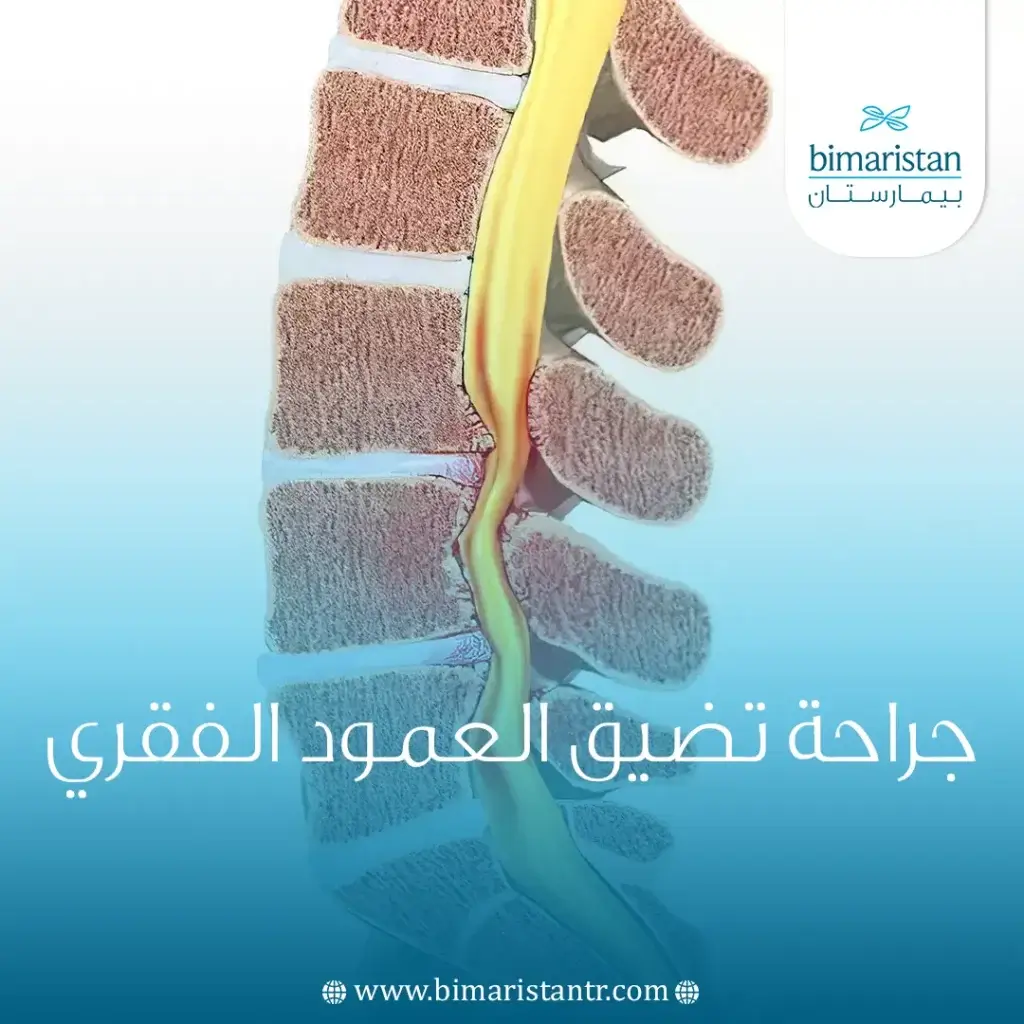
جراحة تضيق العمود الفقري أو القناة الشوكية في تركيا والتي تتم باستخدام المجهر الالكتروني لعلاج الانضغاط الناتج عن النتوء العظمي أو الغضروفي على القناة الفقرية.
تضيق العمود الفقري
تضيق العمود الفقري هو حالة شائعة تحدث عندما تنضغط القناة الشوكية الصغيرة، التي تحتوي على جذور الأعصاب والحبل الشوكي على النخاع الشوكي و/أو جذور الأعصاب، مما يؤدي إلى الشعور بالألم والتشنج والضعف أو التنميل. اعتمادًا على مكان حدوث التضيق، قد تشعر بهذه الأعراض في أسفل الظهر والساقين أو الرقبة أو الكتف أو الذراعين.
عادة يحدث التضيق بسبب هشاشة العظام، أو التهاب المفاصل للعمود الفقري والأقراص بين الفقرات (عظام الظهر).
قد يكون أيضًا بسبب سماكة الأربطة في الظهر، وكذلك بسبب انتفاخ الأقراص التي تفصل الفقرات.
غالبًا ما تبدأ أعراض تضيق القناة الشوكية ببطء وتزداد سوءًا بمرور الوقت.
قد يصبح الألم في الساقين شديدًا لدرجة أنه يصعب المشي حتى لمسافات قصيرة.
في كثير من الأحيان، يحتاج المصابون للجلوس لتخفيف الألم مؤقتًا.
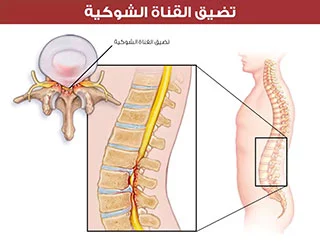
ما هو تضيق العمود الفقري؟
تضيق العمود الفقري هو تضيق منطقة أو أكثر من مناطق العمود الفقري.
هذا التضيق، الذي يحدث غالبًا في أسفل الظهر أو الرقبة، يمكن أن يضغط على الحبل الشوكي أو الأعصاب التي تتفرع من المناطق المضغوطة.
عادةً ما يشكو الشخص المصاب بهذه الحالة من ألم شديد في الساقين أو بطة الساق أو أسفل الظهر عند الوقوف أو المشي. قد يأتي الألم بسرعة أكبر عند المشي صعودا أو نزولاً من تل أو منحدر أو سلالم. عادة يتم تخفيف الألم عن طريق الجلوس أو الانحناء.
ما الذي يسبب تضيق العمود الفقري وعلى من يؤثر؟
يولد بعض الناس بقناة شوكية صغيرة. وهذا ما يسمى “التضيق الخلقي”.
ومع ذلك، فإن تضيق العمود الفقري غالبًا ما يكون بسبب التغيرات المرتبطة بالعمر التي تحدث بمرور الوقت. وهذا ما يسمى “تضيق العمود الفقري المكتسب”.
يزداد خطر الإصابة بتضيق العمود الفقري في الحالات التالية:
- عند المولودين بقناة شوكية ضيقة.
- عند الإناث.
- بعد بلوغ سن 50 سنة.
- عند الذين تعرضوا لإصابة سابقة أو خضعوا لجراحة في العمود الفقري.
كما يمكن أن تسبب بعض الحالات الطبية تضيقاً في العمود الفقري. وهي:
- هشاشة العظام والنتوءات العظمية (المناقير) التي تتشكل مع تقدمنا في العمر.
- التهاب الفقار الروماتويدي (على سبيل المثال، التهاب الفقار اللاصق).
- أورام العمود الفقري.
- مرض باغيت: وهو مرض مزمن يصيب كبار السن ويتمثل في تلف نسيج العظم وخاصة في العمود الفقري أو الجمجمة أو الحوض
كيف يتم تشخيص تضيق العمود الفقري في تركيا؟
سيسألك الطبيب المختص عن الأعراض الموجودة لديك وعن تاريخك المرضي.
إذا اشتبه في حدوث تضيق في العمود الفقري، فسيقوم بإجراء فحص لجسمك. تشمل بعض الأعراض التي سيبحث عنها ما يلي:
- خدر أو ضعف أو تشنج أو ألم في الساقين أو الفخذين أو القدمين مما يجعل المشي صعبًا عليك.
- الألم الممتد إلى أسفل الساق.
- خلل في وظيفة الأمعاء و/أو المثانة.
- فقدان الوظيفة الجنسية.
في الحالات الشديدة، شلل جزئي أو كامل في الساق. تعتبر هذه حالة طبية طارئة ويجب عليك الوصول إلى غرفة الطوارئ في أسرع وقت ممكن.
سيأخذ أخصائي الروماتيزم في الاعتبار أيضًا الحالات الأخرى التي يمكن أن تسبب أعراضًا مماثلة، مثل التهاب المفاصل في الوركين أو الركبتين؛ اضطرابات في الجهاز العصبي.
أو اضطرابات القلب والأوعية الدموية. قد يطلب أخصائي أمراض الروماتيزم أيضًا اختبارات أخرى لتأكيد التشخيص وتحديد مدى خطورة حالتك. وتشمل هذه:
- الأشعة السينية للعمود الفقري للتأكد من وجود هشاشة العظام والنتوءات العظمية (المناقير) وتضيق القناة الشوكية.
- التصوير بالطبقي المحوري (CT SCAN)، والذي يأخذ صورًا أكثر تفصيلاً للظهر والقناة الشوكية.
- التصوير بالرنين المغناطيسي (MRI SCAN) للعمود الفقري لالتقاط صور للحبل الشوكي والأعصاب.
- مخطط كهربية العضل (EMG) لفحص الأعصاب النازلة إلى ساقيك.
- الأشعة السينية للوركين أو الركبتين، وتحاليل الدم، وكذلك اختبارات لفحص الدورة الدموية في ساقيك واستبعاد الأمراض الأخرى ذات الأعراض المماثلة.
كيف يتم معالجة تضيق العمود الفقري في تركيا؟
على الرغم من عدم وجود علاج نهائي لتضيق العمود الفقري، إلا أن التمارين المنتظمة والأدوية والجراحة في بعض الحالات يمكن أن توفر للمريض الراحة.
-
ممارسه الرياضة:
يمكن أن تساعدك التمارين المنتظمة في بناء والحفاظ على قوة عضلات ذراعيك وأعلى ساقيك (العضلات القابضة والباسطة للورك والعضلة رباعية الرؤوس وأوتار الركبة).
سيؤدي ذلك إلى تحسين توازنك وقدرتك على المشي والانحناء والتحرك بالإضافة إلى التحكم في الألم.
يمكن لأخصائي العلاج الطبيعي أن يوضح لك التمارين المناسبة لك.
-
الأدوية:
الأدوية التي لا تستلزم وصفة طبية مثل أسيتامينوفين (تايلينول)، أو مضادات الالتهاب غير الستيرويدية مثل الإيبوبروفين (أدفيل، موترين) أو النابروكسين (أليف، أنابروكس)، قد تخفف الألم أيضًا.
بالإضافة إلى ذلك، قد يصف الطبيب أدوية أخرى للمساعدة في الألم و/ أو تشنج العضلات.
-
حقن الكورتيزون (حقن الكورتيكوستيرويد):
قد يوفر الحقن مباشرة في المنطقة المحيطة بالحبل الشوكي (المعروفة باسم الحقن فوق الجافية) قدرًا كبيرًا من الراحة المؤقتة والعرضية.
ومع ذلك فإن هناك القليل من البيانات الموضوعية التي تدعم استخدام حقن الكورتيزون لعلاج تضيق العمود الفقري.
عادة ما يتم إعطاء هذه الحقن في العيادة الخارجية في المستشفى أو العيادة.
جراحة تضيق العمود الفقري في تركيا
إزالة الضغط عن العمود الفقري ودمج الفقرات
هل تحتاج الى جراحة لعلاج تضيق العمود الفقري؟
يستجيب معظم المرضى الذين يعانون من تضيق العمود الفقري العنقي أو القطني جيدًا للعلاجات غير الجراحية (مثل الأدوية)، لذلك قد لا تحتاج إلى جراحة العمود الفقري.
ومع ذلك، هناك حالات قد تتطلب المضي قدمًا في جراحة العمود الفقري:
- عدم الاستجابة للعلاجات غير الجراحية .
- الألم الشديد لفترة طويلة من الزمن.
- اعتلال الجذور، وهو مصطلح طبي يستخدم لوصف الألم والخدر والوخز في الذراعين أو الساقين.
- فقدان الإحساس في الذراعين أو الساقين.
- انخفاض القوة المحركة في الذراعين أو الساقين.
- فقدان السيطرة على الامعاء أو المثانة (متلازمة ذيل الفرس، على سبيل المثال).
أحد الأهداف الرئيسية لجراحة تضيق العمود الفقري في الرقبة أو أسفل الظهر هو تحرير منطقة الحبل الشوكي و/ أو جذور الأعصاب. هذا يسمى تخفيف الضغط.
من خلال منح الحبل الشوكي وجذور الأعصاب مساحة أكبر للمرور من خلالها، يأمل جراح العمود الفقري في تقليل الألم الناتج عن التهاب الأعصاب.
الهدف الآخر من جراحة تضيق العمود الفقري هو زيادة القوة الحركية في الذراعين أو الساقين. إذا فقدت الإحساس في ذراعيك أو ساقيك، يأمل جراحك أيضًا في استعادة ذلك.
أنواع جراحة تضيق العمود الفقري
عادة يستعمل الجراحون تقنيتين جراحيتين لجراحة تضيق العمود الفقري:
- إزالة أو تخفيف الضغط: يقوم الجراح بإزالة الأنسجة التي تضغط على البنية العصبية، مما يوفر مساحة أكبر في القناة الشوكية (للحبل الشوكي) أو في الثقبة (لجذور الأعصاب).
- التثبيت: يعمل الجراح على الحد من الحركة بين الفقرات.
أولاً: جراحة تخفيف الضغط لعلاج تضيق العمود الفقري
لإزالة النسيج الذي يضغط على العصب، قد يُجري جراح العمود الفقري أحد أنواع الجراحات التالية:
-
بضع الثقبة الفقرية:
إذا كان جزء من القرص أو نتوء عظمي (نبتة عظمية) يضغط على العصب عند خروجه من الفقرة (من خلال مخرج يسمى الثقبة الفقرية)، يمكن إجراء بضع الثقبة (foraminotomy). تعني “فتح نافذة”.
لذا فإن شق الثقبة يجعل فتحة الثقبة أكبر، بحيث يمكن للعصب الخروج دون أن ينضغط.
-
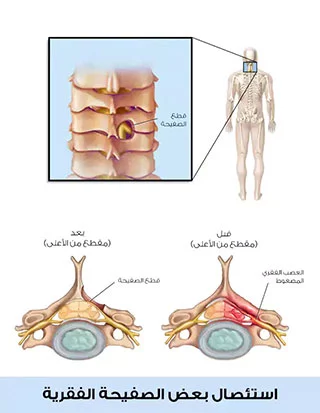
شق الصفيحة الفقرية:
على غرار بضع الثقبة، فإن شق الصفيحة الفقرية يخلق فتحة أكبر ولكن في الصفيحة العظمية هذه المرة, حيث أنه قد تضغط الصفيحة الفقرية على العصب، لذلك قد يوفر الجراح مساحة أكبر للأعصاب عند استخدام شق الصفيحة الفقرية.
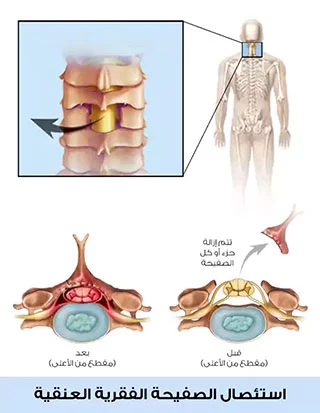
استئصال الصفيحة الفقرية
والذي يشبه إلى حد كبير جراحة الديسك بواسطة المجهر: حيث أنه في بعض الأحيان قد لا يكفي شق الصفيحة الفقرية.
قد يحتاج الجراح إلى إزالة كل أو جزء من الصفيحة، وهذا الإجراء يسمى استئصال الصفيحة الفقرية.
يمكن القيام بذلك في كثير من الأحيان على مستويات عديدة دون أي آثار ضارة.
يعتبر تخفيف الضغط غير المباشر أحد أشكال جراحة تخفيف الضغط حيث يتم تخفيف الضغط عن طريق فصل العظام عن بعضها بدلاً من إزالة العظام بواسطة الأقراص الاصطناعية.
يمكن القيام بذلك باستخدام الأجهزة التي توضع بين الفقرات.
حيث أن الأقراص الاصطناعية يمكنها ايضاً تخفيف الضغط عن طريق استعادة الارتفاع بين الفقرات المجاورة.
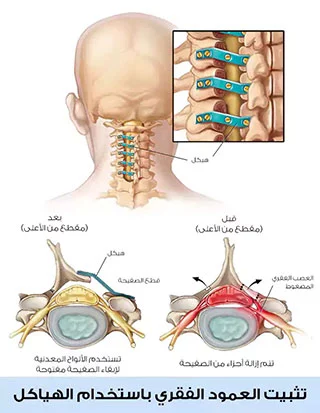
ثانياً: جراحة التثبيت لعلاج تضيق العمود الفقري
لا يحتاج كل من سيخضع لعملية جراحة تضيق العمود الفقري إلى التثبيت، والذي يُعرف أيضًا باسم دمج العمود الفقري.
إنه مفيد بشكل خاص في الحالات التي تنزلق فيها فقرة أو أكثر من الموضع الصحيح، مما يجعل العمود الفقري غير مستقر (ومؤلماً).
في هذه الحالات، يمكن أن يؤدي انزلاق العظام إلى الضغط على الأعصاب.
تعتمد الحاجة إلى التثبيت أيضًا على عدد الفقرات التي يحتاج الجراح للعمل عليها.
على سبيل المثال، إذا كان يحتاج إلى إزالة الصفيحة (باستخدام استئصال الصفيحة الفقرية) في فقرات متعددة، فقد يكون العمود الفقري غير مستقر بدون هذه الهياكل.
ستكون هناك حاجة إلى اجراء التحام في العمود الفقري للمساعدة في تثبيته.
كانت جراحة تثبيت العمود الفقري شائعة لسنوات عديدة.
يمكن إجراؤها بمفردها أو في نفس وقت جراحة تخفيف الضغط.
في عملية تثبيت العمود الفقري، يقوم الجراح بإنشاء بيئة تلتحم فيها عظام العمود الفقري معًا بمرور الوقت (عادةً على مدار عدة أشهر أو أكثر).
يستخدم الجراح طعمًا عظميًا (عادةً باستخدام عظام من جسمك) أو مادة بيولوجية (تحفز نمو العظام).
قد يستخدم الجراح أدوات العمود الفقري (الأسلاك والكابلات والبراغي والقضبان واللوحات) لزيادة الثبات والمساعدة في دمج العظام
. سيوقف الاندماج الحركة بين الفقرات، مما يوفر ثباتًا طويل المدى.
جراحة العمود الفقري المفتوحة أم جراحة العمود الفقري قليلة التوغل؟
إذا تم إجراء الجراحة من خلال شق كبير نسبيًا في ظهرك، فهذا يسمى الجراحة المفتوحة. هناك خيار آخر هو الجراحة قليلة التوغل، والتي تتم من خلال عدة شقوق صغيرة. قد يستخدم الجراح مجهرًا أو منظارًا داخليًا أو كاميرا دقيقة وأدوات جراحية صغيرة جدًا.
ومع ذلك، فإن الجراحة طفيفة التوغل ليست مناسبة للجميع. إذا احتاج جراحك إلى العمل على العديد من الفقرات، فربما تحتاج إلى إجراء عملية جراحية مفتوحة.
يجب على المريض أن يكون على دراية بالمخاطر الجراحية
كما هو الحال مع أي عملية جراحية، هناك مخاطر مرتبطة بجراحة تضيق العمود الفقري. سيناقش الطبيب المخاطر المحتملة معك قبل أن يطلب منك التوقيع على استمارة موافقة جراحية. تشمل المضاعفات المحتملة، على سبيل المثال لا الحصر:
- المخاطر العامة للتخدير
- إيذاء الحبل الشوكي أو الأعصاب
- عدم شفاء الانصهار العظمي (داء مفصلي كاذب)
- فشل في التحسن.
- كسر / فشل الأدوات التي يضعها الجراح (البراغي، الصفائح، القضبان، الاسلاك)
- عدوى و/ أو ألم موقع الطعم العظمي
الشفاء من جراحة تضيق العمود الفقري
بعد الجراحة، لن تتحسن على الفور. من المرجح أن تنهض من السرير في غضون 24 ساعة، وستتناول مسكنات الألم لمدة 2 إلى 4 أسابيع. بعد الجراحة، ستتلقى تعليمات حول كيفية الجلوس والقيام والوقوف بعناية.
من المهم أن تمنح جسمك وقتًا للشفاء، لذلك من المحتمل أن يوصي طبيبك بتقييد أنشطتك.
بشكل عام، لا تفعل أي شيء يحرك عمودك الفقري كثيرًا.
يجب أن تتجنب الرياضات التي تتطلب الاحتكاك الجسدي أو الالتواء أو رفع الأثقال أثناء فترة التعافي.
بعد الجراحة، كن يقظًا. أبلغ طبيبك عن أي مشاكل – مثل الحمى أو زيادة الألم أو العدوى – على الفور.
يجب عليك دائمًا الاعتناء بجسمك وممارسة العادات الصحية، ولكن يجب أن تكون بصحة جيدة بعد الجراحة بشكل خاص. لذلك يجب عليك:
- اتباع خطة طبيبك العلاجية.
- الجلوس والوقوف بشكل صحيح.
- تعلم رفع الاشياء بشكل صحيح.
- ممارسة الرياضة بانتظام (التمارين الخفيفة خصوصاً تعتبر جيدة، ولكن استشر طبيبك أولاً).
- استخدام المعدات الرياضية المناسبة.
- الوصول إلى وزن صحي والحفاظ عليه.
- تناول الأطعمة الصحية (نظام غذائي متوازن وقليل الدسم وغني بالفواكه والخضروات) والحصول على ما يكفي من الكالسيوم.
- التوقف عن التدخين.
- تجنب الاستخدام المفرط للمشروبات الكحولية.
عادةً ما تكون نتائج الجراحة لتصحيح تضيق العمود الفقري جيدة. بشكل عام فإن 80% إلى 90% من المرضى يشفون من آلامهم بعد الجراحة.
حيث تقول معظم الدراسات أن نتائج العملية تكون جيدة جداً في الحالات الشديدة في حال يفضل العلاج الفيزيائي في الحالات الخفيفة والمتوسطة.