يشمل علاج كسور الوجه في تركيا الكثير من عظام الوجه ومنها كسور الفك العلوي، ومن بين تصنيفات كسور الفك العلوي، يعتبر تصنيف Le Fort التصنيف الأكثر شهرة.
أجرى العالم لو فورت تجاربه التي حددت مناطق ضعيفة بنيوياً في الفك العلوي والتي وصفها بأنها خطوط الضعف. وفقاً لهذه النتائج، هناك ثلاثة أنواع أساسية للكسور (المستعرض، الهرمي، والانفصال القحفي الوجهي).
ينتج عن علاج كسور الوجه عجز تجميلي ووظيفي إذا لم تتم بالشكل الصحيح.
ما هي كسور لو فورت؟
كسور لو فورت هي مجموعة من كسور الوجه التي تؤثر على منطقة الثلث المتوسط من الوجه وتسبب مجتمعة فصل جزئي أو كامل لمنطقة الثلث المتوسط من الوجه عن الجمجمة.
تشير منطقة الثلث المتوسط من الوجه إلى المنطقة الممتدة بين الزوايا الخارجية للعين وزوايا الفم ، والتي تتكون من الأنف والخدين والمنطقة فوق الشفة العليا، عادةً ما تشمل كسور لو فورت الصفائح الجناحية للعظام الوتدية ، والتي تشكل قاعدة الجمجمة، وتمتد خلف العين وأسفل الجزء الأمامي من الدماغ.
الصفائح الجناحية هي نتوءات في العظم الوتدية وتربط الوجه الأوسط بالعظم الوتدي، قد تتسبب كسور لو فورت في انسداد في مجاري الهواء مما قد يهدد الحياة إذا لم يتم التعرف عليه ومعالجته بشكل صحيح من قبل أخصائي طبي.
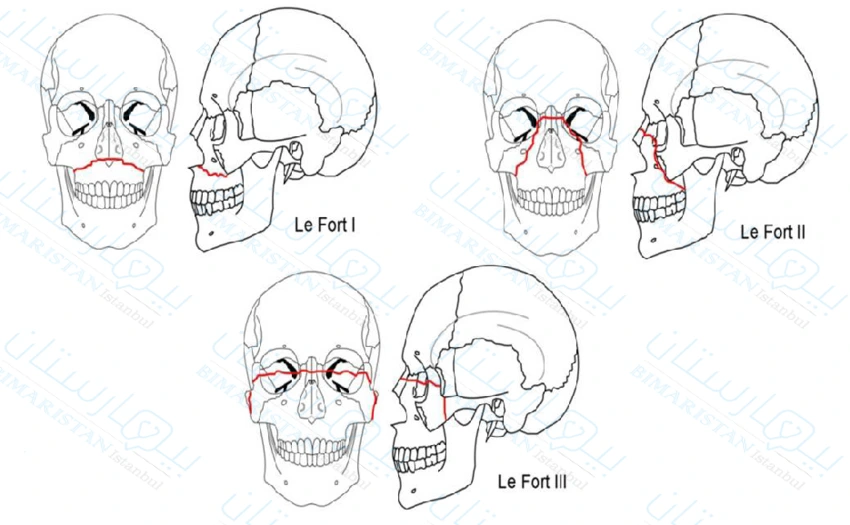
هناك ثلاثة أنواع من كسور لو فورت التي يمكن تصنيفها وفقاً للمستوى الذي تمت به الإصابة، في النوع الأول من كسور لو فورت يكون مستوى الإصابة أفقياً وينتج عنه عادةً انفصال الأسنان عن الجزء العلوي من الوجه.
يمر خط الكسر الأفقي عموماً عبر الحافة السنخية وهي التجويف العظمي الذي يحمل الأسنان والأنف الجانبي والجزء السفلي من الجيب الفكي وهو أحد الجيوب الأنفية الأربعة الموجودة بالقرب من الأنف.
من بين كسور لو فورت، فقط النوع الأول منها يشمل الحافة الأمامية الوحشية للحفرة الأنفية. لذلك، فإن عدم وجود كسر في هذه المنطقة يستبعد حدوث كسر لو فورت من النوع الأول.
يتميز Le Fort من النوع الثاني بكسر هرمي الشكل، تشكل الأسنان العلوية القاعدة ويشكل الدرز الجبهي الأنفي الذي يربط العظم الجبهي بالعظم الأنفي قمة الكسر الهرمي.
يمكن أن يحدث الكسر الهرمي عند الحافة السنخية والجيوب الأنفية الفكية ولكن عادةً ما يمتد أيضاً عبر الحافة الحجاجية (تجويف العين) وعظام الأنف.
غالباً ما يتم إدخال المرضى الذين يعانون من النوع الثاني إلى المستشفى فاقدين للوعي ويجب الانتباه لوجود للأجسام الغريبة مثل الأسنان أو شظايا الأسنان التي قد تسد الشعب الهوائية وقد يصاحبها نزيف حاد أو تسرب السائل الدماغي الشوكي.
في كسر Le Fort من النوع الثالث يكون مستوى الإصابة مستعرضاً أو أفقياً مثل النوع الأول؛ ومع ذلك في النوع الثالث تبدأ الإصابة عادةً في المنطقة الأنفية الجبهية وتمتد عبر جدران الحجاج وقوس الوجنة والصفائح الجناحية.
يعرف كسر لو فورت من النوع الثالث أنه نوع أكثر شمولاً لأنه يمكن أن يؤدي إلى فصل كامل لمنطقة الثلث المتوسط من الوجه عن قاعدة الجمجمة ولذلك يعرف باسم الانفصال القحفي الوجهي.
ما الذي يسبب كسور الوجه؟
غالباً ما تحدث اصابات الوجه في حوادث السيارات حيث تصطدم منطقة الثلث المتوسط من الوجه بجسم ثابت، مثل مقود السيارة لذلك يوصى دائماً باستخدام حزام الأمان من أجل تقليل خطر كسور الوجه. يمكن أن يحدث أيضاً في حالة إصابة منتصف الوجه بجسم صلب، مثل مضرب بيسبول.
إذا تم توجيه القوة نحو منتصف الوجه مباشرة ينتج النوع الأول أو الثاني من كسور لو فورت، أما إذا تم توجيه القوة إلى الأسفل، ينتج النوع الثالث عادةً.
هذا وقد أكدت الدراسات على وجود ترابط وثيق بين الإصابات الجبهية وكسور لو فورت.

كيف يتم تشخيص كسور الوجه؟
تعد مراجعة التاريخ الطبي للفرد والفحص البدني الشامل أمراً ضرورياً في تشخيص كسور لو فورت، يمكن أن يساعد الفحص السريري للكسر، جنباً إلى جنب مع بعض العلامات والأعراض المختلفة في الحصول على تشخيص دقيق للكسر وذلك للبدء بإجراء العمليات لعلاج كسور الوجه:
- يعد كسر الصفائح الجناحية أساسياً في تشخيص كسور الوجه.
- الحافة الأمامية الوحشية للحفرة الأنفية: إذا كانت مكسورة فالكسر هو من النوع الأول من كسور لو فورت، أما إذا كانت سليمة فيجب عندها استبعاد النوع الأول.
- الحافة السفلية للحجاج: إذا كانت مكسورة فالكسر هو من النوع الثاني من كسور لو فورت، أما إذا كانت سليمة فيجب عندها استبعاد النوع الثاني.
- القوس الوجنية: إذا كانت مكسورة فالكسر هو من النوع الثالث من كسور لو فورت، أما إذا كانت سليمة فيجب عندها استبعاد النوع الثالث.
- تشير إصابة الدرز الأنفي الجبهي إلى كسر من النوع الثاني أو الثالث.
- لدى العديد من المرضى الذين يعانون من كسور لو فورت، يحدث لديهم التهاب عصبي رضحي يكون أكثر وضوحاً في الفروع تحت الحجاج من العصب ثلاثي التوائم، وفي بعض الحالات، تحدث استثارة كهربائية تلقائية مستمرة وطويلة الأمد في أسنان الجانب المصاب بكسر لوفورت.
- قد تحدث مجموعة من الكسور في جانب واحد من الوجه.
- قد تحدث كسور ثنائية الجانب ولكن غير متناظرة.
- وقد تترافق مع كسور في عظام الوجه الأخرى.
تظهر كسور النوع الأول عادةً مع تورم طفيف في الشفة العلوية، وكدمات في سطح الشدق (منطقة الخد من داخل الفم)، وعدم انتظام للأسنان (سوء إطباق)، وتخلخل في الأسنان (نتيجة ضعف البنى الداعمة للأسنان كاللثة).
تظهر كسور النوع الثاني عادةً مع تشوه كبير وتورم في منتصف الوجه، واتساع المسافة بين الزوايا الداخلية للجفون (أي المسافة بين الموقين)، ويصبح الفك العلوي والأنف قابل للحركة، ونلاحظ سوء إطباق الأسنان.
بالإضافة إلى ذلك، قد يعاني المرء من تورم حول العينين (وذمة حول الحجاج)، كلف وتكدم حول العينين (كدمات حول الحجاج)، ونزيف في الأنف (رعاف)، وكدمات في دهليز الفم (المنطقة بين السطح الأمامي للأسنان والسطح الخلفي للشفة)،
ومن الشائع أيضاً حدوث تسرب للسائل الدماغي الشوكي عبر الأنف (CSF rhinorrhea)، والذي يظهر غالباً على شكل سيلان أنفي مائي غزير.
أخيراً، تظهر كسور النوع الثالث من كسور لو فورت عادةً بأعراض مشابهة للنوع الثاني، بالإضافة إلى إطالة وتسطح وجهي بشكل ملحوظ وذلك بسبب تعرض الفك المكسور للإزاحة إلى الأسفل أو إلى الداخل (إلى الخلف) ووجع عند محاولة إغلاق الأسنان وسوء إطباق.
بالإضافة إلى حدوث نزيف من الفم، وزيادة الجلد على الجفن العلوي، كما يمكن ملاحظة حدوث الخوص (غؤور العين) وكدمات في الخشاء (المنطقة التي توجد خلف الأذن)، قد يعاني الأفراد أيضاً من نزح أذني ووجود الدم في الأذن الوسطى (نزف في جوف الطبل).
غالباً ما يلزم إجراء فحص بالتصوير المقطعي المحوسب CT لعظام الوجه للحصول على فكرة شاملة عن مدى الإصابة.
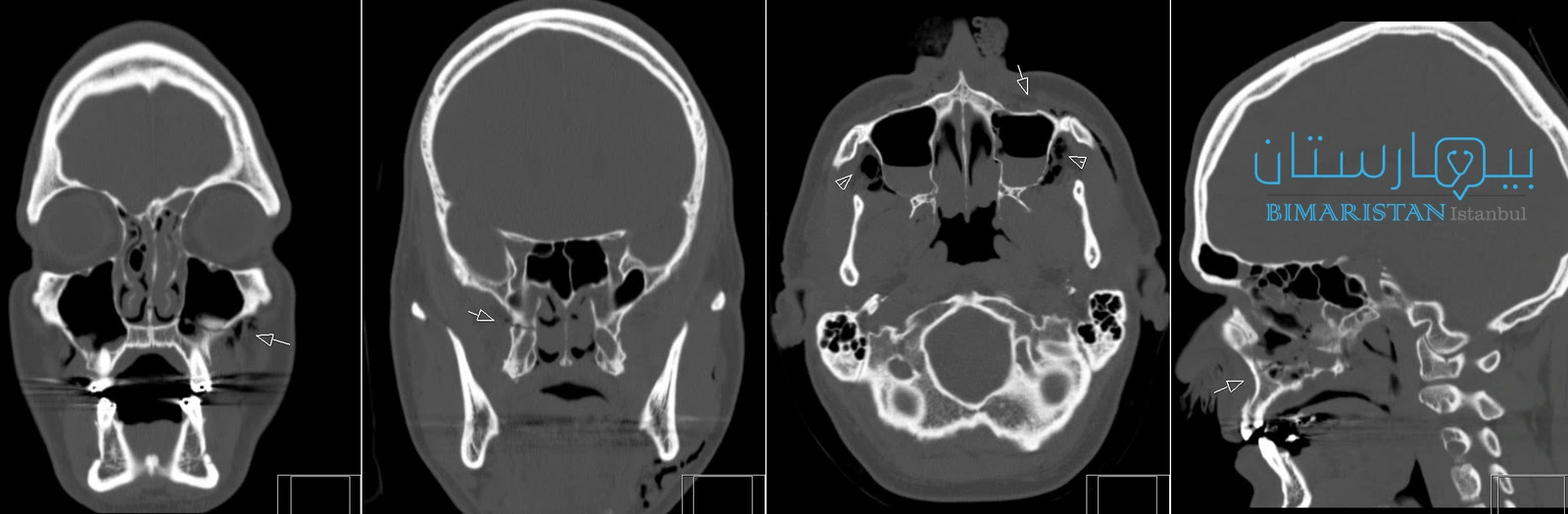
عادةً ما يتطلب علاج كسور الوجه تثبيتاً سريعاً للكسر متبوعاً بالجراحة، من أجل استعادة الاتجاه النموذجي للوجه، واستعادة الوضع الصحيح للأسنان، واستعادة الجيوب الأنفية المصابة، وإعادة توحيد الأنف و محجر العين.
الجراحة لعلاج كسور الوجه في تركيا
يتم توفير الرعاية الجراحية من قبل أخصائيي الجراحة في العيادات أو في أقسام جراحة الوجه والفكين بشكل أساسي للمتضررين الذين يحتاجون إليها وفقاً للإشارات الحيوية الخاصة بهم بعد علاج كسور الوجه.
وتشمل هذه المرضى الذين يعانون من علامات الصدمة والنزيف وفقدان الدم الحاد والاختناق. على سبيل المثال، إذا كانت الحالة هي نزيف من الأوعية الكبيرة في منطقة الوجه والفكين لا يمكن الاعتماد على الضمادة الاعتيادية لوقف النزيف عند علاج كسور الوجه.
لذلك، يتم تقسيم جميع المرضى الذين يعانون من إصابات في منطقة الوجه والفكين إلى ثلاث مجموعات:
- المجموعة الأولى – لا تتطلب سوى الرعاية الجراحية (جروح في الأنسجة الضامة دون عيوب حقيقية، حروق من الدرجة II)؛ بالنسبة لهم هذه المرحلة من العلاج نهائية.
- المجموعة الثانية – يحتاجون إلى رعية جراحية متخصصة (الأنسجة الضامة مصابة بجروح تتطلب العلاج الجراحي بالإضافة للجراحة التجميلية، مثل: أضرار في عظام الوجه والفكين، وحروق من الدرجة III-IV)؛ بعد تقديم الرعاية الجراحية الطارئة، يتم نقلهم إلى مستشفيات الوجه والفكين لإجراء الجراحة التجميلية.
- المجموعة الثالثة – هم المصابين غير القابلين للنقل، فضلاً عن الأشخاص الذين يعانون من إصابات مترافقة مع مناطق أخرى من الجسم (وخاصة عضلة القلب).
أحد الأسباب التي تستدعي إعادة العلاج الجراحي هو أن التدخل الجراحي الفوري حصل بدون إجراء فحص شعاعي أولي، والتي هي أساسية في التشخيص.
عند تقديم الرعاية الجراحية لعلاج كسور الوجه لضحايا المجموعة الثانية الذين سيتم إرسالهم إلى المؤسسات الطبية المتخصصة (إذا لم يكن لديهم موانع للنقل)، يجب على الجراح:
- استخدام التخدير لفترات طويلة في موقع الكسر.
- استخدام المضادات الحيوية.
- التأكد من عدم وجود نزيف من جرح قد يشكل سبباُ لجعل المصابين غير قابلين للنقل.
- ضمان نقل المريض المصاب بشكل مناسب لمؤسسة طبية متخصصة، بمرافقة أفراد الفريق الطبي (تحديد طريقة النقل، ووضعية المريض).
في الآونة الأخيرة أصبحت تركيا من الدول الرائدة في مجال السياحة العلاجية على مستوى العالم لا تتردد بالتواصل معنا.
في الحالات التي يكون فيها موانع تحول دون نقل المصاب إلى مؤسسة طبية أخرى (المجموعة الثالثة)، يتم تزويده بمساعدة أولية تؤهله للنقل إلى قسم الجراحة بمشاركة أطباء الأسنان الموجودين في المستشفيات، وذلك بوجود:
- أخصائي جراحة عامة وجراح عظام، إذ يجب أن يكون على دراية بأساسيات رعاية كسور الوجه والفكين، ليتوافق مع مبادئ علاج كسور الوجه، وكذلك ليتمكن من تقدير حالة المصاب وتحديد المجموعة التي ينتمي إليها والتأكد من وجود سبب يمنعه من النقل في حال كان ينتمي للمجموعة الثالثة.
- جراح الوجه والفكين، حيث يجب أن يتم علاج كسور الوجه عند المرضى في المستشفى بمشاركة جراح الوجه والفكين.
- طبيب أسنان لكي يستطيع تحديد مدى إصابة الأسنان وتغير انتظامها للبدء بخطة علاج ما بعد الجراحة.
إذا لم يتم إصلاح وعلاج كسور الوجه فغالباً ما ترتبط الكسور الواسعة في منطقة الثلث المتوسط من الوجه بتشوهات وظيفية وتجميلية كبيرة.
على الرغم من أن الكسور بالعظام تحتاج في النهاية إلى تقويم وتصليح جراحي إلا أن العلاج الطبي الفوري ضروري ويمكن أن يشمل المضادات الحيوية ومزيلات احتقان الأنف، يمكن أن تقلل الستيرويدات عن طريق الفم أو الوريد من التورم ولكنها لم تظهر أي فائدة للمشاكل طويلة المدى مثل اعتلال العصب البصري.
قد تكون هناك حاجة لتدخلات عاجلة مثل:
- إزاحة أجزاء من الفك العلوي من أجل الحفاظ على مجرى الهواء مفتوحاً: يمكن إجراء إزالة الشوائب الفكية يدوياً أو باستخدام ملقط كبير.
- الإصابات الحجاجية التي تهدد سلامة عضلات العين أو العصب البصري.
عندما يصبح المصاب مستقراً عصبياً وسريرياً، يتم نقله لقسم الجراحة، حيث يتضمن الإصلاح الجراحي لعلاج كسور الوجه ما يلي:
- استعادة النتوءات الوجهية وتجاويف الجيوب الأنفية المصابة.
- استعادة سلامة الأنف والحجاج.
- عملية الاختزال المفتوح مع التثبيت الداخلي (ORIF) تنطوي هذه العملية على مرحلتين هما الاختزال المفتوح والتي تعيد ترتيب العظم المكسور لوضعه الطبيعي لتثبيت العظم داخلياً والذي يُقصد به تثبيت كسور الفك العلوي في مكانها جراحياً حتى يتم الشفاء بالشكل الصحيح.
يتم إجراؤها في الحالات المتقدمة من كسور العظام مثل العظم المتفتت أو بروز العظم من الجلد أو خلع المفصل.
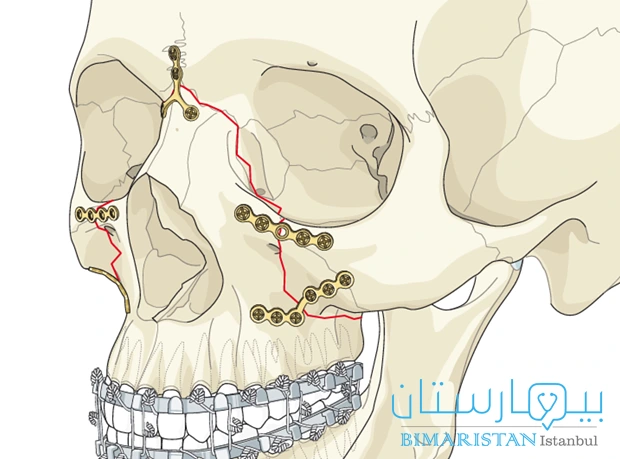
تتم إجراء عملية علاج كسور الوجه من قبل جراح العظام الذي يبدأ بتخدير المريض لتخفيف الألم ثم يتم الإجراء على مرحلتين:
المرحلة الأولى: وتنطوي على إعادة وضع العظام المكسورة في مكانها الصحيح لاستعادة الاستقامة الطبيعية، مع ضمان وضع العظام بأقل عدد ممكن من الفراغات أو الانحناءات.
المرحلة الثانية: وهي التثبيت الداخلي المبني على تثبيت العظام المكسورة معاً من خلال استخدام أنواع مختلفة من الأجهزة، مثل: المسامير المعدنية والقضبان الصلبة والبراغي و شرائح بصورة دائمة أو مؤقتة، وتكون عادة مصنوعة من مواد معدنية قوية مثل التيتانيوم أو الفولاذ المقاوم للصدأ بهدف توفير الدعم والثبات للعظام أثناء علاج كسور الوجه.
مضاعفات الجراحة لعلاج كسور الوجه
ينطوي الإجراء الجراحي السابق لعلاج كسور الوجه على عدة مخاطر:
- مشكلة تأذي الأعصاب.
- حدوث بعض التغيرات في الدورة الدموية.
- حدوث خلل في آلية المضغ (بما في ذلك المفصل الفكي الصدغي).
- شفاء العظم خارج الاستقامة الصحيحة.
- مضاعفات في الرؤية، المضاعفات العينية وتشمل انخفاض في حدة البصر، واختلال وظيفي في عضلات خارج المقلة، والتهاب القرنية العصبي ومشاكل في الجهاز الدمعي بما في ذلك الدُماع.
- سوء إطباق مع عدم استقرار في الفك العلوي إذ قد يحدث نتيجة عدم كفاية العظم لسد الفراغ أو نتيجة التثبيت الضعيف أو غير المناسب، التي قد تظهر بعد 4 أسابيع من التثبيت.
- إصابة العصب تحت الحجاج أو فوق الحجاج المصحوبة بفرط ضغط مستمر، إذ يجب على الطبيب الحرص على تحديد مكان جذور الأعصاب والحفاظ عليها أثناء الجراحة لعلاج كسور الوجه.
- التهاب العقد اللمفية والتهاب المفاصل والخراجات والتهابات في النسيج الضام والتهاب الجيوب الأنفية.
- قد تظهر بعض المضاعفات في جهاز التنفس والتي غالبا ما تكون سبب وفاة هؤلاء المرضى، عندها يتم تقديم العلاج بالهرمونات من قبل إخصائي علاج كسور الوجه.
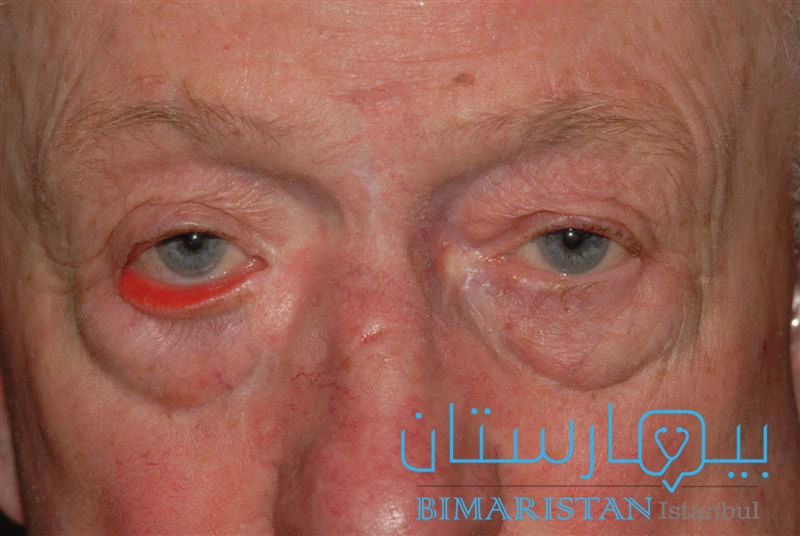
- الشتر الخارجي للجفن السفلي حيث يتدلى الجفن السفلي بعيداً عن العين ويتجه للخارج، لا يكون خطيراً في العادة، لكنه قد يكون غير مريح ويمكن أن يحدث في عين واحدة أو في كلتا العينين.
تعليمات ما بعد الجراحة لعلاج كسور الوجه
- المحافظة على نظافة الفم من خلال التنظيف الدوري للأسنان.
- اقتصار الغذاء على الأطعمة المهروسة والسائلة.
- تناول الأدوية ومضادات الالتهاب بانتظام كما وصفها الأطباء المختصين مع المراجعة الدورية للطبيب، يمكنك التواصل معنا لحجز مواعيد.المتابعة مع طبيب العيون من أجل ملاحظة أي تغييرات في الرؤية مثل ازدواجية الرؤية.
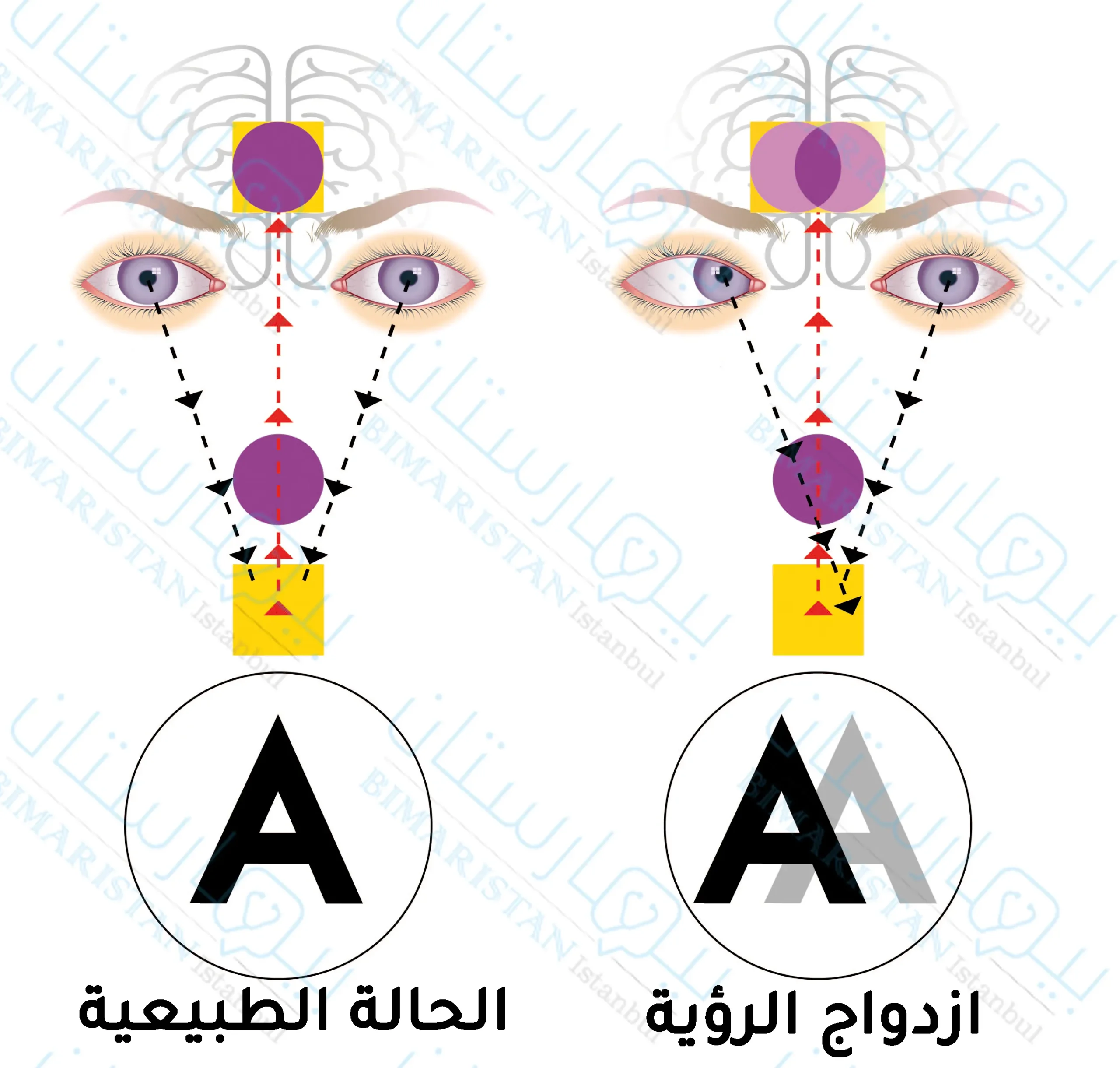
- حالة ازدواج الرؤية