing a variety of infections including spontaneous bacterial peritonitis, aspiration pneumonia, urinary tract infections, and intravenous catheter-associated septicemia. Active infections should be treated appropriately before liver transplantation. (5)
Vaccination and immunity status
Liver transplant patients should be vaccinated against hepatitis A and B if serological tests do not show immunity, and tetanus, diphtheria, and pertussis vaccines must be current, in addition to vaccination against influenza and pneumococcus. (3)
Pulmonary hypertension
Pulmonary hypertension (MPAP ≤ 25 mmHg) occurs due to the presence of portal hypertension and is referred to as pulmonary hypertension (POPH). It is detected in 4-8% of liver transplant candidates. It is not considered hypertension. Mild pulmonary hypertension (MPAP < 35 mmHg) is a major concern but moderate (MPAP ≤ 35 mmHg) and severe (MPAP ≤ 45 mmHg) are predictive factors for increased mortality after liver transplantation. (5)
Smoking
Smoking is implicated in a number of adverse outcomes in liver transplant recipients, including death from cardiovascular causes and an increased incidence of hepatic artery thrombosis. Oropharyngeal, oral, and other tumors following liver transplantation are also associated with smoking and can lead to a high mortality rate that can be avoided in the long term. (5)
There are compelling reasons to ban all smoking methods in liver transplant candidates, and some organ transplant programs consider smoking cessation a requirement for liver transplantation, and this requires a series of negative nicotine tests to document smoking cessation. (5)
Steps of the liver transplant procedure
There are four steps to the liver transplantation process in Turkey:
Resection of the recipient’s liver and preparation for transplantation
Resection of the recipient’s liver is the first step in liver transplantation and can be a difficult procedure due to the close anatomical relationship between the liver and the hepatic tributary of the inferior vena cava in the setting of coagulopathy and portal hypertension. (6)
Liver resection can be performed using one of the following two techniques, but no study in the medical literature has proven the superiority of one over the other:
Traditional technique: In which the hepatic tributary of the original inferior vena cava is removed from the liver, the traditional technique requires complete closure of the vena cava. For this reason, some surgeons prefer to use venous bypass during the nonhepatic phase to avoid hemodynamic instability resulting from total closure of the inferior vena cava. (6)
Piggyback technique: The entire liver is stripped of the inferior vena cava, so the hepatic tributary is only partially preserved when the liver resection is completed. One of the main advantages of this technique is that the venous return is preserved during the hepatic phase, so this is the only technique possible when The venous tributary to the inferior vena cava is not present in the liver graft. (6)
Portal vein anastomosis
After completion of the inferior vena cava anastomosis, the portal vein anastomosis is performed in a comprehensive manner and blood is reperfused to the liver. Blood reperfusion is one of the most important parts of the transplantation process as it can be accompanied by profound hemodynamic instability (bradycardia and hypotension) resulting from the sudden entry of fluid residue. Cold and cytokine-rich transfer of the liver graft to the systemic circulation. To avoid this, the liver graft is washed with saline solution at room temperature and then with systemic blood, either from the portal vein or the inferior vena cava, to wash and warm the liver graft before re-infusion of blood into it. (6)
Hepatic artery anastomosis
End-to-end anastomosis between a donor’s celiac axis and the recipient’s common hepatic artery (at its junction with the gastroduodenal artery) is the most common and widely used technique for hepatic artery reconstruction. Depending on surgeon preference and anatomical factors, the level of hepatic artery reconstruction may vary as the focus is on Allowing only one simple anastomosis in the recipient, anastomosis of the recipient’s separate right hepatic artery branch with the donor gastroduodenal artery trunk is the easiest and most common reconstruction technique. (6)
Biliary anastomosis
After vascular anastomosis and establishing good hemostasis, the cholecystectomy is performed, and donor bile ducts are reconstructed. The preferred anastomosis is a conduit to duct between the common bile ducts of the donor and recipient, and when there is an unacceptable mismatch in duct size, or the recipient’s bile duct is unusable (due to Primary sclerosing cholangitis), Hepatic jejunostomy is performed. (6)
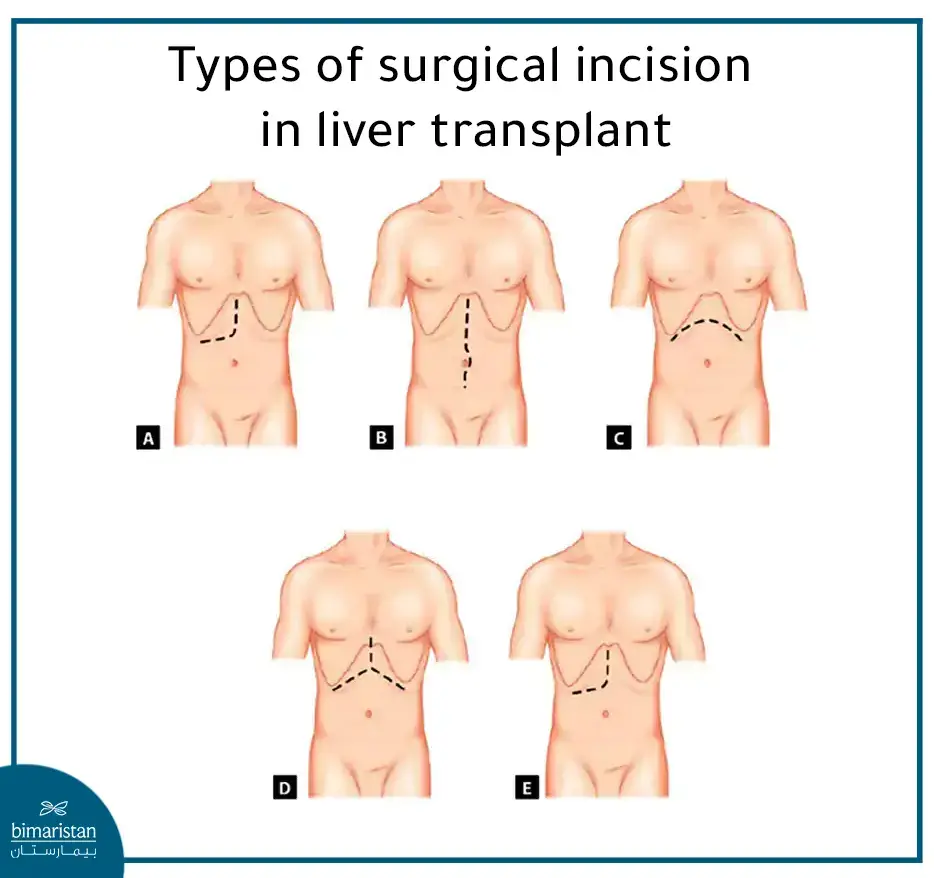
Postoperative care in liver transplantation
A patient who has had a liver transplant needs special care, and must fully follow the doctor’s recommendations.
Monitoring blood circulation after liver transplantation
Hemodynamic monitoring after liver transplantation is critical in post-operative care, and severe changes in hemodynamics that are not properly diagnosed or treated can lead to impaired liver graft function, prolong the length of stay in the intensive care unit, and increase Mortality rate, and management of post-operative circulatory problems begins with a comprehensive understanding of the causative pathophysiology. (7)
The end-stage liver disease typically causes increased cardiac output and decreased systemic vascular resistance, and this process begins to reverse after successful liver transplantation, resulting in decreased cardiac output and increased systemic vascular resistance with improved maintenance of systolic blood pressure. (7)
Early endotracheal extubation after liver transplantation
Early endotracheal extubation after liver transplantation is often possible due to advances in surgical and anesthetic techniques. The concept of early postoperative endotracheal extubation began in cardiac surgery and was applied to liver transplant patients in the late 1990s, and its proponents argue that it reduces the risk of pneumonia-associated pneumonia. On a ventilator, it improves splanchnic and hepatic blood flow, and has also been shown to reduce the length of stay in the intensive care unit. (7)
It is common for liver transplant patients to not be extubated early in the operating room, especially those with pre-existing lung diseases. There is a group of patients who will need a ventilator for a long period of time, which makes them vulnerable to additional pulmonary complications in the postoperative period. Therefore, It is crucial to recognize these patients and work to prevent them from developing ventilator-associated pneumonia (7)
Pain control after liver transplant
Liver transplantation is a major surgical procedure and may be associated with severe post-operative pain. Intraoperative and postoperative pain is usually controlled with fentanyl via intravenous infusion or intermittent dosing. Opiates such as morphine and hydromorphone are avoided if possible due to their long half-lives in the case of Liver failure. (7)
Some patients may need to use a patient-controlled analgesia pump in conjunction with long-acting analgesics or switch to oral medications around the clock if pain persists. Thoracic epidural anesthesia is useful for pain control after abdominal surgery but is not routinely used in liver transplant patients. (7)
Monitoring blood electrolytes after a liver transplant
Adequate management of electrolytes can be difficult in post-liver transplant patients, and patients often have several electrolyte disturbances that must be closely monitored and corrected. (7)
Hypernatremia is a less common complication in liver transplant patients and results from excessive free water loss in patients who use an osmotic laxative (eg, lactulose) to reduce hepatic encephalopathy. (7)
Hyperkalemia may be the most serious electrolyte disorder due to the rapid development of arrhythmia and death. The causes of hyperkalemia after liver transplantation are often multifactorial, as many liver transplant patients either have pre-existing renal dysfunction or will develop transient renal dysfunction in the operative period. And beyond, which can weaken potassium balance mechanisms. (7)
Hypocalcemia is frequently diagnosed in liver transplant patients. It is important to remember that these patients often have low albumin levels and that total calcium does not necessarily reflect free calcium levels, so ionomer calcium levels are more accurate in this situation.
Low calcium levels can result from chelation with anticoagulant citrate in blood products and dialysis agents, and hypocalcemia should be suspected in a patient with hypotension despite adequate resuscitation. (7)
Blood sugar levels after liver transplantation are crucial for both prognosis and complications. Hypoglycemia in the postoperative period may be a sign of bacteremia or poor liver graft function, while high blood sugar (which is more common postoperatively) is an indicator of disease. Latent diabetes may be a response to stress or the result of steroid administration.
Severe hyperglycemia (glucose > 200 mg/dL) is associated with an increased risk of liver allograft rejection, surgical site infections, and increased mortality. (7)
Coagulation disorders after liver transplantation
Coagulation disorders do not improve immediately after liver transplantation and often persist into the intensive care period after surgery. These are due to multifactorial causes that can include excessive fibrinolysis, disseminated intravascular coagulopathy, platelet activation, platelet trapping within the liver graft, And the presence of an effect similar to heparin.
Some patients also suffer from hypercoagulability after liver transplantation, which increases the complexity of evaluating their coagulation status. The cause of hypercoagulability is not completely clear, but it may result from poor synthesis of antithrombin by the liver. (7)
Immunosuppression after liver transplantation
Immunosuppression after liver transplantation is necessary to prevent rejection of the liver graft. However, immunosuppression must be balanced with maintaining other immune functions, especially preventing recurring infections and malignant tumors. Rejection of the transplanted liver occurs less frequently than other organs, so lower doses can be used. (7)
Steroids are used to suppress and control immunity during the first year after liver transplantation, as well as to treat episodes of acute rejection. There is concern that the use of high doses of steroids may accelerate the rates of recurrence of hepatitis C, recurrence of liver cancer, and cirrhosis. (7)
Avoiding the use of steroids for immunosuppression has not been shown to benefit HCV-positive recipients. Common severe side effects of high-dose steroids include:
- Hypertension
- Glucose intolerance
- Agitation/insomnia
- Risk of infection
- Poor wound healing
Most of these signs and symptoms can be controlled, so steroid use is rarely stopped.(7)
Rehabilitation after liver transplantation
Rehabilitation programs may help patients with liver disease and liver transplant recipients improve their quality of life by increasing muscle strength, preventing excessive fatigue, enhancing aerobic capacity, and increasing the level of physical activity. For this purpose, a specific, appropriate physical therapy plan must be developed based on the needs of patients at any stage. Stages of the disease by a physical therapist. Physical therapy after liver transplantation can be mainly divided into three periods: preoperative, postoperative, and delayed postoperative physical therapy. (8)
The reasons for participating in the rehabilitation process after liver transplantation and its contraindications must be well clarified. Any sign of acute rejection of the transplanted liver, severe bleeding, electrolyte imbalance, physiological instability, severe neurological complications, and severe cardiovascular disease may further affect the execution of movements. and specific exercises, so specialized stage-based assessment procedures must be performed before planning physical therapy programs. (8)
Post-liver transplant physical therapy evaluation should include muscle strength and endurance, ventilation capacity, level of physical activity, independence in activities of daily living, and health-related quality of life, and should determine neurological, metabolic, or musculoskeletal comorbidities, level of pain and fatigue, smoking, and alcohol habits. In the context of conducting the evaluation. (8)
Risks and complications of liver transplant
Liver transplantation has many complications, but we will go over them in detail and explain their cause to know their treatment and how to avoid them and the risks and complications include:
Respiratory problems after liver transplantation
Pulmonary complications can be very common after liver transplantation, with many recipients experiencing respiratory compromise requiring care ranging from close monitoring to prolonged mechanical ventilation. Preoperative predisposing factors include both underlying pulmonary disease and smoking. In addition, patients who are intubated before surgery are at risk of requiring mechanical ventilation after surgery due to underlying disease. (7)
Hepatopulmonary syndrome is a complication of cirrhosis that adds special concerns after liver transplantation, as it leads to increased mortality after surgery, especially in severe cases (PaO 2 < 50 mmHg in room air). Prolonged hypoxia after liver transplantation is a complication. Most common in patients with this syndrome. (7)
Infectious complications after liver transplantation
Infections are the major cause of morbidity and mortality after liver transplantation, and the early post-transplant period (first month) is often complicated by incision infections and hospitalization-related infections including urinary infections, pneumonia, septicemia, and pseudomembranous colitis (7).
Patients after liver transplantation are particularly at risk of developing bacterial infections in the liver and surgical incision, including abscesses, cholangitis, and peritonitis, so standard antibiotics should be used prophylactically in the perioperative period to reduce the risk of infections. (7)
Renal complications after liver transplantation
Renal failure after liver transplantation is a common occurrence, and some studies indicate a rate that may reach 50% of cases. and acute ischemic tubular necrosis is the most common cause of early kidney failure after liver transplantation. (7)
There are a number of factors that contribute to an increased risk of kidney disorders after liver transplantation, including:
- Hepatorenal syndrome
- Hepatitis C
- Diabetes
- Hemodynamic instability during and after surgery
- Large blood transfusion
- Intravenous infusion of vasoconstrictors
- Infections
- Repeated radiological procedures
- Immunosuppressants and antibiotics that are harmful to the kidneys (7)
Thrombocytopenia after liver transplantation
Low platelet count is a common disorder after liver transplantation. The causes of thrombocytopenia are diverse but are linked to a decrease in their number in circulation and a decrease in their production. (7)
In the case of severe cirrhosis, there is often significant retention of platelets in the spleen due to high portal vein blood pressure, and the new liver graft will also trap platelets. There is a decrease in platelet production due to low levels of thrombopoietin in patients with liver failure, and large amounts of blood transfusion can Significant postoperative period leads to increased thrombocytopenia. (7)
Graft rejection after liver transplant
There are many types of liver graft rejection that may occur after a liver transplant. Graft rejection can be hyperacute, acute, chronic, or graft-versus-host disease. (7)
Rejection can be mediated by T lymphocytes or by antibodies, and the process often targets the interlobular bile ducts, the vascular endothelium in the portal vein, hepatic veins, and sometimes the hepatic artery and its branches. (9)
High-acute antibody-mediated rejection occurs within minutes to hours after liver transplantation and occurs in 60% of cases due to an allograft that is incompatible with the ABO blood group. In this case, plasmapheresis, splenectomy, CD20 monoclonal antibody are used, and rituximab to prevent a hyperacute rejection event, but immediate retransplantation is often the only option. (7)
To know more about the drug rituximab, you can review the article Treating Hodgkin and Non-Hodgkin Lymphoma.
Acute rejection is caused by T lymphocytes and usually appears within days or weeks of liver transplantation in 36-75% of cases. Acute rejection is characterized by mononuclear inflammation and active cell damage, and episodes of resistance to anti-rejection drugs can develop leading to chronic rejection. (7)
Rejection due to graft-versus-host disease occurs in 1-2% of liver transplant recipients and is associated with a mortality rate of 85%. In the case of solid organ transplantation, donor lymphocytes remaining in the parenchyma become detectable in the recipient within weeks after transplantation, and these competent cells react with Immunity against various cellular antigens present in the recipient. This form of rejection is divided between an acute type (which occurs within 100 days of transplantation) and a chronic type (after 100 days of transplantation). (7)
Results of liver transplant surgery
Outcomes for liver transplant patients continue to improve due to improvements in both surgical techniques and immune stabilization regimens and because of better management of infections and post-transplant complications, yet donor shortages remain the greatest challenge facing the liver transplant sector today. (2)
Given the high rates of morbidity and mortality associated with end-stage liver disease, it is essential that physicians caring for such patients have a valid and reproducible system for estimating the severity and prognosis of the disease, and this system will be useful in identifying those who need a liver transplant. (2)
Physiological rather than chronological age determines the acceptability of an older patient for liver transplantation. With careful attention to comorbidities and functional status, overall outcomes are acceptable in recipients over 70 years of age, although they are less good than in younger age groups. (4)
Quality of life at 10 years and 30 years after liver transplantation was taken into account. Patients’ expectation of quality of life was generally good and was only low in the elderly, whose ability to do physical activity was reduced compared to the general population. No difference was observed in terms of the quality of transplantation. liver disease between male and female patients, but one study indicated that overall quality of life was higher in male recipients compared to females. (4)
In the end, we find that liver transplantation is one of the best operations performed in Turkey to solve liver problems once and for all, and that the cost of liver transplantation in Turkey is much lower than in other countries, with almost the same quality and expected results, and that many patients talked about my experience with liver transplantation. In Turkey, all comments were positive and promising, even long after they had donated their liver or had a liver transplant.
How long does a patient live after a liver transplant?
Life expectancy after a liver transplant depends on many factors, including:
- Patient age: In general, younger people live longer after a liver transplant than older people.
- Patient health: People who are generally healthy before surgery tend to live longer after it.
- Cause of liver damage: Survival rates vary depending on the cause of liver damage. For example, people who undergo a liver transplant for alcoholic cirrhosis live longer than people who undergo a liver transplant for hepatitis B or C.
- Type of liver transplant: People who receive a liver from a living donor live longer than people who receive a liver from a dead donor.
- Follow-up care: After surgery, it is important to carefully follow your doctor’s instructions, including taking anti-rejection medications and attending regular follow-up appointments. Adherence to follow-up care can positively impact life expectancy.
in general,
- About 75% of people who undergo a liver transplant can live for at least 5 years.
- 50% of people who undergo a liver transplant can live for at least 10 years.
- 20% of people who undergo a liver transplant can live for at least 20 years.
Liver transplant cost in Turkey
Liver transplant cost in Turkey varies according to the type of center
The cost of liver transplantation in state medical city hospitals ranges between 30 and 37 thousand US dollars.
While its cost in university hospitals specializing in organ transplantation ranges between 45 and 55 thousand US dollars.
While the cost of liver transplantation in private hospitals ranges between 50 and 80 thousand US dollars.
| Hospital Type | Cost with Viral Infection (Hepatitis B or C) | Cost without Viral Infection |
|---|---|---|
| International Hospital | 35,000$ | $45,000 |
| $45,000 | $45,000 | $55,000 |
| Private Hospital | $70,000 | $80,000 |
Sources:
- Bulur A and Sevmiş M. Clinical, surgical and histopathological characteristics of liver transplant recipients: An analysis of a large sample from Turkey. Gulhane Medical Journal 2022;64:60-66.
- Ionescu, V.A, Diaconu C.C, Bungau S, Jinga V, Gheorghe G. Current Approaches in the Allocation of Liver Transplantation. J. Pers. Med. 2022;12,1661.
- Mahmod N. Selection for Liver Transplantation: Indications and Evaluation. Current Hepatology Reports 2020;19:203-212.
- European Association for the Study of the Liver. EASL Clinical Practice Guidelines: Liver transplantation. Journal of Hepatology 2016;64:433-485.
- Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alono-Coello P, et al. Evaluation for Liver Transplantation in Adults: 2013 Practice Guideline by the American Association for the Study of Liver Diseases and the American Society of Transplantation. BMJ 2008;336:924-926.
- Miller C and Diago Uso T. The Liver Transplant Operation. Clinical Liver Disease 2013; 2,(4):192-196.
- Parekh K.N, et al. Postoperative Care of the Liver Transplant Recipient. Springer 2017;29:365-384.
- Yıldırım M.S, Yurdalan S.U. Physiotherapy in Liver Transplantation. InTech 2012;21:445-454.
- Zhu J.H, et al. Medical complications of liver transplantation. AME Medical Journal 2018;3:1-10.